Oncology
Abstract
Epigenetic macromolecular enzyme complexes tightly regulate gene expression at the chromatin level and have recently been found to colocalize with RNA splicing machinery during active transcription; however, the precise functional consequences of these interactions are uncertain. Here, we identify unique interactions of the CoREST repressor complex (LSD1-HDAC1-CoREST) with components of the RNA splicing machinery and their functional consequences in tumorigenesis. Using mass spectrometry, in vivo binding assays, and cryo-EM we find that CoREST complex-splicing factor interactions are direct and perturbed by the CoREST complex selective inhibitor, corin, leading to extensive changes in RNA splicing in melanoma and other malignancies. Moreover, these corin-induced splicing changes are shown to promote global effects on oncogenic and survival-associated splice variants leading to a tumor-suppressive phenotype. Using machine learning models, MHC IP-MS, and ELISpot assays we identify thousands of neopeptides derived from unannotated splice sites which generate corin-induced splice-neoantigens that are demonstrated to be immunogenic in vitro. Corin is further shown to reactivate the response to immune checkpoint blockade, effectively sensitizing tumors to anti-PD1 immunotherapy. These data position CoREST complex inhibition as a unique therapeutic opportunity which perturbs oncogenic splicing programs while also creating tumor-associated neoantigens that enhance the immunogenicity of current therapeutics.
Authors
Robert J. Fisher, Kihyun Park, Kwangwoon Lee, Katarina Pinjusic, Allison Vanasse, Christina S. Ennis, Parisa Farokh, Scott B. Ficarro, Jarrod A. Marto, Hanjie Jiang, Eunju Nam, Stephanie Stransky, Joseph Duke-Cohan, Melis A. Akinci, Anupa Geethadevi, Eric Raabe, Ana Fiszbein, Shadmehr Demehri, Simone Sidoli, Chad W. Hicks, Derin B. Keskin, Catherine J. Wu, Philip A. Cole, Rhoda M. Alani
Abstract
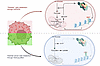
Enhanced lipid metabolism, which involves the active import, storage, and utilization of fatty acids from the tumor microenvironment, plays a contributory role in malignant glioma transformation; thereby, serving as an important gain of function. In this work, through studies initially designed to understand and reconcile possible mechanisms underlying the anti-tumor activity of a high-fat ketogenic diet, we discovered that this phenotype of enhanced lipid metabolism observed in glioblastoma may also serve as a metabolic vulnerability to diet modification. Specifically, exogenous polyunsaturated fatty acids (PUFA) demonstrate the unique ability of short-circuiting lipid homeostasis in glioblastoma cells. This leads to lipolysis-mediated lipid droplet breakdown, an accumulation of intracellular free fatty acids, and lipid peroxidation-mediated cytotoxicity, which was potentiated when combined with radiation therapy. Leveraging this data, we formulated a PUFA-rich modified diet that does not require carbohydrate restriction, which would likely improve long-term adherence when compared to a ketogenic diet. The modified PUFA-rich diet demonstrated both anti-tumor activity and potent synergy when combined with radiation therapy in mouse glioblastoma models. Collectively, this work offers both a mechanistic understanding and a potentially translatable approach of targeting this metabolic phenotype in glioblastoma through diet modification and/or nutritional supplementation that may be readily integrated into clinical practice.
