Immunology
Abstract
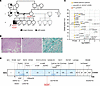
Tumor-infiltrating CD8 cells recognize neoantigens created by tumor-specific mutations. Nonetheless, even after checkpoint inhibitor therapy, most patients progress. A deeper understanding of anti-tumor responses could facilitate development of better therapies. To enable such studies, we applied TCXpress, a high throughput platform that clones fully expressible TCRs from single cells into retro- or lenti- viral vectors without sequencing or gene synthesis, to study TCRs from CD8 cells infiltrating mouse MC38 tumors. We expressed cloned TCRs in reporter cells and interrogated TCR specificity by coculturing them with B6WT3 cells transduced with tandem minigenes encoding predicted neoantigens. We isolated TCRs reactive against epitopes from mutant Rpl18, Adpgk, Psmd2, and Zc3h7b along with self-reactive TCRs that recognized normal B6 and MC38 cells. Importantly, we successfully treated MC38-bearing mice with T cells transduced with anti-Rpl18 TCRs. These results establish a system that could be used to study many types of T cell responses and validates a therapeutic approach that could be tested in the clinic.
Authors
Alexander M. Rowe, Smriti Chaurasia, Wenzhong Wei, Laura García-Diéguez, Katherine Querry, Johnathon G. Schiebel, Christy Smolak, Alexander G. Muralles, Daniel Wikenheiser, Kevin Quann, Collin Pirner, Kentin Codispot, Mark J. Shlomchik, Warren D. Shlomchik
Abstract
Enhancing NAD+ levels with nicotinamide riboside (NR) confers anti-inflammatory effects in human disease, although immunoregulatory mechanisms remain poorly characterized. We previously showed that ex vivo NR supplementation of primary CD4+ T cells from psoriatic individuals dampened immune responsiveness. To validate this in vivo, we performed a randomized, placebo-controlled NR supplementation study in individuals with mild-to-moderate psoriasis. Participants received oral NR (500 mg twice daily) or matching placebo for 4 weeks, with blood samples collected at baseline and after supplementation. NR reduced Th17 immune responsiveness. Bulk CD4+ T cell RNA-seq identified induction of the SLIT-ROBO signaling pathway. NR supplementation increased circulating SLIT2 levels and enhanced SLIT2 production in dermal fibroblasts. Pharmacologic and genetic interrogation in CD4+ T cells and fibroblasts demonstrated that SLIT2, acting through the ROBO1 receptor, inhibited Rho GTPase signaling, thereby attenuating canonical Th17 polarization and fibroblast inflammatory activation. These findings indicate that NAD+ augmentation exerts anti-inflammatory effects in psoriasis through SLIT2-ROBO1-mediated crosstalk between dermal fibroblasts and circulating CD4+ T cells, leading to suppression of Th17-driven inflammation.
Authors
Kim Han, Rachael J. Klein, Thomas C. Recupero, Anna Chiara Russo, Rahul Sharma, Anand K. Gupta, Shahin Hassanzadeh, Rebecca D. Huffstutler, Pradeep K. Dagur, Bryan Fisk, Neelam R. Redekar, Michael N. Sack
Abstract
CHI3L1, a chitinase-like protein, is implicated in pulmonary fibrosis, yet its mechanisms incompletely understood. In this study, we demonstrated that CHI3L1 coordinates profibrotic macrophage activation and invasive myofibroblast differentiation, and their crosstalk. In vitro, CHI3L1 drove M2-like macrophage polarization as evidenced by increased CD163, CD206, and PD-L1, and amplified TGF-β1-induced fibroblast responses, including myofibroblast transformation, migration, and invasion. Mechanistically, CHI3L1 enhanced TGF-β1 signaling through SMAD, AKT, and ERK pathways, and PD-L1 was required for CHI3L1/TGF-β1-driven myofibroblast transformation. Co-culture studies further demonstrated the ability of CHI3L1 to induce profibrotic macrophage activation that enhanced myofibroblast transformation mediated via a CD44–PD-L1 axis. In vivo, following bleomycin challenge, CHI3L1 transgenic mice exhibited increased PD-L1+ M2 macrophages, PD-L1+/PDGFRα+ fibroblasts, and PD-1+ immune cells compared with wild-type controls. Therapeutically, combined anti-CHI3L1 and anti-PD-1 antibodies, as well as a bispecific anti-CHI3L1-anti-PD-1 antibody, produced greater anti-fibrotic efficacy than monotherapy. These findings demonstrate crosstalk between CHI3L1 and the PD-1/PD-L1 pathway that promotes profibrotic macrophage activation and invasive fibroblast differentiation and support dual targeting of CHI3L1 and PD-1/PD-L1 as a promising therapeutic strategy for pulmonary fibrosis.
