Development
Abstract
Although inflammatory complications are common in preterm infants, the effects of these conditions on neonatal immune development remain poorly defined. We therefore investigated whether severe bronchopulmonary dysplasia (BPD) and systemic infection, two major complications of prematurity, produce distinct immune signatures and change immune composition over time. We performed longitudinal high-dimensional immune profiling of residual whole blood from 38 preterm infants sampled every two weeks, along with 10 term infants at birth. Preterm infants with severe BPD showed a progressive increase in Th17-polarized CD4+ T cells, neutrophils, and Th17-related cytokines compared to age-matched infants with moderate BPD. In contrast, some preterm infants with systemic bacterial or viral infections mounted exceptionally robust CD8+, CD4+, and γδ T cell responses, with oligoclonal expansion, terminal differentiation, and coordinated plasma cytokine shifts that persisted well beyond resolution of infection. These findings demonstrate that different preterm comorbidities imprint the neonatal immune system in divergent ways. Thus, comprehensive and longitudinal immune profiling may not only identify connections between clinical inflammatory complications and underlying immune pathways but also reveal potential targets for intervention.
Authors
Benjamin A. Fensterheim, Michelle L. McKeague, Divij Mathew, Shwetank, Ajinkya Pattekar, Matthew Lee, Zahabia Rangwala, Sean Nasta, Macy C. Kee, Cynthia Clendenin, Zachary Martinez, Caroline Diorio, Allison R. Greenplate, Krithika Lingappan, E. John Wherry
Abstract
X-linked myotubular myopathy (XLMTM) is a rare genetic disorder that typically presents at birth with progressive muscle weakness and respiratory difficulties and is caused by myotubularin-1 (MTM1) gene mutations. Here we examine the role of phosphatidylinositol-4-phosphate 3-kinase catalytic subunit type 2 beta (PIK3C2B), a lipid kinase that interacts with MTM1, in XLMTM in various models. We examined the effect of BLU3797, a novel, highly potent, selective, orally bioavailable PIK3C2B inhibitor, on survival, muscle development, myofiber phenotypes, and gene expression in MTM1-/y mice. PIK3C2B-deficient XLMTM animals demonstrated increased survival, restored muscle function, fewer myofibers with centralized nuclei, and normalization of disease-associated molecular markers. BLU3797 alleviated the XLMTM phenotype in a dose-dependent and reversible manner. Loss of functional PIK3C2B in XLMTM mice promoted a more differentiated, adult-like myofiber profile, which was strongly associated with normalization of disease surrogates and a reduction in markers of early muscle development and regeneration. BLU3797 treatment appears to modulate the expression of microRNAs associated with satellite cell activation and myofiber fusion. These findings indicate that PIK3C2B inhibition with BLU3797 effectively reverses the XLMTM disease phenotype by enhancing muscle function and promoting development toward a more mature state.
Authors
Andrew Shearer, Melissa L. Brooks, Maxine M. Chen, Thiwanka Samarakoon, John Hsieh, Gramoz Kondakci, Emanuele Perola, Jason Brubaker, Kristina Fetalvero, Stefanie Schalm, Joana Caetano-Lopes
Abstract
β-arrestins are ubiquitously expressed cytosolic adaptor proteins that regulate G protein-coupled receptor-dependent and -independent pathways essential for numerous physiological functions. This study investigated the role of β-arrestin1 and -2 in embryonic lymphatic vessel development and survival by generating and characterizing mice with lymphatic, tamoxifen-inducible loss of the genes encoding β-arrestin-1 and -2 (Arrb1/2ΔiLEC). At embryonic day15.5 (E15.5), Arrb1/2ΔiLEC embryos exhibit profound hydrops fetalis and increased embryonic mortality compared to control Arrb1/2fl/fl embryos. Edematous Arrb1/2ΔiLEC embryos, which were more often represented by the female sex, showed growth restriction and decreased lymphatic endothelial cell (LEC) proliferation in the jugular lymphatic sac compared to controls. In vitro knockdown of β-arrestin1 in LECs increased proliferation and increased activation of AKT, while knockdown of β-arrestin2 decreased proliferation and decreased activation of both ERK and CREB. Arrb1/2ΔiLEC embryos also exhibited dilated dermal lymphatics with decreased continuous VE-Cadherin adherens junctions compared to controls. These results were recapitulated in vitro in β-arrestin1 and/or -2 knockdown human LECs, which showed a decrease in membrane VE-Cadherin and β-catenin levels, and prevention of adrenomedullin-induced linearization of VE-cadherin at endothelial cell–cell junctions. Collectively, these results demonstrate that loss of β-arrestin1/2 in lymphatics causes hydrops fetalis, mid-gestational growth arrest and embryonic demise associated with reduced LEC proliferation and disrupted VE-Cadherin adherens junctions.