Authors
Shiva Kant, Yi Zhao, Pravin Kesarwani, Kumari Alka, Jacob F. Oyeniyi, Ghulam Mohammad, Nadia Ashrafi, Stewart F. Graham, C. Ryan Miller, Prakash Chinnaiyan
Abstract
Glycolysis fuels cytotoxic allogeneic T cells in acute graft-versus-host disease (aGvHD), but the downstream role of glucose metabolism in modulating aGvHD remains unclear. Targeting glycolysis or glucose receptors is toxic. Therefore, we explored alternative glucose-dependent pathways, focusing on the pentose phosphate pathway (PPP). Single-cell RNA sequencing revealed PPP upregulation in allogeneic T cells during allogeneic hematopoietic cell transplantation (allo-HCT). We showed that donor T cell deficiency in 6-phosphogluconate dehydrogenase (6PGD), the second rate-limiting enzyme in the PPP, significantly reduced aGvHD severity and mortality in murine models. Functional assays demonstrated that PPP blockade led to proliferation arrest without inducing apoptosis. PPP blockade shifted T cell metabolism away from T cell dependency on glycolysis for rapid T cell proliferation. Pharmacological inhibition of the PPP through 6PGD blockade with 6-aminonicotinamide (6AN) effectively reduced aGvHD severity, like donor 6PGD-deficient T cells in an allogeneic aGvHD model. Similarly, 6AN reduced xenogeneic GvHD lethality. 6PGD inhibition preserved the graft-versus-tumor (GvT) effect, with the generation of a small subset of granzyme Bhi effector T cells with potent antitumor activity. These findings highlight the PPP as a key regulator of allogeneic T cell proliferation and differentiation and identify 6PGD as a promising therapeutic target to mitigate aGvHD severity while preserving beneficial GvT effects.
Authors
Saeed Daneshmandi, Eun Ko, Qi Yan, Jee Eun Choi, Prashant K. Singh, Richard M. Higashi, Andrew N. Lane, Teresa W.M. Fan, Jingxin Qiu, Sophia Hani, Keli L. Hippen, Jianmin Wang, Philip L. McCarthy, Bruce R. Blazar, Hemn Mohammadpour
Abstract
Over 95% of head and neck cancers are squamous cell carcinoma (HNSCC). HNSCC is mostly diagnosed late, causing a poor prognosis despite the application of invasive treatment protocols. Tumor-educated platelets (TEPs) have been shown to hold promise as a molecular tool for early cancer diagnosis. We sequenced platelet mRNA isolated from blood of 101 HNSCC patients and 101 propensity-score matched non-cancer controls. Two independent machine learning classification strategies were employed using a training and validation approach to identify a cancer predictor: a particle swarm optimized support vector machine (PSO-SVM) and a least absolute shrinkage and selection operator (LASSO) logistic regression model. The best performing PSO-SVM predictor consisted of 245 platelet transcripts and reached a maximum area under the curve (AUC) of 0.87. For the LASSO-based prediction model 1,198 mRNAs were selected, resulting in an median AUC of 0.84, independent of HPV status. Our data show that TEP RNA classification by different AI tools is promising in the diagnosis of HNSCC.
Authors
N.E. Wondergem, J.B. Poell, S.G.J.G In 't Veld, E. Post, S.W. Mes, M.G. Best, W.N. van Wieringen, T. Klausch, R.J. Baatenburg de Jong, C.H.J. Terhaard, R.P. Takes, J.A. Langendijk, I.M. Verdonck-de Leeuw, F. Lamers, C.R. Leemans, E. Bloemena, T. Würdinger, R.H Brakenhoff
Abstract
Immune checkpoint inhibitors (ICIs) such as anti-PD-1 and anti-CTLA-4 antibodies are used to induce an immune response against many types of tumors. However, ICIs often also induce autoimmune responses, referred to as immune-related adverse events (irAEs), which occur unpredictably and at varying levels of severity in ICI-treated patients. The immunologic factors that predispose patients to the development of severe irAE are largely unclear. Here, we utilized high dimensional mass cytometry immunophenotyping of longitudinal blood samples from patients with metastatic melanoma treated with combination anti-PD-1/CTLA4 ICI therapy in the context of a clinical trial to characterize alterations in immune profiles induced by combination ICI therapy and to identify immune features associated with development of severe irAEs. Deep T cell profiling highlighted that ICI therapy induces prominent expansions of activated, CD38hi CD4+ and CD8+ T cells, which are frequently bound by the therapeutic anti-PD-1 antibody, as well as substantial changes in regulatory T cell phenotypes. However, neither the baseline frequency nor the extent of expansion of these cell populations was associated with development of severe irAEs. Rather, single cell-association testing revealed naïve CD4+ T cell abundance pre-treatment as significantly associated with the development of severe irAEs. Biaxial gating of naïve CD4+ T cells confirmed a significant positive association of naïve CD4+ T cell proportion and development of a severe irAE and with the number of irAEs developed in this cohort. Results from this broad profiling study indicate the abundance of naïve CD4+ T cells as a predictive feature for the development of severe irAEs following combination anti-PD-1/CTLA4 ICI therapy.