Authors
Han-Seok Jeong, Takayuki Sadanaga, Joyce H. Lee, Suchitra Kamle, Bing Ma, Yang Zhou, Sung Jae Shin, Jack A. Elias, Chun Geun Lee
Abstract
Eosinophilic esophagitis (EoE) is a type 2 allergic disease characterized by esophageal inflammation and epithelial cell dysfunction. The acquired loss of the anti-serine protease of kazal type 7 (SPINK7) in the squamous epithelium of the esophagus has a causal role in EoE pathogenesis. Yet there is a limited understanding of the factors that regulate its expression and responsiveness to inflammatory stimuli. Herein, we have identified the transcription factor, ovo like transcriptional repressor 1 (OVOL1) as an esophageal selective gene product that regulates SPINK7 promoter activity. Overexpression of OVOL1 increased SPINK7 expression, whereas its depletion decreased SPINK7 expression, impaired epithelial barrier and increased production of the pro-atopy cytokine thymic stromal lymphopoietin (TSLP). Stimulation with IL-13 abrogated the nuclear translocation of OVOL1 and promoted enhanced degradation of OVOL1 protein. This effect of IL-13 was dependent on the esophageal specific cysteine protease calpain-14 at least in part. Analysis of human esophageal biopsies demonstrated that the expression of esophageal OVOL1 correlated with SPINK7 transcript expression and was lost as a function of EoE disease activity. In summary, our study identifies key regulatory mechanisms in EoE pathogenesis, demonstrating that OVOL1 promotes SPINK7 transcription, whereas IL-13 suppresses this pathway in EoE.
Authors
Nurit P. Azouz, Andrea M. Klingler, Sierra S. Beach, Kalen A. Rossey, Mark Rochman, Misu Paul, Julie M. Caldwell, Michael Brusilovsky, Alexander T. Dwyer, Xiaoting Chen, Daniel Miller, Carmy Forney, Leah C. Kottyan, Matthew T. Weirauch, Marc E. Rothenberg
Abstract
Human γδ T cells are a rare but functionally diverse lymphocyte subset critical for tumor surveillance and antimicrobial immunity. Although they express natural killer (NK) cell-associated receptors such as Killer-cell Immunoglobulin-like Receptors (KIRs), the relevance of KIR expression on γδ T cells remains largely unexplored. Using flow cytometry, ATAC-seq and RNA-seq, we identified KIR expression as a marker that distinguished two functionally and molecularly distinct γδ T cell subsets. KIR⁺ γδ T cells exhibited an advanced, memory-like differentiation state characterized by heightened cytotoxicity, stable epigenetic remodeling and a predominant IFNγ-producing profile. In contrast, KIR⁻ γδ T cells maintained a naïve-like phenotype and preferentially produced IL-17 upon polarization. Notably, KIR+ γδ T cells were consistently observed across individuals but were significantly enriched in cytomegalovirus (CMV)-seropositive donors, suggesting that chronic antigenic stimulation could promote the emergence of KIR⁺ effector γδ T cells. These findings reveal a functional dichotomy in human γδ T cells defined by KIR expression, linking IFNγ-driven cytotoxicity with KIR⁺ cells and IL-17 production with KIR⁻ cells. This insight advances our understanding of γδ T cell heterogeneity and has implications for viral immunity, immune memory and the development of γδ T cell-based immunotherapies.
