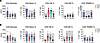Immunology
Abstract
Clonal haematopoiesis of indeterminate potential (CHIP) is the expansion of blood stem cells and progeny after somatic mutation. CHIP associates with increased cardiovascular disease (CVD) with inflammation from macrophages a proposed common effector. However, mouse CHIP studies are discordant for clonal expansion and inflammation. Similarly, directionality of association between CHIP and CVD remains debated. We investigated effects of three CHIP mutations on macrophage cytokines, clonal expansion and atherosclerosis in parallel. We find that Tet2 and Dnmt3a mutations increase cytokines and inflammasome activation in Tet2 but decrease in Dnmt3a. However, Jak2 mutant macrophages produced equivalent cytokine as wild-type. In mice, Tet2 mutants clonally expanded, but Dnmt3a and Jak2 mutants didn’t. Expansion was unaffected by systemic inflammation, while hyperlipidemia expanded Tet2-/- cells, but not mono-allelic mutants. Similarly, human Mendelian randomisation showed no effect of serum cytokines or CVD on CHIP risk. Experimental atherosclerosis was increased in females with Tet2 and males with Jak2, but unchanged with Dnmt3a mutations. Together, common CHIP mutations have disparate effects on macrophage cytokines and clonal expansion, and sex-dependent effects on atherogenesis, suggesting a common mechanism across CHIP is unlikely. Thus, CHIP mutations differ in pathophysiology and clinical sequalae across sexes and should be treated as different entities.
Authors
Paul R. Carter, Lauren Kitt, Amanda Rodgers, Nichola Figg, Ang Zhou, Chengrui Zhu, Ziyang Wang, Peter Libby, Stephen Burgess, George S. Vassiliou, Murray CH. Clarke
Abstract
Hofbauer cells (HBC) are fetal-derived macrophages located in the placenta that contribute to antimicrobial defense, angiogenesis, tissue remodeling, and metabolic processes within the chorionic villi. Although their roles in placental biology are increasingly recognized, the mechanisms that regulate HBC identity and function are not yet fully defined. This study aimed to define the core transcriptomic and epigenomic features of HBCs in term placentas and to examine their capacity for transcriptional responsiveness and phenotypic variation. Using chromatin accessibility profiling and bulk RNA sequencing, we found that HBCs exhibit a unique gene expression and chromatin accessibility profile compared to other fetal and adult macrophages. We identified a coordinated transcriptional network involving nuclear receptors NR4A1–3, the glucocorticoid receptor (GR), and RFX family members (RFX1, RFX2, RFX5) that appears to shape HBC identity, particularly through pathways linked to lipid metabolism and angiogenesis. Although exploratory in nature, in vitro stimulation studies showed that HBCs exhibited increased transcriptional activity in response to combined IL-4 and RSG treatment, including induction of the lipid transporter CD36. Mass cytometry analysis revealed surface markers indicative of both immature and mature macrophage states. Together, these results indicated that HBCs represent a distinct and diverse macrophage population with specialized and adaptable regulatory program in the human placenta.
Authors
Benjámin R. Baráth, Dóra Bojcsuk, Krisztian Bene, Noemí Caballero-Sánchez, Tímea Cseh, João CR. de Freitas, Petros Tzerpos, Marta Toth, Zhonghua Tang, Seth Guller, Zoárd Tibor Krasznai, Patrícia Neuperger, Gabor J. Szebeni, Gergely Nagy, Tamás Deli, Laszlo Nagy
Abstract
Mucosal secretory IgA (sIgA) plays a central role in protecting against the invasion of respiratory pathogen via the upper respiratory tract. To understand how intranasal booster induces mucosal sIgA response in humans, we first used liquid chromatography-tandem mass spectrometry for peptide identification of immunoglobulin (MS Ig-Seq) and single-cell B-cell receptor sequencing (scBCR-seq) to identify mucosal spike-specific sIgA monoclonal antibodies (mAbs) after intranasal booster. These mucosal sIgA mAbs exhibited enhanced neutralization up to 100-fold against SARS-CoV-2 variants compared to their monomeric IgG and IgA isotypes. Deep sequencing and longitudinal analysis of B-cell receptor repertoires revealed that nasal booster re-stimulates memory B cells primed by intramuscularly vaccination to undergo IgA class switching, somatic hypermutation, and clonal expansion. Single-cell sequencing revealed that intranasal booster upregulated the expression of mucosal homing receptors in spike-specific IgA-expressing B cells. This increase coincided with a transient increase of cytokines and chemokines that facilitate B cell recruitment in the nasal mucosa. Our findings demonstrate that intranasal booster can be an effective strategy for inducing upper respiratory mucosal sIgA and establishing mucosal immune protection.
