Infectious disease
Citation Information: JCI Insight. 2025. https://doi.org/10.1172/jci.insight.199689.
Abstract
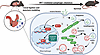
Urinary tract infections (UTIs) are the most common severe bacterial infections in young children, often associated with vesicoureteral reflux (VUR). To explore host genetic-microbiota interactions and their clinical implications, we analyzed the urinary microbiota (urobiota) and conducted genome-wide association studies (GWAS) for bacterial abundance traits in pediatric UTI and VUR patients from the RIVUR and CUTIE cohorts. We identified four urobiota community types based on relative abundance, characterized by the genera Enterococcus, Prevotella, Pseudomonas, and Escherichia/Shigella, and their associations with VUR, age, and toilet training. Children with VUR exhibited decreased microbial diversity and increased abundance of genera that included opportunistic pathogens, suggesting a disrupted urobiota. We detected genome-wide significant genetic associations with urinary bacterial relative abundances, in or near candidate genes including CXCL12, ABCC1, and ROBO1, which are implicated in urinary tract development and response to infection. We showed that Cxcl12 is induced 12 hours after uropathogenic bacterial infection in mouse bladder. The association with CXCL12 suggests a genetic link between UTI, VUR and cardiovascular phenotypes later in life. These findings provide the first characterization of host genetic influences on the pediatric urobiota in UTI and VUR, offering insights into the interplay between disease, host genetics and the urobiota composition.
Authors
Miguel Verbitsky, Pavan Khosla, Daniel Bivona, Atlas Khan, Yask Gupta, Heekuk Park, Tian H. Shen, Aryan Ghotra, Katherine Xu, Iman A. Ghavami, Priya Krithivasan, Jeremiah Martino, Tanya Sezin, Tze Y. Lim, Victoria Kolupaeva, Nita A. Limdi, Yuan Luo, Hakon Hakonarson, Simone Sanna-Cherchi, Krzysztof Kiryluk, Cathy L. Mendelsohn, Anne-Catrin Uhlemann, Jonathan Barasch, Ali G. Gharavi
Citation Information: JCI Insight. 2025. https://doi.org/10.1172/jci.insight.195678.
Abstract
BACKGROUND. Fecal Microbiota Transplantation (FMT) is the most effective therapy for recurrent Clostridioides difficile infection (rCDI), yet its mechanism of action remains poorly understood. METHODS. We report the results of a clinical trial of subjects undergoing FMT therapy for rCDI (n=16), analyzing colon biopsies, plasma, peripheral blood mononuclear cells, and stool at the time of FMT and two-month follow-up. Plasma and colon biopsy samples were also collected from healthy controls for comparison with rCDI patients. Microbiome composition, colonic gene expression, and immune changes were evaluated through high-throughput sequencing and immunoprofiling via flow cytometry. RESULTS. No subjects experienced recurrence at follow-up. FMT significantly altered the intestinal microbiome but had no significant impact on the systemic immune system. In contrast, FMT promoted broad changes in colonic transcriptional profiles compared to both pre-FMT and healthy control biopsies, inhibiting genes associated with pro-inflammatory signaling and upregulating type 2 immunity and proliferative pathways (Myc and mTORC1). FMT increased expression of IL-33 and the type 2 immune EGFR family ligand amphiregulin, potentially explaining upregulation of Myc and mTORC1 pathways. Spatial transcriptomics demonstrated that these changes were localized to the colonic epithelium. Comparison of transcriptional profiles with available single cell gene sets determined that post-FMT biopsies were enriched in signatures associated with proliferative cell types while repressing signatures of differentiated colonocytes. CONCLUSIONS. We conclude that FMT promotes proliferation of the colonic epithelium in rCDI patients, which may drive regeneration and protect against subsequent CDI. REGISTRATION. Clinicaltrials.gov NCT02797288. FUNDING. NIH grants R01 AI152477, R01 AI124214, and K23 AI163368.
Authors
G. Brett Moreau, Jiayi Tian, Nick R. Natale, Farha Naz, Mary K. Young, Uma Nayak, Mehmet Tanyüksel, Isaura Rigo, Gregory R. Madden, Mayuresh M. Abhyankar, Nicholas Hagspiel, Savannah Brovero, Mark Worthington, Brian Behm, Chelsea Marie, William A. Petri Jr., Girija Ramakrishnan
Citation Information: JCI Insight. 2025. https://doi.org/10.1172/jci.insight.197491.