Authors
Yanna Tian, D. Stephen Serafin, Monserrat Avila-Zozaya, Alyssa M. Tauro, Natalie M. Torres-Valle, Bryan M. Kistner, Danielle M. Dy, Elizabeth S. Douglas, Kathleen M. Caron
Abstract
Sleep disturbance is a prevalent yet poorly understood comorbidity in autism spectrum disorders (ASD). Here, we uncover a bidirectional regulatory axis connecting the ASD risk gene POGZ to core circadian mechanisms. We demonstrate that Pogz is widely expressed in the suprachiasmatic nucleus (SCN), the central pacemaker of the circadian rhythms and exhibits circadian oscillations in both the hypothalamus and liver with its transcription directly regulated by the circadian molecule DBP through a D-box element in its proximal enhancer. Pogz-deficient mice exhibited prolonged circadian periodicity, impaired light-induced phase shift, delayed adaption to an 8-hour advance jet-lag, and reduced SCN c-Fos activation in response to light pulses. Mechanistically, POGZ interacts with and enhances the transcription activity of CREB, a key regulator of light-induced phase resetting. Notably, Pogz deletion leads to ASD-related deficits in social novelty and cognition, with cognitive impairments influenced by both photoperiod and behavioral paradigm. Our findings thus reveal a critical, previously unrecognized intersection between an ASD risk gene and circadian clock, offering new insights into the pathogenesis of core ASD symptoms and comorbid sleep disturbances.
Authors
Ting Wu, Jiao He, Chu-Jun Xu, Chi-Yu Li, Pingchuan Zhang, Yanfeng Wang, Shanshan Zhu, Lusi Zhang, Jingtan Zhu, Jing Zhang, Jia-Da Li, Huadie Liu
Abstract
Low nephron endowment constitutes a risk factor for hypertension and renal disease. Epigenetic regulation is crucial for nephron progenitor cell differentiation, affecting nephron number and renal function. The role of many epigenetic modulators, such as Lysine-specific histone demethylase 1a (LSD1 or KDM1A), remains unclear. We used Kdm1a-KO mice to demonstrate that Kdm1a depletion in nephron progenitor cells results in reduced kidney size in neonates and led to glomerulosclerosis, proteinuria, and renal cysts in adults. Notably, Kdm1a deletion in podocytes or tubular cells did not replicate these effects. CRISPR/Cas9-mediated KDM1A deletion in human kidney organoids caused cyst formation and altered gene expression, with snRNA-seq revealing downregulation of podocyte genes and upregulation of metabolic genes. The presence of noncoding RNAs indicated roles in cell proliferation. Our study reveals the critical role of Kdm1a function in nephron development and highlights its affect on transcriptional programming for long-term renal function and susceptibility to cyst formation.