Authors
Si Chen, Zhengyuan Zhang, Zihan Lin, Li Yin, Lishan Ning, Wenming Liu, Qian Wang, Chenchen Yang, Bo Feng, Ying Feng, Yongping Wang, Hengchun Li, Ping He, Huan Liang, Yichu Liu, Zhixia Li, Bo Liu, Yang Li, Diana Boraschi, Linbing Qu, Xuefeng Niu, Nanshan Zhong, Pingchao Li, Ling Chen
Abstract
CD4+ T cells predominate lymphocytic foci found in the salivary glands (SGs) of Sjögren’s disease (SjD) cases. Yet little is known about T cell receptor (TCR) repertoire features that distinguish cases from healthy controls (HCs), the relationship between SG and peripheral blood (PB) repertoires of cases, and antigens recognized by pathogenic T cell clones. We performed deep sequencing of bulk-sorted CD4+CD45RA– PB T cells from SjD cases and matched HCs, and single-cell TCR sequencing of the same T cell population from labial SG biopsies of these cases. We found that clonally expanded SG CD4+ T cells expressed complementarity-determining region 3 (CDR3) sequences that were also detected in multiple copies in the blood of the same individuals with SjD. SjD cases displayed a “private” and restricted PB TCR repertoire with reduced clonotype diversity. We identified SjD-associated TCR motifs with the same putative antigen specificity shared between SGs and PB of cases. Their abundances in PB correlated with reduced salivary flow, linking these T cells with pathogenic disease features. Finally, we discovered 2 Ro60 epitopes eliciting an HLA-restricted immune response from expanded SG T cell clones. The comprehensive characterization of SjD TCR repertoires enables the discovery of target antigens and therapeutic strategies.
Authors
Ananth Aditya Jupudi, Michelle L. Joachims, Christina Lawrence, Charmaine Lopez-Davis, Bhuwan Khatri, Astrid Rasmussen, Kiely Grundahl, R. Hal Scofield, Judith A. James, Joel M. Guthridge, Christopher J. Lessard, Linda F. Thompson, A. Darise Farris
Abstract
Cardiac arrhythmias increase during acute SARS-CoV-2 infection and in long COVID syndrome, by unknown mechanisms. This study explored the acute and long-term effects of COVID-19 on cardiac electrophysiology and the cardiac conduction system (CCS) in a hamster model. Electrocardiograms and subpleural pressures were recorded by telemetry for 4 weeks after SARS-CoV-2 infection, and interferon-stimulated gene expression and macrophage infiltration of the CCS were assessed at 4 days and 4 weeks postinfection. COVID-19 induced pronounced tachypnea and cardiac arrhythmias, including bradycardia and persistent atrioventricular block, though no viral protein expression was detected in the heart. Arrhythmias developed rapidly, partially reversed, and then redeveloped, indicating persistent CCS injury. COVID-19 induced cardiac cytokine expression, connexin mislocalization, and CCS macrophage remodeling. Interestingly, sterile innate immune activation by direct cardiac injection of polyinosinic:polycytidylic acid (PIC) induced arrhythmias similar to those of COVID-19. PIC strongly induced cytokine secretion and interferon signaling in hearts, human induced pluripotent stem cell–derived cardiomyocytes, and engineered heart tissues, accompanied by alterations in excitation-contraction coupling. Importantly, the pulmonary and cardiac effects of COVID-19 were blunted by JAK/STAT inhibition or a mitochondrially targeted antioxidant, indicating that SARS-CoV-2 infection indirectly leads to arrhythmias by innate immune activation and redox stress, which could have implications for long COVID syndrome.
