Inflammation
Abstract
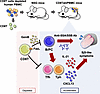
BACKGROUND Platelets are increasingly recognized as active participants in immune signaling and systemic inflammation. Upon activation, platelets form monocyte platelet aggregates (MPA) representing the crossroads of thrombosis and inflammation. We hypothesized that platelet transcriptomics could capture this thromboinflammatory axis and identify individuals at elevated cardiovascular risk.METHODS: MPA levels, defined as CD14+CD61+ cells, were measured using flow cytometry at 2 time points, 4 weeks apart, in healthy individuals Platelets were isolated and sequenced. Individuals were categorized as MPAhi or MPAlo based on consistently high or low MPA levels across time points.RESULTS Among 149 participants (median age 52 years, 57% female, 50% non-White), MPAhi individuals exhibited increased expression of platelet activation markers P-selectin (P < 0.001), PAC-1 (P = 0.021), and CD40L (P < 0.001) and enriched immune signaling pathways. Informed by MPA levels and derived from the platelet transcriptome, we developed a 42-gene thromboinflammation platelet signature (TIPS), which correlated with MPA levels in multiple cohorts and was reproducible over time. TIPS was elevated in patients with COVID-19 (P = 0.0002) and myocardial infarction (Padj = 0.008), and as in predicted future cardiovascular events in patients who underwent lower extremity revascularization after a median follow-up of 18 months (adjusted for age, sex, race, and ethnicity [adjHR] 1.55, P = 0.006). Notably, TIPS was modifiable by ticagrelor (P = 0.002) but not aspirin.CONCLUSION These findings establish MPA as a biomarker of thromboinflammation and introduce TIPS, a platelet RNA signature, that captures thromboinflammation and provides a promising tool for cardiovascular risk stratification and a potential therapeutic target.TRIAL REGISTRATION NCT04369664FUNDING NIH R35HL144993, NIH R01HL139909, and AHA 16SFRN2873002 to JSB, DFG Walter-Benjamin-Programme 537070747 to AB.
Authors
Antonia Beitzen-Heineke, Matthew A. Muller, Yuhe Xia, Elliot Luttrell-Williams, Florencia Schlamp, Deepak Voora, Kelly V. Ruggles, Michael S. Garshick, Tessa J. Barrett, Jeffrey S. Berger
Abstract
Oral lichen planus (OLP) is a recalcitrant inflammatory disease with potential for malignant transformation, involving a cytotoxic CD8+ T cells-mediated basal keratinocyte apoptosis. However, it lacks an appropriate mouse model for study. Here we developed an OLP-like mouse model using topical oxazolone to induce a delayed-type hypersensitivity-mediated oral lichenoid reaction. Histological and ultrastructural analysis confirmed hallmark pathological features of OLP, including band-like CD8+ T cell infiltration and basal cell damage, and the presence of Civatte bodies. Comparative transcriptomic analysis revealed significant similarity between RNA-seq profiles of the mouse model and human OLP lesions, highlighting shared upregulated genes and enriched pathways, particularly those related to IFN-γ signaling and cytotoxic T cell activity. Functional studies demonstrated that the OLP phenotype depended on IFN-γ, with local priming by IFN-γ intensifying the disease through upregulation of major histocompatibility complex class I. Additionally, the absence of Langerhans cells exacerbated disease severity in vivo. Therapeutic evaluation showed that the JAK inhibitors baricitinib and ruxolitinib effectively reduced disease burden and provided mechanistic insights. In conclusion, this OLP-like mouse model recapitulates key immunopathological and transcriptomic features of human OLP, offering a robust platform for dissecting disease mechanisms and evaluating novel therapeutic strategies.