Authors
Kathryne E. Marks, Alice Horisberger, Mehreen Elahee, Ifeoluwakiisi A. Adejoorin, Nilasha Ghosh, Michael A. Postow, Laura Donlin, Anne R. Bass, Deepak A. Rao
Abstract
Survival in chronic myeloid leukemia (CML) was dramatically improved by development of tyrosine kinase inhibitors (TKIs) directed to the BCR::ABL1 oncogene. Unfortunately, ~30% of CML patients develop TKI-resistance during prolonged treatment, with enhanced blast crisis risk. Oxidation Resistance 1 (Oxr1) regulates anti-oxidant pathways that detoxify reactive oxygen species (ROS) generated by the phagocyte-NADPH oxidase. In the current studies, we found that Oxr1 expression increased in hematopoietic stem and progenitor cells (HSPCs) from CML mice versus controls; decreased during TKI-induced remission; and rose during chronic phase relapse. Oxr1 has long and short isoforms, and we found increased short, but decreased long, Oxr1 in mice or humans during CML relapse. We determined long Oxr1 prevents ROS accumulation in CML marrow, but short Oxr1 is a dominant negative. Previously, we found exaggerated and sustained emergency granulopoiesis in CML mice, with repeated episodes facilitating relapse during TKI-remission. In the current studies, we found knocking-down Oxr1 in murine marrow further accelerates CML progression during this physiologic stress. We found increased DNA-damage in HSPCs from these mice, including a BCR::ABL1 kinase-domain mutation found in TKI-resistant human CML. These studies suggest long Oxr1 detoxifies ROS to decrease mutagenesis in CML, but aberrant short Oxr1 expression enhances progression.
Authors
weiqi huang, Bin Liu, Liping Hu, Chi-Hao Luan, Priyam Patel, Elizabeth T. Bartom, Elizabeth A. Eklund
Abstract
Glioblastoma (GBM) is an aggressive brain tumor that often progresses despite resection and treatment. Timely and continuous assessment of GBM progression is critical to expedite secondary surgery or enrollment in clinical trials. However, current progression detection requires costly and specialized magnetic resonance imaging (MRI), which, in the absence of new symptoms or signs, is usually scheduled every 2 to 3 months. Here, we hypothesized that changes in daily activity associate with GBM growth and disease progression. We found that wheel-running activity in GBM-bearing mice declined as tumors grew, and preceded weight loss and circadian breakdown by over a week. Temozolomide treatment in the morning, but not evening, significantly reduced tumor size and restored daily locomotion in mice. In a pilot study of six GBM patients wearing an actigraphy watch, wrist movement provided a feasible and continuous longitudinal indicator of daily activity with one-minute resolution. Following tumor resection and radiation, daily activity declined in two patients 19 and 55 days before detection of progression by MRI, but did not change for the four patients with stable disease. These results suggest that daily activity tracking using wearable devices may serve as a real-time indicator and potential monitoring tool for GBM progression and treatment efficacy.
Authors
Maria F. Gonzalez-Aponte, Sofia V. Salvatore, Anna R. Damato, Ruth G.N. Katumba, Grayson R. Talcott, Omar H. Butt, Jian L. Campian, Jingqin Luo, Joshua B. Rubin, Olivia J. Walch, Erik D. Herzog
Abstract
Therapeutics blocking PI3K/mTOR complex 1 (mTORC1) are commonly used for tumor treatment, and at times achieve major responses, yet minimal residual disease (MRD) persists, leading to tumor relapse. We developed multiple MRD models both in vitro (rapamycin persistent, RP) and in vivo after mTORC1 inhibition. All 11 RP/MRD cell lines showed complete growth and signaling insensitivity to rapamycin but variable sensitivity to bi-steric mTORC1 inhibitors, with MtorS2035 mutations identified in 4 of 7 RP cell lines. Multiomic analyses identified a pronounced shift toward oxidative phosphorylation and away from glycolysis with increased mitochondrial number in all RP/MRD models. MYC and SWI/SNF expression was significantly enhanced. Both the SWI/SNF inhibitor AU-15330 and the mitochondrial complex I oxidative phosphorylation inhibitor IACS-010759 showed pronounced synergy with bi-steric mTORC1 inhibitors to cause cuproptotic cell death in RP/MRD cells, suggesting these combinations as a potential patient treatment strategy for rapalog resistance.