Authors
Nicola Wanner, Julia Keller, Nastassia Liaukouskaya, Geoffroy Andrieux, Sandra D. Laufer, Manuel Rogg, Tillmann Bork, Wei Liang, Fabian Braun, Fabian Haas, Milagros N. Wong, Victor G. Puelles, Sydney E. Gies, Charlotte Meyer, Melanie Boerries, Martin Helmstädter, Oliver Kretz, Iris Hild, Eric Metzger, Roland Schüle, Wibke Bechtel-Walz, Tobias B. Huber
Abstract
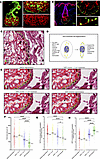
The cardiac conduction system (CCS) develops asymmetrically along the body axes. In heterotaxy syndrome—resulting from aberrant left–right (L–R) axis formation—atrial and atrioventricular conduction defects can cause life-threatening arrhythmias. However, the developmental mechanisms regulating the atrioventricular conduction system (AVCS) disposition and integrity remain unclear. To investigate the etiology of AVCS malformations in laterality defects, we analyzed CCS development and function in mouse mutants for Cryptic and Lefty1, which are key regulators of Pitx2 in the L–R axis formation. Cryptic–/– embryos exhibited bilateral sinoatrial (SA) nodes and an ectopic anterior AV node and bundle accompanied by reduced Pitx2 expression. In contrast, Lefty1–/– embryos showed a hypoplastic SA node and AV node–bundle dissociation with ectopic Pitx2 expression. Single-cell transcriptomic analysis of Pitx2–/– hearts revealed expansion of AV node and bundle populations, consistent with a repressive role of Pitx2 in AVCS specification. Genetic lineage tracing indicated that Pitx2-expressing cells from the left lateral plate mesoderm populate cranioventral cardiac regions, where AVCS development is suppressed. Together, these findings clarify how global L–R axis information is locally integrated to shape AVCS disposition and integrity, providing a mechanistic model for AVCS abnormalities in laterality-associated congenital heart disease.
Authors
Kunihiko Joo, Ryohei Matsuoka, Keiko Kitajima, Kenta Yashiro, Akira Shiose, Ryuji Tominaga, Michael M. Shen, Shinya Oki, Chikara Meno
Abstract
Proper development of the umbilical cord and placental vasculature is essential for embryonic development. While the allantois is known give rise to endothelial cells (ECs) within the placenta, whether the allantois gives rise to ECs in the umbilical cord is debated. Furthermore, a lack of genetic tools to study placental vascular development independent of the embryo proper has hindered robust investigation into the primary cause of vascular defects from early studies utilizing global knockouts. In this study, we delineate the contribution of the allantois to the umbilical vessels and utilize a mouse genetic tool previously developed by our lab to revisit the role of Notch signaling during placental development. We show that the allantois has mosaic contribution to the umbilical endothelium with higher contributions closer to the placenta. Allantoic deletion of Dll4 disrupts umbilical cord and placental vascular formation with secondary defects in the heart. Lastly, we identify Unc5b downstream of Notch signaling that restricts EC migration while promoting chemokine signaling for smooth muscle cell (SMC) recruitment to arteries. These findings identify a genetic tool for investigating placental vascular development and give new insights into the ontogeny and mechanisms of placental vascular and umbilical cord development.
Authors
Derek C. Sung, Hana A. Ahanger, Sweta Narayan, Jesse A. Pace, Mei Chen, Jisheng Yang, Siqi Gao, T.C.S. Keller IV, Jenna Bockman, Xiaowen Chen, Erica Nguyen, Alan T. Tang, Patricia Mericko-Ishizuka, Ivan Maillard, Mark L. Kahn
Abstract
Acne vulgaris is a common skin condition involving complex interactions among lipid-secreting sebaceous glands, keratinocytes, immune cells, and microbiota. While retinoids are effective for treating acne, disease pathogenesis remains poorly understood. In particular, it remains unclear how different subtypes of acne, including inflammatory (pustular) and noninflammatory (comedonal) lesions, vary in gene expression, signaling, and sebaceous gland involvement. Here, we performed spatial transcriptomics on healthy, nonlesional, comedonal, and pustular acne skin using a custom panel targeting sebaceous differentiation, lipid metabolism, and retinoid signaling pathways. We also designed a specialized segmentation pipeline to improve transcript assignment in the spatially complex sebaceous gland. Our analyses identified a PPARG+ transitional basal cell state in sebocytes and revealed that comedonal skin upregulates sebogenesis genes, whereas pustular skin downregulates sebogenesis. Both lesion types exhibited increased AP-1 transcription factors and elevated FABP5, a chaperone that blunts retinoic acid receptor signaling. Finally, we demonstrated that an AP-1 inhibitor, T-5224, downregulates FABP5 in human keratinocytes and reduces pustule formation in a mouse model of high-fat diet–induced folliculitis. Altogether, these findings indicate that altered lipogenesis, retinoid signaling, and keratinocyte differentiation are key features of acne, and nominate AP-1 and FABP5 as potential therapeutic targets.