Authors
Zhenlai Zhu, Tinglan Yang, Peng Peng, Kang Li, Wen Qin, Chen Zhang, Shuyan Wang, Yuanyuan Wang, Minghui Wei, Erle Dang, Meng Fu, Hao Guo, Wen Yin, Shuai Shao, Qing Liu
Abstract
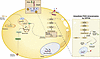
Mitochondrial dysfunction is a major mechanism of acute kidney injury (AKI), and increased circulating interleukin 6 (IL-6) is associated with systemic inflammation and death due to sepsis. We tested whether kidney mitochondrial DNA (mtDNA) contributes to IL-6 release in sepsis-associated AKI via Toll-like receptor 9 (TLR9). In a murine model of sepsis via cecal ligation and puncture (CLP), we used next-generation sequencing of plasma mtDNA to inform the design of optimal target sequences for quantification by droplet digital PCR, and to identify single-nucleotide polymorphisms (SNPs) to infer tissue origin. We found significantly higher concentrations of plasma mtDNA after CLP versus shams and that plasma mtDNA SNPs matched kidney SNPs more than other organs. Kidney mtDNA contributed directly to IL-6 and mtDNA release from dendritic cells in vitro and kidney mitochondria solution led to higher IL-6 concentrations in vivo. IL-6 release was mitigated by a TLR9 inhibitor. Finally, plasma mtDNA was significantly higher in septic patients with AKI compared with those without AKI and correlated significantly with plasma IL-6. We conclude that AKI contributes to increased circulating IL-6 in sepsis via mtDNA release. Targeting kidney mitochondria and mtDNA release are potential translational avenues to decrease mortality from sepsis-associated AKI.
Authors
Avnee J. Kumar, Katharine Epler, Jing Wang, Alice Shen, Negin Samandari, Mark L. Rolfsen, Laura A. Barnes, Gerald S. Shadel, Alexandra G. Moyzis, Alva G. Sainz, Karlen Ulubabyan, Kefeng Li, Kristen Jepsen, Xinrui Li, Mark M. Fuster, Roger G. Spragg, Roman Sasik, Volker Vallon, Helen Goodluck, Joachim H. Ix, Prabhleen Singh, Mark L. Hepokoski
Abstract
Sepsis is a life-threatening organ dysfunction caused by a dysregulated host response to infection. During early sepsis, kinins are released and bind to B1 (BDKRB1) and B2 (BDKRB2) bradykinin receptors, but the involvement of these receptors in sepsis remains incompletely understood. This study demonstrated that the genetic deletion of Bdkrb2 had no significant impact on sepsis induced by cecal ligation and puncture (CLP) compared to wild-type (WT) mice. In contrast, Bdkrb1−/− mice subjected to CLP exhibited decreased lethality and bacterial load, associated with an increased influx of neutrophils into the peritoneal cavity, compared with WT mice. Neutrophils from CLP-Bdkrb1−/− mice partially restored CXCR2 expression and reduced the upregulation of P110γ observed in WT CLP neutrophils. Pharmacologic inhibition of BDKRB1 combined with imipenem treatment substantially improved survival compared with antibiotic therapy alone. In human neutrophils, stimulation with LPS led to the upregulation of BDKRB1 expression, and antagonism of BDKRB1 restored neutrophil migration in response to CXCL8. These findings identify BDKRB1 as an important modulator of neutrophil dysfunction in sepsis and a promising therapeutic target whose inhibition improves bacterial clearance, restores neutrophil migration, and increases the efficacy of antibiotic treatment.
