Cell biology
Abstract
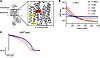
Abdominal aortic aneurysm (AAA) lacks effective pharmacological therapies. Here, we investigate transcription factor 7-like 2 (TCF7L2), a genetic locus associated with both thoracic and abdominal aortic aneurysms, to elucidate its role in AAA pathogenesis. Integrating summary-data-based Mendelian randomization (SMR) with single-cell RNA sequencing (scRNA-seq) of human and mouse aortas, we identify TCF7L2 as a gene enriched in vascular smooth muscle cells (VSMCs) and causally linked to AAA development. Smooth muscle cell-specific TCF7L2 knockout significantly attenuates AAA formation across three distinct murine models (Ang II infusion-, BAPN/Ang II co-administration-, and elastase-induced AAA), independent of systemic blood pressure or lipid levels. Mechanistic studies reveal that TCF7L2 directly upregulates MMP14 and downregulates TIMP3 expression in vitro and in vivo, driving MMP2-mediated extracellular matrix (ECM) degradation. Concurrently, TCF7L2 represses integrin β1 (ITGB1) expression, reducing VSMC adhesion to the ECM. Collectively, these findings identify TCF7L2 as a key driver of pathological vascular remodeling in AAA, suggesting that targeting TCF7L2 may offer a novel therapeutic strategy for limiting AAA progression.
Authors
Yongjie Deng, Yaozhong Liu, Yang Zhao, Hongyu Liu, Guizhen Zhao, Zhenguo Wang, Xu Zhang, Chao Xue, Wei Huang, Tianqing Zhu, Haocheng Lu, Yanhong Guo, Lin Chang, Ida Surakka, Y. Eugene Chen, Jifeng Zhang
Abstract
Aortic dissection or rupture is a leading cause of mortality in vascular Ehlers-Danlos syndrome (VEDS), a disorder caused by mutations in the COL3A1 gene. Col3a1G938D/+ mice recapitulate features of VEDS, including high risk of aortic rupture. As in people with VEDS, aortic risk in this model accelerates at the onset of puberty, especially in males. We identify developmentally regulated gene programs associated with this vulnerability and that are targeted by treatments that mitigate aortic risk. Both genetic and pharmacological inhibition of the androgen receptor (AR) eliminated survival differences between sexes, while treatment with a dual AR and mineralocorticoid receptor (MR) antagonist provided near-complete and durable protection in both sexes. Pathways targeted by dual AR/MR inhibition, including those related to extracellular matrix (ECM) organization and cell-ECM interactions, largely overlapped with those also modulated by isolated MR antagonism. Selective targeting of MR signaling emerged as an effective therapeutic strategy in both sexes that avoids sexual side effects in males.
Authors
Emily E. Juzwiak, Caitlin J. Bowen, Rhiannon Edwards, Leda Restrepo, Serena Lee, Cassie A. Parks, Anthony Zeng, Maya M. Black, Oscar E. Reyes Gaido, Emily E. Bramel, Dustin T. Shigaki, Michael A. Beer, Chiara Bellini, Harry C. Dietz, Elena Gallo MacFarlane
Abstract
Pulmonary fibrosis is frequently accompanied by pulmonary hypertension, which can occur disproportionate to the extent of fibrosis, suggesting a fibrosis-independent vascular remodeling process. Here, we demonstrated that plasma growth differentiation factor 15 (GDF15) is elevated across diverse fibrotic lung disease subtypes and correlates with markers of elevated right heart pressures, but not pulmonary function indices, indicating a possible link to endothelial cell dysfunction. To investigate the import of endothelial GDF15 as a modifier of lung fibrosis pathogenesis, we generated endothelial cell-specific Gdf15 knockout mice, which showed protection from bleomycin-induced lung injury and fibrosis, with preserved lung function. RNA sequencing of human pulmonary microvascular endothelial cells revealed altered expression of barrier-regulatory genes in GDF15-deficient endothelial cells compared to controls. Functional studies confirmed that GDF15 knockdown attenuates thrombin-induced barrier disruption by reducing cytosolic Ca2+ responses. Together, these findings implicate endothelial GDF15 as a modifier of vascular permeability and Ca2+ signaling, and a contributor to lung injury and fibrosis.
