Vascular biology
Abstract
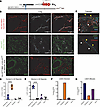
Vascular tortuosity (VT) is a critical biomarker of disease progression and decision to treat ischemic retinal disorders, particularly retinopathy of prematurity (ROP). The murine oxygen-induced retinopathy model is the most widely-used model of ischemic retinopathy. Although VT has been described in OIR, its temporal dynamics have not been systematically defined. In this study, a semi-automated artificial intelligence (AI)-based pipeline was used to quantify VT throughout OIR. Retinal flat mounts from age-matched normoxic and OIR mice (postnatal days [P]10-P56) underwent vessel segmentation using a generative adversarial network (GAN), and VT was quantified as a cumulative tortuosity index (CTI) with the iROP-Assist algorithm. Concurrently, standard OIR outcomes of neovascularization (NV) and vaso-obliteration (VO) were quantified using OIRseg.org. NV peaked at P17 and resolved by P23, while VO regressed over a similar interval. VT peaked with NV at P17 but remained elevated through P56. These temporal changes mirror both the development of VT and its persistence after NV regression observed clinically in ROP. Collectively, these findings establish VT as a durable, quantifiable phenotype in OIR and expand the model’s utility beyond neovascular endpoints, providing a translational platform for investigating VT pathogenesis and evaluating the effects of therapeutic agents on vascular tortuosity.
Authors
Kyle V. Marra, Tomoya Murakami, Jimmy S. Chen, Edith Aguilar, Jacob I. Robinson, Maxwell Prenner, Richard Daneman, Martin Friedlander, Eric Nudleman
Abstract
Spreading depolarizations (SDs) are propagating waves of near-complete breakdown of transmembrane ion gradients that occur during acute ischemic stroke and worsen outcome by driving calcium overload and glutamate release in neurons and astrocytes. The plasmalemmal sodium-calcium exchanger (NCX) plays a key role in such changes, in that the complex ionic disequilibrium during ischemia induces reverse-mode activity of NCX, leading to cellular calcium overload in exchange for sodium. However, the cell type-specific roles of NCX in neurons and astrocytes during SDs remain unclear. Here, we used ion and glutamate reporters in an in vivo stroke model in mice carrying inducible, cell-specific deletions of NCX isoform-1. Neuronal NCX1 deletion reduced neuronal and astrocytic calcium transients, increased neuronal sodium transients, decreased extracellular glutamate levels, and raised SD initiation threshold. In contrast, astrocytic NCX1 deletion increased sodium transients in both neurons and astrocytes, and increased neuronal calcium as well as extracellular glutamate levels. A computational model of ischemia confirmed that these effects are consistent with reverse-mode NCX1 activity. Together, these findings indicate opposing roles of reverse-mode NCX1 during ischemia. Neuronal NCX1 promotes SD susceptibility, calcium overload and glutamate release, whereas astrocytic NCX1 exerts protective effects by attenuating glutamate elevation and neuronal calcium accumulation.
Authors
Somayyeh Hamzei Taj, Pawan Kumar Thapaliya, Cordula Rakers, Niklas J. Gerkau, Christine R. Rose, Ghanim Ullah, Gabor C. Petzold
Abstract
Idiopathic Pulmonary Fibrosis (IPF) is a fatal, aging-related disease characterized by persistent lung fibroblast activation, progressive lung scarring and several vascular abnormalities. We have previously demonstrated that aging-associated vascular dysfunction drives maladaptive endothelial responses to injury and exacerbates lung fibrosis via secretion of pro-fibrotic endothelial-derived factors. However, regulatory mechanisms governing endothelial dysfunction during progressive lung fibrosis remain poorly understood. Here, using preclinical mouse models of progressive lung fibrosis as well as human IPF lungs, we demonstrate that miR-205-5p is overexpressed in lung ECs from fibrotic lungs, and coordinates gene expression programs implicated in endothelial dysfunction and progressive fibrosis. Mechanistically, miR-205-5p induces senescence in lung ECs, mirroring the senescent phenotype of IPF lung ECs. Consistently, conditioned medium derived from lung ECs overexpressing miR-205-5p promotes lung fibroblast activation. Importantly, miR-205-5p inhibition in IPF lung ECs attenuates endothelial senescence and limits paracrine fibroblast activation. Finally, inhibition of miR-205-5p in vivo preserves the pulmonary vascular network and attenuates lung fibrosis progression in aged mice challenged with bleomycin. Collectively, our findings support a novel connection between lung endothelial miR-205-5p, endothelial senescence and pro-fibrotic alteration of the endothelial secretome, and highlight miR-205-5p inhibition as a potential therapeutic intervention for pulmonary fibrosis.