Authors
Raquel Duque do Nascimento Arifa, Carolina Braga Resende Mascarenhas, Lívia Caroline Resende Rossi, Maria Eduarda Freitas Silva, Larissa M. Lucas, João Paulo Pezzini Barbosa, Daiane Boff, Brenda Gonçalves Resende, Lívia Duarte Tavares, Alesandra Corte Reis, Vanessa Pinho, Flavio Almeida Amaral, Caio Tavares Fagundes, Cristiano Xavier Lima, Mauro Martins Teixeira, Daniele G Souza
Abstract
Peripheral helper T (Tph) and follicular helper T (Tfh) cells are key regulators of B cell differentiation and antibody production, making them promising targets for autoimmune disease treatment. However, their differentiation mechanisms differ significantly between humans and mice, limiting drug validation in mouse models. Here, we present a simple and effective method for in vivo proliferation of human Tph/Tfh and B cells. We discovered that after depleting CD8+ T cells of human peripheral blood mononuclear cell–transferred immunodeficient mice (CD8TΔhPBMC mice), human Tph/Tfh cells and B cells proliferated markedly in the spleen compared with those in human PBMC–transferred immunodeficient mice (hPBMC mice). Transcriptome analysis confirmed proliferating cells’ close resemblance to human Tph/Tfh cells. Furthermore, multicolor flow cytometry revealed CXCL13+ Tph cells infiltrating Sjögren’s syndrome–associated (SjS-associated) organs, such as salivary glands. Single-cell RNA sequencing identified IL-21+CXCL13+IFN-γ+ICOS+TIGIT+GPR56+ Tph cells in the salivary glands. These findings are consistent with reduced saliva volume and elevated SjS markers, such as anti-SSA antibody, in these mice, which were both ameliorated by immunosuppressants. In vitro, CD8+ T cells from hPBMC mice induced B cell apoptosis and inhibited Tph/Tfh differentiation. This model advances understanding of human Tph/Tfh cell biology and offers a valuable platform for studying SjS and therapeutic targets.
Authors
Mariam Piruzyan, Sota Fujimori, Ryota Sato, Yuki Imura, Sachiko Mochiduki, Kana Takemoto, Akiko Nishidate, Yuzo Koda
Abstract
Processes that promote white adipocyte inflammatory function remain incompletely defined. Here, we demonstrated that type I interferon–dependent (IFN-I–dependent) skewing of adipocyte glycolysis, nicotinamide adenine dinucleotide (NAD+) utilization, and pyruvate kinase isozyme M2 (PKM2) function may contribute to increased systemic and tissue inflammation and disease severity in obesity. Notably, chemical and/or genetic inhibition of glycolysis, the NAD+ salvage pathway, or PKM2 restricted IFN-I–dependent increase in adipocyte inflammatory cytokine production. Further, genetic or small molecule targeting of PKM2 function in vivo was sufficient to reduce systemic and tissue inflammation and metabolic disease severity in obese mice, in an adipocyte PKM2-dependent manner. Further, white adipose tissue of individuals living with obesity and metabolic disease, compared with metabolically healthy individuals with obesity, showed an increase in expression of inflammatory and metabolic genes, while small molecule targeting of PKM2 function contributed to reduced IFN-I–driven inflammatory cytokine production by primary human adipocytes. Together, our findings invoke the IFN-I/PKM2 axis as a potential target for modulating adipocyte dysregulated inflammation.
Authors
Michelle S.M.A. Damen, Pablo C. Alarcon, Calvin C. Chan, Traci E. Stankiewicz, Hak Chung, Keisuke Sawada, Cassidy J. Ulanowicz, John Eom, Jarren R. Oates, Jennifer L. Wayland, Jessica R. Doll, Rajib Mukherjee, Miki Watanabe-Chailland, Lindsey Romick-Rosendale, Sara Szabo, Michael A. Helmrath, Joan Sanchez-Gurmaches, Maria E. Moreno-Fernandez, Senad Divanovic
Abstract
Authors
Zhehao Tan, Gio Wu, Daniela Salgado Figueroa, Paramita Dutta, Zachary Jaeger, Marissa Mazurie, David Schairer, Dawn Eichenfield, Wynnis L. Tom, Lauren Galli, Lawrence Eichenfield, Bob Geng, Brian Hinds, Hal M. Hoffman, Lori Broderick, Ben Croker, Ferhat Ay, Reid Oldenburg
Abstract
Prolonged and dysregulated neutrophilic inflammation causes tissue damage in chronic inflammatory diseases, including antibody-mediated glomerulonephritis (AGN). An increase in glycolysis, supported by enhanced glucose uptake, is a hallmark of hyperneutrophilic inflammation. Neutrophils upregulate glucose transporter 1–mediated (Glut1-mediated) glucose incorporation for renal antimicrobial activities. However, little is known about the role of neutrophil-specific Glut1 function in the pathogenesis of AGN. Using a well-vetted mouse model of AGN, we show that neutrophils upregulate Glut1 expression and function in the nephritic kidney. We demonstrate that Glut1 function in the hematopoietic cells during the early stage of the disease is necessary for kidney pathology. Most importantly, neutrophil-intrinsic Glut1 function is critical for AGN. While neutrophil-specific Glut1 ablation diminished the expression of tissue-damaging effector molecules in both the early and late stages, renal cytokines’ and chemokines’ production were compromised only in the late stage of the disease. Consequently, Glut1 inhibitor treatment ameliorated renal pathology in AGN mice. These data identify a Glut1-driven inflammatory circuit in neutrophils, which is amenable to therapeutic targeting in AGN.