Authors
Deepthi Ashok, Ting Liu, Misato Nakanishi-Koakutsu, Joseph Criscione, Meghana Prakash, Alexis Tensfeldt, Byunggik Kim, Bryan Ho, Julian Chow, Morgan Craney, Mark J. Ranek, Brian L. Lin, Kyriakos Papanicolaou, Agnieszka Sidor, D. Brian Foster, Hee Cheol Cho, Andrew Pekosz, Jason Villano, Deok-Ho Kim, Brian O’Rourke
Abstract
The transcription factor IKAROS, encoded by IKZF1, is crucial for lymphocyte development and differentiation. Germline heterozygous IKZF1 mutations cause B cell immunodeficiency, but also affect T cells. Patients with IKZF1 haploinsufficiency (HI) or dimerization-defective (DD) variants show reduced naive and increased memory T cells, while dominant-negative (DN) mutations result in the opposite phenotype. Gain-of-function patients display variable patterns. To investigate IKAROS’s role in shaping the human naive/memory T cell phenotype, we performed IKAROS immunomodulation and knockdown experiments and analyzed early T cell development in an artificial thymic organoid (ATO) system using CD34+ cells from patients with representative IKZF1 variants. IKAROS inhibition by lenalidomide or silencing by small hairpin RNA directly altered expression of HNRNPLL, the master regulator of CD45 isoform splicing that defines CD45RA+/naive and CD45RO+/memory phenotypes. In the ATO system, IKAROS-DN precursor cells were blocked at the CD4–CD8–/double-negative stage and retained a CD45RA+ phenotype, whereas IKAROS-HI cells inefficiently reached the CD4+CD8+/double-positive stage and partially transitioned from CD45RA to CD45RO. Analysis of public gene expression data showed high HNRNPLL expression in double-positive thymic cells, beyond the stages affected by IKZF1 DN and HI mutations. Collectively, these findings indicate that IKAROS regulates early and late T cell development by mechanisms, including HNRNPLL modulation.
Authors
Jennifer Stoddard, Hye Sun Kuehn, Ravichandra Tagirasa, Marita Bosticardo, Francesca Pala, Julie E. Niemela, Agustin A. Gil Silva, Kayla Amini, Eduardo Anaya, Mario Framil Seoane, Carolina Bouso, Dimana Dimitrova, Jennifer A. Kanakry, Laia Alsina, Matias Oleastro, Steven M. Holland, Thomas A. Fleisher, Richard L. Wasserman, Luigi D. Notarangelo, Sergio D. Rosenzweig
Abstract
Autoimmunity arises when self-reactive B and T cells target the body’s own tissues, with B cells contributing through antigen presentation as well as production of autoantibodies and proinflammatory cytokines. Genome wide association studies (GWAS) and recent identification of loss-of-function gene variants in individuals with young-onset autoimmunity have highlighted a role for protein tyrosine phosphatase nonreceptor type 2 (PTPN2) in development of autoimmunity. While prior studies have focused on the mechanism of Ptpn2 in T cells and other cell types, its function in B cells has not been explored. To test the B cell–intrinsic roles of Ptpn2, we generated a B cell–specific deletion of Ptpn2 in mice (Mb1-Cre;Ptpn2fl/fl). We found that loss of Ptpn2 in B cells promoted organ inflammation, increased the frequency of age/autoimmune-associated B cells (ABCs) and plasmablasts in the periphery, and increased circulating autoantibodies. Moreover, we found that Ptpn2 acted as a negative regulator of the JAK/STAT and TLR7 pathways in B cells. In line with this, treatment of B cells from Mb1-Cre;Ptpn2fl/fl mice with IFN-γ and TLR7 agonist lead to enhanced differentiation into ABCs. These findings highlight the critical roles of Ptpn2 in B cell function and its potential as a key regulator in preventing B cell associated autoimmunity.