Authors
Giuseppe Muscato, Benjamin B. Roos, Sharonda Harris, Xiaoyu Tracy Cai, Gina Civettini, Enrico Sciacca, Ahmed Raslan, Alessandra Castaldi, Sharon Elliot, Marilyn K. Glassberg, Carlo Vancheri, Daniel J. Tschumperlin, Giovanni Ligresti, Nunzia Caporarello
Abstract
Authors
Sarah Platt, Norhan B.B. Mohammed, Joseph Brancale, Caroline S.C. Tippett, Kevin Seo, Silvia Vilarinho
Abstract
Kawasaki disease (KD) is an acute febrile systemic vasculitis of unknown etiology and the leading cause of acquired heart disease among children. Complement activation has long been observed in patients with acute KD, however, its contribution to disease development remains unknown. Here, using publicly available datasets, we showed that patients with acute KD exhibited higher expression of complement products in whole blood, consistent with the activation of the complement pathway. Similarly, in the Lactobacillus casei cell wall extract (LCWE) murine model of KD, LCWE injection induced increased expression of complement products in cardiovascular tissues, suggestive of activation of the complement pathways. C3-deficient mice or WT mice treated with the complement C5a Receptor 1 (C5ar1) antagonist developed significantly more severe LCWE-induced cardiovascular lesions and vasculitis. Furthermore, we observed that LCWE binds to serum C3, an opsonizing factor that labels microbial targets for clearance, and LCWE deposition in the liver was significantly higher in C3-deficient mice compared to WT mice. Overall, our data indicate that blocking the complement system significantly exacerbates LCWE-induced KD vasculitis, likely by impairing C3-mediated clearance of LCWE. These data suggest that the complement pathway may play a protective role in KD pathogenesis by promoting clearance of potential bacterial or viral trigger of KD.
Authors
Asli E. Atici, Begüm Kocatürk, Benjamin L. Ross, Emily A. Aubuchon, Rebecca A. Porritt, Thacyana T. Carvalho, Takahiro Namba, Youngho Lee, Magali Noval Rivas, Moshe Arditi
Abstract
Lung IL-33 is involved in pathogen defense, barrier homeostasis, and development of allergic responses. We previously identified a 5 kb noncoding region within a GWAS-defined segment that regulates expression of human IL33 (hIL33) but is absent in the murine locus. To understand how this region affects IL-33 expression in vivo, we engineered 2 BAC-transgenic strains in which 166 kb of the human genome upstream of the hIL33 locus, along with a fluorescent reporter, was inserted into the murine genome, both with and without the 5 kb region. Comparison to a murine Il33 (mIl33) reporter strain revealed species-specific tropism; hIL33 reporter was mostly expressed in the endothelium, while mIl33 reporter was expressed in type 2 alveolar epithelium. hIL33 reporter expression in tracheal basal epithelium, submucosal glands, and lung microvasculature required the 5 kb region. Surprisingly, allergen and exogenous IL-33 downregulated hIL33 reporter in lung endothelium only when the 5 kb region was present. Similar IL-33–dependent downregulation of IL33 transcripts was observed in human endothelial cell lines, validating that our hIL33 reporter strain recapitulated human endothelial biology. Together, these data reveal the importance of the asthma-associated human 5 kb region in regulating human IL33 expression in a cell type– and context-dependent manner.