Abstract
Herpes Simplex Virus 2 (HSV-2) infection results in variable rates of local viral shedding in anogenital skin. The impact of episodic viral exposures on immune cells in adjacent mucosal tissues, including the genital tract, is unknown. However, any immune responses at this site could impact protective mucosal immunity, tissue homeostasis, and adverse health outcomes. To investigate the impact of HSV-2 on cervicovaginal tract immunity, we applied flow cytometry, immunofluorescent imaging, analysis of soluble immune factors, and spatial transcriptomics to cervicovaginal tissue and blood samples provided by a total of 232 HSV-2-seropositive and seronegative participants, with genital HSV-2 shedding evaluated at the time of biopsy. This unique dataset was used to define and spatially map immune cell subsets and localized gene expression via spatial transcriptomics. HSV-2-seropositivity alone was associated with minimal differences in cervicovaginal and circulating T cell phenotypes. However, the vaginal mucosa during active HSV-2 shedding was associated with alterations in T cell, macrophage, and dendritic cell localization and gene expression consistent with increased immune surveillance, with immune activating and suppressing signals potentially reinforcing mucosal tissue homeostasis.
Authors
Finn MacLean, Rachael M. Zemek, Adino Tesfahun Tsegaye, Jessica B. Graham, Jessica L. Swarts, Sarah C. Vick, Nicole B. Potchen, Irene Cruz Talavera, Lakshmi Warrier, Julien Dubrulle, Lena K. Schroeder, Anna Elz, David Sowerby, Ayumi Saito, Katherine K. Thomas, Matthias Mack, Joshua T. Schiffer, R. Scott McClelland, Keith R. Jerome, Bhavna H. Chohan, Kenneth Ngure, Nelly Rwamba Mugo, Evan W. Newell, Jairam R. Lingappa, Jennifer M. Lund
Citation Information: JCI Insight. 2025. https://doi.org/10.1172/jci.insight.196809.
Abstract
Toll-like receptor 7 (TLR7) agonists are promising immunostimulatory agents for the treatment of chronic infections and cancer. However, their systemic toxicity remains a challenge. In this study, SA-5, a novel liver-targeted, orally available TLR7 agonist, was evaluated for pharmacokinetics, safety, and efficacy in young and aged macaques across 1–10 mg/kg repeated doses. Safety was evaluated through hematologic, biochemical, and flow cytometric profiling, while efficacy was assessed via IFN-α production, gene expression of interferon-stimulated genes, and plasmacytoid dendritic cell activation. A principal component analysis (PCA)-based composite scoring system was used to integrate multimodal parameters. SA-5 induced dose-dependent type I IFN with limited systemic inflammation, with 3 mg/kg showing optimal balance. SA-5 had comparable immunostimulatory activity to GS-9620 but with reduced adverse biomarker shifts. In aged macaques, efficacy was maintained with modestly increased safety responses. These findings support SA-5 as a safer next-generation TLR7 agonist effective across age groups, highlighting integrated biomarker profiling in preclinical immunomodulatory drug development.
Authors
Shokichi Takahama, Takahiro Tomiyama, Sachiyo Yoshio, Yuta Nagatsuka, Hirotomo Murakami, Takuto Nogimori, Mami Kochi, Shoko Ochiai, Hidenori Kimura, Akihisa Fukushima, Tatsuya Kanto, Takuya Yamamoto
Citation Information: JCI Insight. 2025. https://doi.org/10.1172/jci.insight.194450.
Abstract
The immune mechanisms induced by the Bacillus Calmette-Guérin (BCG) vaccine, and the subset of which mediate protection against tuberculosis (TB), remain poorly understood. This is further complicated by difficulties to verify vaccine-induced protection in humans. Although research in animal models, namely mice and non-human primates (NHPs), has begun to close this knowledge gap, discrepancies in the relative importance of biological pathways across species limit the utility of animal model-derived biological insights in humans. To address these challenges, we applied a systems modeling framework, Translatable Components Regression (TransCompR), to identify human blood transcriptional variability which could predict Mtb challenge outcomes in BCG-vaccinated NHPs. These protection-associated pathways included both innate and adaptive immune activation mechanisms, along with signaling via type I interferons and anti-mycobacterial T helper cytokines. We further partially validated the associations between these mechanisms and protection in humans using publicly available microarray data collected from BCG-vaccinated infants who either developed TB or remained healthy during two years of follow-up. Overall, our work demonstrates how species translation modeling can leverage animal studies to generate hypotheses about the mechanisms that underlie human infectious disease and vaccination outcomes, which may be difficult or impossible to ascertain using human data alone.
Authors
Kate Bridges, Denis Awany, Anele Gela, Temwa-Dango Mwambene, Sherry L. Kurtz, Richard E. Baker, Karen L. Elkins, Christopher M. Sassetti, Thomas J. Scriba, Douglas A. Lauffenburger
Citation Information: JCI Insight. 2025;10(21):e189420. https://doi.org/10.1172/jci.insight.189420.