Authors
Kristen Raffensperger, Marta Bueno, Brian J. Philips, Megan Miller, Máté Katona, Shuai Yuan, Adriana Estrada-Bernal, Byron Chuan, Pavan Suresh, Stephanie Taiclet, Scott Hahn, Yingze Zhang, Jonathan K. Alder, Seyed Mehdi Nouraie, Daniel J. Kass, Oliver Eickelberg, Adam C. Straub
Abstract
Idiopathic pulmonary fibrosis (IPF) is a progressive interstitial lung disease driven by aberrant fibroblast-to-myofibroblast differentiation, which requires metabolic reprogramming. Here, we identify alanine as an essential metabolite for myofibroblast differentiation. Transforming growth factor–β1 (TGF-β) increases intracellular alanine levels through enhanced synthesis and import in both normal and IPF lung fibroblasts. Alanine synthesis is primarily mediated by glutamate-pyruvate transaminase 2 (GPT2), whose expression is regulated by the glutamine–glutamate–α-ketoglutarate axis. Inhibition of GPT2 depletes alanine and suppresses TGF-β-induced α-SMA and COL1A1 expression, which are rescued by exogenous alanine. We also identify solute carrier family 38 member 2 (SLC38A2) as a transporter for both alanine and glutamine, upregulated by TGF-β or alanine deprivation. SLC38A2 and GPT2 form a coordinated regulatory axis sustaining intracellular alanine levels to support myofibroblast differentiation. Mechanistically, alanine deficiency impairs glycolytic flux and depletes tricarboxylic acid cycle intermediates, while alanine supplementation provides carbon and nitrogen for intracellular glutamate and proline biosynthesis, particularly under glutamine deprivation. Combined inhibition of alanine synthesis and uptake suppresses fibrogenic responses in fibroblasts and human precision-cut lung slices, highlighting dual metabolic targeting as a potential therapeutic strategy for fibrotic lung disease.
Authors
Fei Li, Niv Vigder, David R. Ziehr, Mari Kamiya, Hung N. Nguyen, Diana E. Ferreyra Faustino, Aseel H. Khalil, Hilaire C. Lam, Matthew L. Steinhauser, Edy Y. Kim, William M. Oldham
Abstract
Donnai-Barrow Syndrome (DBS) arises from loss-of-function (LoF) variants in the endocytic receptor LRP2/megalin and is characterized by low molecular weight (LMW) proteinuria and developmental abnormalities. Urinary proteomics of nine DBS patients revealed that the urinary proteome of a DBS patient with the missense variant LRP2 p.C1400R was indistinguishable from that of patients with splice site, nonsense, or frameshift mutations. A CRISPR mouse model of the variant was generated to determine the mechanism of LoF and proteinuria. The mutant LRP2 was expressed and observed to dimerize and localize to the proximal tubule apical membrane. However, both fluid-phase and receptor-mediated endocytosis were impaired in the context of a general perturbation of endocytic flux. Immunofluorescence revealed aberrant endocytic recycling with mislocalized RAB11+ and TFR1+ compartments and enlarged lysosomes. Structural modeling showed the LRP2 assembly likely tolerates the cysteine to arginine substitution at the cell surface, but at endosomal pH the variant introduced steric clashes that may disrupt intramolecular interfaces and disturb receptor recycling. These findings point to the importance of LRP2 recycling for global endocytic flux and offer a blueprint for leveraging patient-specific alleles to dissect proximal tubule function.