Authors
Maile K. Hollinger, Chanie L. Howard, Donna C. Decker, Kelly M. Blaine, Ivy Aneas, Emily M. Grayson, Tania E. Velez, Fernando A. Oliveira, Riley T. Hannan, Daniel F. Camacho, Philip A. Verhoef, Cara L. Hrusch, Rebecca S. Griffes, Jeffrey M. Sturek, Marcelo A. Nobrega, Nathan Schoettler, Anne I. Sperling
Abstract
Single-ventricle congenital heart disease (SV-CHD) is a uniformly lethal condition requiring the Glenn surgery, which as a side effect eliminates arterial pulsatility and contributes to pulmonary vascular complications. In Glenn patients, we quantified pulsatility loss in each dimension of force (flow, pressure, and stretch) using cardiac catheterization and MRI. To model and investigate the individual impact of each dimension of pulsatility loss on the pulmonary vasculature, we applied isolated pulsatile and non-pulsatile mechanical stimuli to pulmonary artery endothelial cells (ECs) in vitro. We found that each dimension of force triggered distinct transcriptional responses, revealing force-specific regulation of structural and signaling pathways. Pulsatile stretch uniquely stimulated EC secretion of PDGFB, a key driver of vascular smooth muscle cell (vSMC) recruitment. In a rat Glenn model, loss of pulsatility led to vascular wall thinning, loss of EC PDGFB, and reduced activation of smooth muscle PDGFBRβ, confirming in vivo relevance. Our findings uncover a mechanistic link between endothelial stretch sensing and PDGFB-mediated EC-vSMC crosstalk, essential for maintaining pulmonary artery architecture. Clinically, these insights suggest that restoring or mimicking pulsatile forces may help preserve vascular integrity and prevent remodeling in patients with SV-CHD.
Authors
Stephen B. Spurgin, Lauren Thai, Tina C. Wan, Christopher P. Chaney, Mitzy A. Cowdin, Surendranath Veeram Reddy, Tarique Hussain, Munes Fares, M. Luisa Iruela-Arispe, Thomas Carroll, Andrew D. Spearman, Ondine Cleaver
Abstract
Glaucoma is associated with ocular hypertension, and lowering intraocular pressure is the primary objective of current therapies. Recent studies have established a key role for Schlemm’s canal endothelium in this pressure increase and have shown that it has a unique, lymphatic-like hybrid phenotype characterized by expression of the lymphatic transcription factor PROX1. However, the functional importance of this hybrid phenotype in the adult canal remains unclear, as long-term studies have been limited by systemic requirements for lymphatic gene expression and a lack of Schlemm’s canal–specific animal models. Here, we designed and validated a strategy using 4OH-tamoxifen-loaded nanocarriers to generate targeted, Schlemm’s canal-specific Prox1 knockout mice that specifically lacked lymphatic characteristics in the canal endothelium. Within four weeks, intraocular pressure was significantly elevated, and ocular hypertension was maintained for at least 24 weeks. Unlike lymphatic vessels, which degenerate following Prox1 deletion, Schlemm’s canal persisted but reverted to a less functional vein-like phenotype with no change in size or morphology. Together, these findings demonstrate the utility of nanocarrier-mediated tamoxifen delivery and establish the importance of the Schlemm’s canal lymphatic-like phenotype in intraocular pressure regulation, providing targets for future glaucoma therapies and a mouse model of adult-onset ocular hypertension.