Authors
Hossein Rahimi, Wonseok Choi, Doureradjou Peroumal, Shuxia Wang, Partha S. Biswas
Abstract
Elexacaftor/tezacaftor/ivacaftor (ETI) cystic fibrosis transmembrane conductance regulator (CFTR) modulator therapy has led to rapid and substantial improvements in cystic fibrosis (CF) airway disease. Underlying molecular and cellular mechanisms, long-term efficacy, and ability to reverse airway epithelial remodeling in established disease remain unclear. Longitudinal nasal brushes from an adult CF cohort were used to evaluate gene expression, cellular composition, stem cell function, and microbiome changes at baseline and at 6 months and 2 years after ETI. The baseline to 6 month span showed a massive downregulation of extensive neutrophilic inflammatory gene expression programs that correlated with increased pulmonary function and decreased sinusitis. Primary airway epithelial stem cell cultures from matched donor samples showed partially improved differentiation and barrier capacity at 6 months. Although clinical outcomes remained stable during the 6 month to 2 year span, transcriptional changes revealed a resurgence of baseline inflammatory programs. The time course of gene expression was consistent with ongoing normalization of epithelial remodeling. Relative abundance of Pseudomonas also decreased during the time course. These data suggest that ETI rectifies inflammation, epithelial remodeling, and bacterial infection in the airways, but resurgence of inflammatory gene expression may indicate ongoing inflammation, potentially presaging disease progression with long-term therapy.
Authors
Eszter K. Vladar, Austin E. Gillen, Sangya Yadav, Mikayla R. Murphree, David Baraghoshi, J. Kirk Harris, Elmar Pruesse, Sierra S. Niemiec, Alexandra W.M. Wilson, Katherine B. Hisert, Stephen M. Humphries, Matthew Strand, David A. Lynch, Max A. Seibold, Daniel M. Beswick, Jennifer L. Taylor-Cousar
Abstract
The lung’s mechanosensitive immune response to alveolar overdistension impedes ventilation therapy for hypoxemic respiratory failure. Though mechanistically unclear, the prevailing hypothesis is that the immune response results when alveolar overdistension stretches alveolar macrophages (AMs). Since this hypothesis is untested in live lungs, we optically imaged live mouse alveoli to detect alveolus-adherent, sessile AMs that communicate with the alveolar epithelium through connexin43 (Cx43)-containing gap junctions. Alveolar hyperinflation did not stretch the AMs, but it increased AM Ca2+. AM-specific Cx43 deletion blocked the Ca2+ response, as well lung injury due to mechanical ventilation at high tidal volume (HTV). HTV was also inhibited by AM-targeted delivery of liposomes containing the inhibitor of endosomal Ca2+ release, Xestospongin C. We conclude, Cx43- and Ca2+-dependent AM-epithelial interactions determine the lung’s mechanosensitive immunity, providing a basis for therapy for ventilator-induced lung injury.
Authors
Liberty Mthunzi, Mohammad Islam, Galina A Gusarova, Brian Karolewski, Sunita Bhattacharya, Jahar Bhattacharya
No posts were found with this tag.