Authors
Bridget N. Alexander, Soojin Kim, Kristen L. Wells, Maya J. Hunter, Kevin P. Toole, Scott M. Wemlinger, Daniel P. Regan, Andrew Getahun, Mia J. Smith
Abstract
Developing biomarkers to quantitatively monitor disease-specific T cell activity is crucial for assessing type 1 diabetes (T1D) progression and evaluating immunotherapies. This study presents an approach using V-gene targeted sequencing to quantify T cell receptor (TCR) clonotypes as biomarkers for pathogenic T cells in T1D. We identified "public" TCR clonotypes shared among multiple non-obese diabetic (NOD) mice and human organ donors, with a subset expressed exclusively by islet antigen-reactive T cells in those with T1D. Employing V-gene targeted sequencing of only TCRs containing TRAV16/16D allowed quantitative detection of the public islet antigen-reactive TCR clonotypes in peripheral blood of NOD mice. Frequencies of these public TCR clonotypes distinguished prediabetic NOD mice from those protected from diabetes. In human islets, public TCR clonotypes identical to preproinsulin-specific clones were exclusively found in T1D donors. This quantifiable TCR sequencing approach uncovered public, disease-specific clonotypes in T1D, providing biomarker candidates to monitor pathogenic T cell frequencies in blood for assessing disease activity and therapeutic response.
Authors
Laurie G. Landry, Kristen L. Wells, Amanda M. Anderson, Kristen R. Miller, Kenneth L. Jones, Aaron W. Michels, Maki Nakayama
Abstract
BACKGROUND. Chimeric antigen receptor (CAR) T-cells are a leading immunotherapy for refractory B-cell malignancies; however, their impact is limited by toxicity and incomplete efficacy. Daily (circadian) rhythms in immune function may offer a lever to boost therapeutic success; however, their clinical relevance to CAR T-cell therapy remains unknown. METHODS. We retrospectively analyzed CAR T-cell survival and complications based on infusion time at two geographically distinct hospitals in St. Louis, Missouri (n=384), and Portland, Oregon (n=331) between 1/2018 and 3/2025. The primary outcome was 90-day overall survival (OS). Secondary outcomes included event-free survival (EFS), cytokine release syndrome (CRS), immune cell-associated neurotoxicity syndrome (ICANS), ICU admission, shock, respiratory failure, and infection. We quantified the independent relationship between infusion time and outcomes using multivariable mixed-effects logistic regression and time-to-event models, adjusting for patient, oncologic, and treatment characteristics. RESULTS. The therapeutic index of CAR-T cells inversely correlated with administration time, with later infusions associated with lower effectiveness and more adverse outcomes. For each hour that CAR T-cell treatment was delayed, the adjusted odds of 90-day mortality increased by 24% (aOR 0.64-0.88, p=<0.001), severe neurotoxicity by 17% (p=0.023), and mechanical ventilation by 27% (p=0.026). These temporal patterns were most pronounced in patients receiving CD19-targeting CAR T-cell products. In contrast, we did not find an association between infusion time and severe CRS (aOR 0.99, 95% CI 0.75–1.27, p=0.92). CONCLUSION. Time of day is a potent and easily modifiable factor that could optimize CAR T-cell clinical performance. FUNDING. National Institutes of Health.
Authors
Patrick G. Lyons, Emily Gill, Prisha Kumar, Melissa Beasley, Brenna Park-Egan, Zulfiqar A. Lokhandwala, Katie M. Lebold, Brandon Hayes-Lattin, Catherine L. Hough, Nathan Singh, Guy Hazan, Huram Mok, Janice M. Huss, Colleen A. McEvoy, Jeffrey A. Haspel
Abstract
HDAC8, an evolutionarily distinct, X-linked, zinc-dependent class I histone/protein deacetylase, is implicated in developmental disorders, parasitic infections, myopathy, and cancers. Our study demonstrates the important role of HDAC8 in immune cells by conditional targeting of HDAC8 in murine T cells and application of selective HDAC8 inhibitors. Using flow cytometry, RNA-seq and ChIP-seq analyses, we demonstrate that knocking down or inhibiting HDAC8 impaired murine Treg suppressive function in vitro and in vivo, but promoted conventional host T cell responses, thereby limiting syngeneic tumor growth. Mechanistically, HDAC8 knockout downregulated Foxp3 expression, enhanced H3K27 acetylation levels and promoted IL-2, IL-6, Fas, and FasL expression in both Treg and conventional T-effector cells. Thus, our combined genetic and pharmacologic studies establish the central importance of HDAC8 in T cell responses and suggest that selective HDAC8 inhibitors represent a potential therapeutic approach in immuno-oncology.
Authors
Fanhua Kong, Yan Xiong, Liqing Wang, Rongxiang Han, Hossein Fazelinia, Jennifer Roof, Lynn A. Spruce, Aaron B. Beeler, Wayne W. Hancock
No posts were found with this tag.