Authors
Mahya Razmi, Yeganeh Almasi, Marilee Larrivée, Jonathan B. Angel, Alexandre Blais, Zakia Djaoud
Abstract
Inhibiting the mammalian target of rapamycin (mTOR) during acute viral infection generates highly functional memory CD8 T cells. We investigated the effects of inhibiting mTOR by using rapamycin during the effector and contraction phases of the immune response to a DNA prime and Modified Vaccinia Ankara (MVA) boost SIV vaccination in rhesus macaques. Rapamycin administered either during MVA boosts alone (DMR) or during both primes and boosts (DRMR) reduced the contraction of effector CD8 T cells, resulting in higher frequencies of SIV-specific memory CD8 T cells with enhanced quality as indicated by expression of Bcl-2 and CD127. Additionally, rapamycin reduced the frequency of proliferating CCR5+ CD4 T cells in the blood following the MVA boost. Post SIV251 infection, rapamycin-treated macaques demonstrated marked expansion of SIV-specific CD8 T cells (reaching up to 50% in blood and 25% in gut). The heightened expansion of SIV-specific CD8 T cells in the DMR group was associated with markedly lower (2-logs compared to unvaccinated and 1-log compared to DM) peak viral load in the gut and set-point viremia, along with improved survival post infection. Thus, inhibiting the mTOR pathway during MVA boosts of a DNA/MVA vaccine enhances vaccine efficacy by improving memory CD4 and CD8 T cell function.
Authors
Shanmugalakshmi Sadagopal, Kasey Stokdyk, Suefen Kwa, Rahul Basu, Sailaja Gangadhara, Rafi Ahmed, Smita S. Iyer, Koichi Araki, Rama Rao Amara
Abstract
Lipotoxicity associated with metabolic dysfunction-associated steatotic liver disease (MASLD) causes dysregulated fatty acid (FA) and glucose metabolism, inducing cellular energy imbalance, oxidative stress (OS), and hepatocellular injury. Interleukin (IL)-10 is altered in MASLD, including increased IL-10 transcripts in peripheral immune cells; however, its role in hepatic responses to lipotoxic stress remains unclear. We evaluated whether IL-10 treatment attenuates lipotoxic injury and MASLD-related phenotypes in vivo and in vitro to reveal MASLD treatment strategies. As MASLD models, in vivo high-fat diet mice and in vitro normal human hepatocytes under palmitic acid exposure, with confirmatory experiments in HepG2 cells, were used and treated with IL-10. We assessed FA and glucose metabolism, OS, and apoptosis with histological changes and mechanisms related to hepatocellular viability/metabolic activity and stress-responsive survival signaling in vitro. IL-10 modulated FA synthesis and β-oxidation, reducing lipid accumulation, and altered glucose metabolic pathways, consistent with improved glucose handling under lipotoxic stress. Furthermore, IL-10 reduced OS and cell death markers while enhancing antioxidant responses, consistent with hepatocellular protection. These data suggest that IL-10 attenuates lipotoxic injury by modulating hepatic response pathways, thereby improving MASLD-related phenotypes, and supports the potential of IL-10 as a therapeutic target for MASLD.
Authors
Akira Kado, Kazuya Okushin, Takeya Tsutsumi, Toshiyuki Kishida, Kazuhiko Ikeuchi, Hiroshi Yotsuyanagi, Kyoji Moriya, Kazuhiko Koike, Mitsuhiro Fujishiro
Abstract
IL-10–producing B cells exert immunosuppressive effects, yet their low abundance and poor in vitro viability have limited their therapeutic application. Here, we developed a stromal coculture system using MS5 cells engineered to express human CD40L, BAFF, and IFN-β1 (MS5-3F, for “3 factors”), which enables robust induction and greater than 1000-fold expansion of human IL-10–producing B cells. The expanded cells showed phenotypic and transcriptional profiles characteristic of unswitched (IgM+) plasmablasts and potently suppressed CD4+ T cell proliferation in an IL-10–dependent manner. MS5-3F–expanded B cells also increased the frequency of regulatory T cells in vitro, an effect that was not abrogated by IL-10/IL-10R blockade, suggesting contributions from additional mechanisms. IL-10 production originated predominantly from naive B cells, rather than memory B cells. Furthermore, B cells from patients with systemic lupus erythematosus, despite impaired IL-10 production under conventional conditions, were efficiently differentiated into IL-10–producing B cells using this system. The expanded cells showed minimal IgG-secreting output. Our platform offers a scalable strategy for generating human regulatory B cells, laying the foundation for B cell–based immunotherapies.