Authors
Joseph S. Durgin, Natalia A. Veniaminova, Thomas J. Huyge, Shih-Ying Tsai, Jennifer Fox, Yuli Cai, Mrinal K. Sarkar, Lam C. Tsoi, Johann E. Gudjonsson, Sunny Y. Wong
Abstract
Mutations in LMNA, encoding nuclear lamina protein Lamin A/C, cause premature aging disorders, most notably Hutchinson-Gilford Progeria Syndrome. Despite obvious skull abnormalities in progeroid patients, the disease-causing mechanism remains elusive. The L648R single amino acid substitution blocks prelamin A maturation in mice, modeling a unique human patient. Here, we describe skull deformities in premature aging caused by aberrant suture fusion resembling those of patients with craniosynostosis. Further examinations identify prelamin A accumulation causatively linked to multiple suture synostoses in low bone density. This etiology is distinct from conventional suture fusion mediated by excessive ossification. In addition, the mutation disrupts skeletal stem cell stemness and subsequent stem cell-mediated proliferation and differentiation in osteogenesis. Intrasutural bones present in progeroid patients are highly reminiscent of synostosis caused by stem cell exhaustion. Comparative gene expression profiling further reveals cytoskeletal dynamics associated with skeletogenic cell aging and suture patency in mice and humans. Functional studies demonstrate that abnormal structures of progeric nuclei caused by prelamin A accumulation affect cytoskeleton organization and nucleoskeleton assembly essential for craniofacial skeletogenesis. Pharmacogenetic analyses indicate alleviation of osteogenic defects via actin polymerization. Our findings provide compelling evidence for nuclear and cytoskeletal defects, mediating stem cell-associated osteogenic deformities in progeroid disorders.
Authors
Kai Li, Trunee Hsu, Hitoshi Uchida, Tingxi Wu, Susan Michaelis, Howard J. Worman, Wei Hsu
Abstract
Lung development relies on diverse cell intrinsic and extrinsic mechanisms to ensure proper cellular differentiation and compartmentalization. In addition, it requires precise integration of multiple signaling pathways to temporally regulate morphogenesis and appropriate cell specification. To accomplish this, organogenesis relies on epigenetic and transcriptional regulators to promote cell fate and inhibit alternative cell fates. Using genetic mouse and human embryonic stem cell (hESC) differentiation models, tissue explants, and single-cell transcriptomic analysis, we demonstrated that Bromodomain Containing Protein 4 (BRD4) is required for mammalian lung morphogenesis and cell fate. Endodermal deletion of BRD4 impaired epithelial-mesenchymal crosstalk, leading to disrupted proximal-distal patterning and branching morphogenesis. Moreover, temporal deletion of BRD4 revealed developmental stage-specific defects in airway and alveolar epithelial cell specification with a predominant role in proximal airway cell fate. Similarly, BRD4 promoted lung endodermal cell differentiation into airway lineages in a hESC-derived lung organoid model. Together, these data demonstrated that BRD4 orchestrates early lung morphogenesis and separately regulates cell specification, indicating a multifunctional and evolutionarily conserved role for BRD4 in mammalian lung development.
Authors
Hongbo Wen, Derek C. Liberti, Prashant Chandrasekaran, Shahana Parveen, Kwaku K. Quansah, Mijeong Kim, Ana N. Lange, Abigail T. Marquis, Sylvia N. Michki, Annabelle Jin, MinQi Lu, Ayomikun A. Fasan, Sriyaa Suresh, Shawyon P. Shirazi, Lisa R. Young, Jennifer M.S. Sucre, Maria C. Basil, Rajan Jain, David B. Frank
No posts were found with this tag.