Abstract
Sepsis contributes substantially to mortality rates worldwide, yet clinical trials that have focused on its underlying pathogenesis have failed to demonstrate benefits. Recently, enhancing self-defense has been regarded as an emerging therapeutic approach. Autophagy is a self-defense mechanism that protects septic mice, but its regulatory factor is still unknown. Moreover, the role of interferon regulatory factor 7 (IRF7) in sepsis has been debated. Here, we showed that Irf7 deficiency increased mortality during polymicrobial sepsis. Furthermore, IRF7 drove macrophages to protect against sepsis. Mechanistically, IRF7 is a transcription factor that upregulates the expression of autophagy-related genes responsible for autophagosome formation and autolysosome maturation, induces autophagic killing of bacteria, and ultimately reduces septic organ injury. Recombinant adeno-associated virus 9–Irf7–mediated IRF7 overexpression promoted the autophagic clearance of pathogens and improved sepsis outcomes, which may be the mechanism underlying the observed improvement in bacterial clearance. These findings provide evidence that IRF7 is the underlying regulatory factor that drives autophagy to eliminate pathogens in macrophages during sepsis. Collectively, IRF7 overexpression represents a potential host-directed therapeutic strategy for preclinical sepsis models, operating independently of antibiotic mechanisms.
Authors
Guiming Chen, Kangxin Li, Haihua Luo, Lianxu Zhao, Yong Jiang
Citation Information: JCI Insight. 2025;10(21):e194932. https://doi.org/10.1172/jci.insight.194932.
Abstract
Primary exposure to influenza antigens during infancy shapes the humoral response to subsequent exposures. Development of a universal vaccine approach to protect newborns against influenza would represent a major step forward. In our previous study, we showed vaccination of newborn African green monkeys (AGMs) with an adjuvanted hemagglutinin (HA) stem nanoparticle induced robust IgG responses with broad recognition across HAs. Here, we examined the cellular responses in the lung-draining lymph node of these vaccinated newborn AGMs following challenge with a heterologous H1N1 virus. Our results show that vaccination is associated with early HA stem IgG+ B cell and antibody-secreting cell responses following infection, consistent with a rapidly recalled memory response. In addition, there was evidence of an increase in both HA stem– and head–specific plasma cells in vaccinated animals, suggesting a vaccine-engendered benefit for novel antibodies targeting HA epitopes. Finally, challenge was associated with preferential increases in antibodies that cross-react with H5 HA, suggesting improved protection against this divergent strain. Overall, these findings indicate that HA stem with AddaVax as adjuvant generates a stem-specific cross-reactive memory pool in newborn AGMs with the potential to be rapidly recalled upon infection.
Authors
Kali F. Crofts, Beth C. Holbrook, Courtney L. Page, Maya Sangesland, Masaru Kanekiyo, Martha Alexander-Miller
Citation Information: JCI Insight. 2025;10(21):e195436. https://doi.org/10.1172/jci.insight.195436.
Abstract
BACKGROUND Accurate prognostic assays for COVID-19 represent an unmet clinical need. We sought to identify and validate early parsimonious transcriptomic signatures that accurately predict fatal outcomes.METHODS We studied 894 patients enrolled in the prospective, multicenter Immunophenotyping Assessment in a COVID-19 Cohort (IMPACC) with peripheral blood mononuclear cells (PBMC) and nasal swabs collected within 48 hours of admission. Host gene expression was measured with RNA-Seq. We trained parsimonious prognostic classifiers incorporating host gene expression, age, and SARS-CoV-2 viral load to predict 28-day mortality in 70% of the cohort. Classifier performance was determined in the remaining 30% and externally validated in a contemporary COVID-19 cohort (n = 137) with vaccinated patients.RESULTS Fatal COVID-19 was characterized by 4,189 differentially expressed genes in the peripheral blood. A COVID-specific 3-gene peripheral blood classifier (CD83, ATP1B2, DAAM2) combined with age and SARS-CoV-2 viral load achieved an area under the receiver operating characteristic curve (AUC) of 0.88 (95% CI, 0.82–0.94). A 3-gene nasal classifier (SLC5A5, CD200R1, FCER1A), in comparison, yielded an AUC of 0.74 (95% CI, 0.64–0.83). Notably, OLAH, the most strongly upregulated gene in both PBMC and nasal swab and recently implicated in severe viral infection pathogenesis, yielded AUCs of 0.86 (0.79–0.93) and 0.78 (95% CI, 0.69–0.86), respectively. Both peripheral blood classifiers demonstrated comparable performance in an independent contemporary cohort of vaccinated patients (AUCs 0.74–0.80).CONCLUSION Our parsimonious blood- and nasal-based classifiers accurately predicted COVID-19 mortality and merit further study as accessible prognostic tools to guide triage, resource allocation, and early therapeutic interventions.FUNDING NIH: 5R01AI135803-03, R35HL140026, 5U19AI118608-04, 5U19AI128910-04, 4U19AI090023-11, 4U19AI118610-06, R01AI145835-01A1S1, 5U19AI062629-17, 5U19AI057229-17, 5U19AI125357-05, 5U19AI128913-03, 3U19AI077439-13, 5U54AI142766-03, 5R01AI104870-07, 3U19AI089992-09, 3U19AI128913-03, 5T32DA018926-18, and K0826161611. National Institute of Allergy and Infectious Diseases, NIH: 3U19AI1289130, U19AI128913-04S1, and R01AI122220. National Center for Advancing Translational Sciences, NIH: UM1TR004528. The National Science Foundation: DMS2310836. The Chan Zuckerberg Biohub San Francisco.