Authors
Ryo Kawakami, Keisuke Imabayashi, Akemi Baba, Yuichi Saito, Kazuhiko Kawata, Yutaro Yada, Airi Shibata, Rinka Ito, Ryo Kurasawa, Ryota Higuchi, Sungyeon Park, Hiroaki Niiro, Shinya Tanaka, Yoshihiro Baba
Abstract
Nearly 100 individuals have been identified who carry deleterious biallelic germline variants in CARD9 and experience life-threatening, invasive fungal infections caused by Ascomycetes but are otherwise resistant to other infectious agents. CARD9 is an adaptor protein expressed predominantly in myeloid cells, which functions downstream of dectin receptors, pattern recognition receptors for fungal antigens, to activate innate immune responses. The impact of CARD9 deficiency on lymphocytes, however, is less clear. We deciphered the functional consequences and delineated mechanisms of disease in a patient (P1) with a nonsense germline homozygous CARD9 variant (c.673A>T/p.K225*) and invasive Candida disease. P1’s PBMCs expressed truncated CARD9 and showed significantly reduced cytokine production in response to fungal ligands. P1 had reduced frequencies of circulating memory CD4+ TH17-like (CCR6+CXCR3–) cells. In addition, in vitro differentiation of P1’s naive CD4+ T cells into IL-17A/IL-17F–secreting cells was greatly impaired. Consistent with impaired responses of innate and adaptive immune cells from P1 in vitro, proportions of Candida-specific CD4+ T cells were strongly and selectively diminished. Our findings suggest that the CARD9 variant identified in P1 is pathogenic, affecting not only CARD9-induced immunity mediated by myeloid cells but also CD4+ T cell–intrinsic IL-17–dependent immunity and Candida-specific T cell responses.
Authors
Erika Della Mina, Carlos G. El-Haddad, Timothy A. West, Clara W.T. Chung, Jing Jing Li, Vivienne Lea, Elissa K. Deenick, Filomeen Haerynck, Jean-Laurent Casanova, Anne Puel, Cindy S. Ma, Stuart G. Tangye, Alisa Kane
Abstract
Vascularized skins were 3D printed using single donor human fibroblasts, pericytes, keratinocytes, and endothelial cells (ECs), the latter either unmodified (WT-ECs) or deleted of MHC molecules (KO-ECs). Adult MISTRG6 immunodeficient mice neonatally inoculated with adult human hematopoietic stem cells (HSCs) received printed skin allogeneic to the HSCs and were boosted 3 weeks after grafting with human PBMCs autologous to the HSCs. HSC inoculation alone produced low levels of circulating human myeloid and lymphoid cells without affecting grafts; PBMC boosting dramatically increased circulating human CD4+ T cells and boosted CD8+ T cells only in mice with WT-EC grafts. These grafts became infiltrated by human macrophages, dendritic cells, CD4+ and CD8+ T cells and showed evidence of rejection. Shared T cell clones were present in skin and spleen. KO-EC grafts had minimal infiltration of graft or spleen without rejection, despite MHC molecule expression on other graft cell types.
Authors
Zuzana Tobiasova, Esen Sefik, Lingfeng Qin, Jennifer M. McNiff, Gwendolyn Davis, Richard A. Flavell, W. Mark Saltzman, Jordan S. Pober
No posts were found with this tag.