Authors
Sofia Lara Ochoa, Hoi-Lam Li, Hyeohn Kim, Zihang Yan, Natalia C. Mendonca, Pan Liu, Hyunjoo J. Lee, Michael P. Vincent, Sultan Almunif, Hao F. Zhang, Haiyan Gong, Evan A. Scott, Mark Johnson, Benjamin R. Thomson
Abstract
In metabolic dysfunction-associated steatohepatitis (MASH), liver sinusoidal endothelial cells (LSECs) acquire a proinflammatory phenotype termed lipotoxic endotheliopathy. We previously identified glycogen synthase kinase 3β (GSK3β) as a central signaling hub in LSECs during MASH. To elucidate the molecular mechanisms and functional outcome of lipotoxicity-induced GSK3β activation in LSECs, we utilized endothelial cell-specific Gsk3β knockout (Gsk3β△End) mice fed MASH-inducing diets. Endothelial Gsk3β deletion significantly reduced markers of lipotoxic endotheliopathy, including adhesion molecules and chemokines, alongside liver injury, inflammation, and fibrosis. Immune profiling via flow cytometry and mass cytometry by time of flight (CyTOF) identified decreased hepatic infiltration of proinflammatory myeloid populations, particularly mature dendritic cells (DCs) in Gsk3β△End mice. In a co-culture system, GSK3β in lipotoxic LSECs promoted DCs maturation. Mechanistically, GSK3 inhibition restored lipotoxicity-induced alterations in LSEC mitochondrial morphology and respiration by regulating AMP-activated protein kinase and dynamin-related protein 1. This rescue suppressed chemokines and adhesion molecules expression, thereby limiting immune cell recruitment. Collectively, under lipotoxic stress, GSK3β amplifies mitochondrial dysfunction and inflammatory signaling in LSECs, enhancing myeloid cell homing and DC maturation. Targeting LSEC GSK3β may therefore represent a promising therapeutic strategy to mitigate LSEC driven fibro inflammatory response in human MASH.
Authors
Akitoshi Sano, Qianqian Guo, Khaled Warasnhe, Chady Meroueh, Nantawat Satthawiwat, Asma Hamdi, Ghefar Hmaydoosh, Xin Dai, Usman Yaqoob, Kevin D. Pavelko, Charlene Miciano, Tatiana Kisseleva, Zeba Firdaus, Patrick P. Starlinger, David Pereyra, Enis Kostallari, Petra Hirsova, Davide Povero, Samar H. Ibrahim
Abstract
Abdominal aortic aneurysm (AAA) lacks effective pharmacological therapies. Here, we investigate transcription factor 7-like 2 (TCF7L2), a genetic locus associated with both thoracic and abdominal aortic aneurysms, to elucidate its role in AAA pathogenesis. Integrating summary-data-based Mendelian randomization (SMR) with single-cell RNA sequencing (scRNA-seq) of human and mouse aortas, we identify TCF7L2 as a gene enriched in vascular smooth muscle cells (VSMCs) and causally linked to AAA development. Smooth muscle cell-specific TCF7L2 knockout significantly attenuates AAA formation across three distinct murine models (Ang II infusion-, BAPN/Ang II co-administration-, and elastase-induced AAA), independent of systemic blood pressure or lipid levels. Mechanistic studies reveal that TCF7L2 directly upregulates MMP14 and downregulates TIMP3 expression in vitro and in vivo, driving MMP2-mediated extracellular matrix (ECM) degradation. Concurrently, TCF7L2 represses integrin β1 (ITGB1) expression, reducing VSMC adhesion to the ECM. Collectively, these findings identify TCF7L2 as a key driver of pathological vascular remodeling in AAA, suggesting that targeting TCF7L2 may offer a novel therapeutic strategy for limiting AAA progression.
Authors
Yongjie Deng, Yaozhong Liu, Yang Zhao, Hongyu Liu, Guizhen Zhao, Zhenguo Wang, Xu Zhang, Chao Xue, Wei Huang, Tianqing Zhu, Haocheng Lu, Yanhong Guo, Lin Chang, Ida Surakka, Y. Eugene Chen, Jifeng Zhang
No posts were found with this tag.