Authors
Andrew Beenken, Tian H. Shen, Aryan Ghotra, Hediye Erdjument-Bromage, Jeong Lee, Jared S. Kushner, Rachel E. Sturley, Atlas Khan, Jeffrey R. Arace, Leora Kronenberg, Lucy D. Shen, Gabriel H. Rahmani, Patricia K. Donahoe, Thomas A. Neubert, Frances A. High, Ora A. Weisz, Jonathan Barasch
Abstract
Extracellular matrix (ECM) disorder was considered as the result of fibrosis, but it is recently recognized that fibrotic ECM initiates a self-reinforcing circuit and contributes to development of fibrosis. Versican, an ECM component, participates in cell-ECM interaction and ECM regeneration. In pleura, versican is primarily derived from pleural mesothelial cells (PMCs). However, the role and mechanism of versican in pleural fibrosis remained unknown. In this study, versican and versican-mediated pleural viscoelasticity was found elevated in both human and murine pleural fibrotic tissues. Versican knockdown by shRNA prevented increases of viscoelasticity as well as pleural fibrosis. High level of versican and viscoelasticity promoted mesothelial to mesenchymal transition (MesoMT) in PMCs. Mechanistically, increased viscoelasticity induced pleural fibrosis through CD44/USP10/Smad4 mechanotransduction pathway. In conclusion, these results revealed that excessive versican in fibrotic pleural ECM enhanced ECM viscoelasticity, and consequently promoted progression of pleural fibrosis.
Authors
Zi-Heng Jia, Xin-Liang He, Xiao-Lin Cui, Qian Li, Pei-Pei Cheng, Li-Qin Zhao, Shu-Yi Ye, Shi-He Hu, Chen-Yue Lian, He-De Zhang, Li-Mei Liang, Lin-Jie Song, Fan Yu, Liang Xiong, Fei Xiang, Xiaorong Wang, Meng Wang, Xiyong Dai, Hong Ye, Wan-Li Ma
Abstract
Impaired adhesion and differentiation of keratinocytes is a hallmark of several skin diseases, but only some of the factors that regulate these processes have been identified. Here, we studied the role of isoform-rich dermokine – a wound- and tumor-regulated protein – in keratinocytes using a combination of multi-omics and functional approaches. CRISPR/Cas9-induced knockout of dermokine isoforms in human keratinocytes inhibited differentiation of these cells in three-dimensional organotypic skin cultures, which was confirmed by quantitative proteomics. In two-dimensional monocultures, dermokine deficiency affected the proteome and phosphoproteome as revealed by mass spectrometry. We found reduced abundance of differentiation-specific proteins and increased phosphorylation of cell adhesion protein p120 (catenin-δ1). The adhesive strength of dermokine knockout keratinocytes was impaired, which was rescued by p120 knock-down or ROCK inhibition. Finally, we verified the correlation between decreased dermokine expression and increased p120 phosphorylation in human non-healing wounds. These results identify dermokine as regulator of keratinocyte adhesion and differentiation, involving at least in part its effect on p120 phosphorylation and ROCK. Our data point to a function of dermokine in the pathogenesis of chronic wounds.
Authors
Vahap Canbay, Till Wüstemann, Weihua Tian, Tobias A. Beyer, Camilla Reiter Elbæk, Michael Stumpe, Gaetana Restivo, Chatpakorn Christiansen, Anabel Migenda Herranz, Susanne Mailand, Jürg Hafner, Rune Busk Damgaard, Steffen Goletz, Jörn Dengjel, Ulrich auf dem Keller, Chiara Francavilla
Abstract
Lysophosphatidic acid (LPA) is a bioactive lipid that signals through G protein–coupled receptors (LPA1–6) and regulates multiple cellular processes, including fibrosis. Although LPA signaling has been implicated in fibrotic diseases in several organs, its role in skeletal muscle remains unclear. Here, we show that LPA/LPA1 signaling promotes fibrogenesis after sciatic nerve transection. Denervation induces differential expression of LPA signaling axis components and a transient early increase in intramuscular LPA levels. Pharmacological inhibition of LPA1/3 with Ki16425, or genetic deletion of LPA1, reduces extracellular matrix accumulation and expansion of fibro/adipogenic progenitors (FAPs) in denervated muscle. Although LPA blockade suppresses atrophy-related gene expression, it does not fully preserve myofiber size. Mechanistically, denervation increases YAP/TAZ expression, nuclear localization in FAPs, and transcriptional activity, effects that are attenuated by LPA axis inhibition. Furthermore, pharmacological inhibition of YAP/TAZ with verteporfin reduces fibrosis after denervation, supporting their role as critical downstream mediators. Finally, transient denervation activates the LPA axis, promotes muscle fibrosis, reduces axonal density in the sciatic nerve, and increases neuromuscular junction instability, effects reversed by Ki16425. Together, these findings identify the LPA/LPA1/YAP/TAZ pathway as a key driver of denervation-induced muscle fibrosis and a potential therapeutic target in neuromuscular disorders.