Authors
Heng Du, Heng-Jia Liu, Magdalena Losko, Yu Chi Yang, Min Yuan, Elizabeth P. Henske, John M. Asara, Mallika Singh, David J. Kwiatkowski
Abstract
HOXB13 is a prostate-specific transcription factor best known for its role as an androgen receptor (AR) cofactor. Recent evidence suggests that HOXB13 plays critical AR-independent functions in repressing lipogenic programs and promoting prostate cancer (PCa) metastasis. However, the mechanisms linking HOXB13 loss to tumor metastasis remain unclear. Here, we show that p300 and CBP co-occupy lipogenic enhancers suppressed by HOXB13 and HDAC3 and are essential for enhancer activation and target gene expression following HOXB13 depletion. Loss of HOXB13 induces lipid-sensitive matrix metalloproteinases (MMPs), promoting increased cell motility. Importantly, pharmacological inhibition of p300 and CBP blocks HOXB13-loss-driven lipogenesis, reduces MMP expression, and decreases cell migration in vitro and tumor metastasis in vivo. Analysis of clinical samples revealed that HOXB13 expression is reduced in metastatic hormone-sensitive PCa compared with matched primary tumors, further supporting its role in tumor metastasis. These findings demonstrate that HOXB13 downregulation promotes PCa metastasis through p300- and CBP-dependent lipogenic and motility pathways, which may be targeted by p300 inhibition.
Authors
Xiaodong Lu, Liu Peng, Qi Chu, Samantha Ye, Mingyang Liu, Maha Hussain, Mehmet A. Bilen, Lara R. Harik, Jonathan Melamed, Jonathan C. Zhao, Jindan Yu
Abstract
Patients with cutaneous T cell lymphoma (CTCL) experience high morbidity and mortality due to S. aureus skin infections and sepsis, but the underlying mechanisms remain unclear. We have previously identified high levels of LAIR2, a decoy protein for the inhibitory receptor LAIR1, in advanced CTCL. Mice lack a LAIR2 homolog, so we used Lair1 knock-out (KO) mice to model LAIR2 overexpression. In a model of S. aureus skin infection, Lair1 KO mice had significantly larger abscesses and areas of dermonecrosis compared to WT despite similar bacterial burdens. Lair1 KO exhibited a pattern of increased inflammatory responses in infection and sterile immune stimulation, with increased production of proinflammatory cytokines and myeloid chemokines, neutrophil ROS, and collagen/ECM pathway proteins, including collagens and complement factors. These findings support the notion that loss of LAIR1 signaling causes an excessive inflammatory response that exacerbates tissue damage and does not improve infection control. Underscoring the clinical relevance of our findings, CTCL skin lesions exhibited similarly increased expression in cytokine and collagen/ECM remodeling pathways, suggesting that high levels of LAIR2 promote excessive inflammatory tissue damage and compromise host defense against S. aureus infection. LAIR signaling represents a promising target for therapeutic development in CTCL and other inflammatory diseases.
Authors
Hannah K. Dorando, Evan C. Mutic, Kelly L. Tomaszewski, Yulia Korshunova, Ling Tian, Mellisa K. Stefanov, Chaz C. Quinn, Deborah J. Veis, Juliane Bubeck Wardenburg, Amy C. Musiek, Neha Mehta-Shah, Jacqueline E. Payton
No posts were found with this tag.