Authors
Rithwik Narendra, Emily C. Lydon, Hoang Van Phan, Natasha Spottiswoode, Lucile P. Neyton, Joann Diray-Arce, IMPACC Network, COMET Consortium, EARLI Consortium, Patrice M. Becker, Seunghee Kim-Schulze, Annmarie Hoch, Harry Pickering, Patrick van Zalm, Charles B. Cairns, Matthew C. Altman, Alison D. Augustine, Steve Bosinger, Walter Eckalbar, Leying Guan, Naresh Doni Jayavelu, Steven H. Kleinstein, Florian Krammer, Holden T. Maecker, Al Ozonoff, Bjoern Peters, Nadine Rouphael, Ruth R. Montgomery, Elaine Reed, Joanna Schaenman, Hanno Steen, Ofer Levy, Sidney C. Haller, David Erle, Carolyn M. Hendrickson, Matthew F. Krummel, Michael A. Matthay, Prescott Woodruff, Elias K. Haddad, Carolyn S. Calfee, Charles R. Langelier
Citation Information: JCI Insight. 2025;10(21):e198069. https://doi.org/10.1172/jci.insight.198069.
Abstract
Despite the widespread use of adenovirus, mRNA, and protein-based vaccines during the COVID-19 pandemic, their relative immunological profiles and protective efficacies remain incompletely defined. Here, we compared antigen kinetics, innate and adaptive immune responses, and protective efficacy following Ad5, mRNA, and protein vaccination in mice. Ad5 induced the most sustained antigen expression, but mRNA induced the most potent IFN responses, associated with robust antigen presentation and costimulation. Unlike Ad5 vaccines, which were hindered by preexisting vector immunity, mRNA vaccines retained efficacy after repeated use. As a single-dose regimen, Ad5 vaccines elicited higher immune responses. However, as a prime-boost regimen, and particularly in Ad5 seropositive mice, mRNA vaccines were more immunogenic than the other vaccine platforms. These findings highlight strengths of each vaccine platform and underscore the importance of host serostatus in determining optimal vaccine performance.
Authors
Bakare Awakoaiye, Shiyi Li, Sarah Sanchez, Tanushree Dangi, Nahid Irani, Laura Arroyo, Gabriel Arellano, Shadi Mohammadabadi, Malika Aid, Pablo Penaloza-MacMaster
Citation Information: JCI Insight. 2025. https://doi.org/10.1172/jci.insight.197308.
Abstract
Elite controllers (ECs) maintain undetectable levels of plasma viremia in the absence of treatment, but small reservoirs of replication-competent proviruses persist in the vast majority of these persons. We longitudinally studied paired blood and inguinal lymph node samples (LNMC) from two ECs to better characterize distinguishing features of viral reservoir cell dynamics in ECs. In both participants, we observed a 7- to 10-fold lower frequency of intact proviruses in LNMC samples relative to reservoir cells circulating in blood. The landscape of intact proviruses in both tissue compartments was dominated by shared large clones that were frequently integrated in non-coding DNA regions, but the frequency and diversity of intact proviruses was more limited in LNMCs. Of note, over 9-10 years of longitudinal follow-up, a 3- to 18-fold reduction of intact proviruses was observed. Together, these data support the hypothesis that viral reservoirs in ECs’ blood and lymphoid tissues are under strong, likely immune-mediated selection pressure.
Authors
Samantha K. Marzi, Chloé M. Naasz, Leah Carrere, Carmen Gasca-Capote, Isabelle C. Roseto, Ce Gao, Matthias Cavassini, Andrea Mastrangelo, Mathias Lichterfeld, Matthieu Perreau, Xu G. Yu
No posts were found with this tag.