Authors
Meilyn Cruz-Soca, Adriana Córdova-Casanova, Jennifer Faundez-Contreras, Nicolás W. Martínez, Francesca Vaccaro-Rivera, Sebastián Bazaes-Astorga, Cristian Gutiérrez-Rojas, Felipe S. Gallardo, Daniela L. Rebolledo, Felipe A. Court, Jerold Chun, Carlos P. Vio, Soledad Matus, Juan Carlos Casar, Enrique Brandan
Abstract
Inactivating NOTCH1 mutations in head and neck squamous cell carcinoma (HNSCC) were described over a decade ago, suggesting a tumorsuppressor function—unlike its oncogenic role in other tumors. Today, much debate persists regarding a putative oncogenic role in HNSCC as well, with reports that NOTCH1 signaling drives tumor growth and a cancerstemcell (CSC) phenotype. In this work, comprehensive experiments unequivocally demonstrate that NOTCH1 is a tumor suppressor in HNSCC regardless of mutation or activation status and that it reduces CSC frequency. We developed a signature of NOTCH1 activation showing the pathway is associated with very early differentiation, an altered tumor microenvironment, and better prognosis. Clarifying whether NOTCH1 occasionally functions as an oncogenic driver in HNSCC is crucial to prognosis and personalized therapy. The results presented unify the field, reconcile conflicting data, and provide critical insights into the biological and clinical significance of NOTCH1, with broader implications in other squamous carcinomas with NOTCH1 mutations.
Authors
Chenfei Huang, Shhyam Moorthy, Qiuli Li, Kazi M. Ahmed, Kalil Saab, Defeng Deng, Jiping Wang, Xiayu Rao, Jiexin Zhang, Yuanxin Xi, Jing Wang, Zhiyi Liu, Noriaki Tanaka, David A. Wheeler, Eve Shinbrot, Rami Saade, Curtis R. Pickering, Tong-Xin Xie, Adel K. El-Naggar, Abdullah A. Osman, Kunal Rai, Patrick A. Zweidler-McKay, John V. Heymach, Lauren A. Byers, Faye M. Johnson, Vlad C. Sandulache, Jeffrey N. Myers, Pedram Yadollahi, Mitchell J. Frederick
Abstract
Short QT syndrome is a heritable arrhythmia disorder linked to sudden cardiac death. We recently identified that individuals with alternating hemiplegia of childhood (AHC), a rare neurodevelopmental disorder, can exhibit shortened corrected QT intervals and elevated risk for ventricular fibrillation. This is especially true for patients with AHC heterozygous for the recurrent ATP1A3-D801N variant, though the underlying cardiac mechanism remains unclear. We hypothesized that the D801N missense impairs Na+/K+-ATPase function, causing Ca2+ overload, shortened action potential duration (APD), and arrhythmias. Using in silico modeling and patient-derived induced pluripotent stem cell cardiomyocytes (iPSC-CMsD801N), we observed shorter APD, elevated intracellular and sarcoplasmic reticulum Ca2+ levels, and delayed afterdepolarizations (DADs) compared with WT. Additionally, increased Ca²+ influx via the Na+/Ca2+ exchanger (NCX1) during depolarization was observed in iPSC-CMsD801N. Simulations and in vitro experiments suggest that reduced ATPase function accelerated inactivation of L-type Ca2+ channels. Pharmacologic inhibition of NCX1 with ORM-10103 normalized APD and reduced DADs. These findings support a Ca2+-mediated mechanism for arrhythmogenesis in ATP1A3-D801N carriers and identify NCX1 as a potential therapeutic target.
Authors
Minu-Tshyeto K. Bidzimou, Padmapriya Muralidharan, Zhushan Zhang, Danyal Raza, Daniel Needs, Bo Sun, Robin M. Perelli, Mary E. Moya-Mendez, P.K. Rakesh Manivannan, Arsen S. Hunanyan, Abbigail Helfer, Christine Q. Simmons, Alfred L. George Jr., Donald M. Bers, Nenad Bursac, Mohamad A. Mikati, Andrew P. Landstrom
No posts were found with this tag.