Hepatology
Abstract
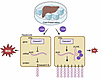
Hepatic ischemia-reperfusion injury (IRI) disrupts cellular signaling pathways and contributes to early allograft dysfunction (EAD) in orthotopic liver transplantation (OLT). In this study, we found that the hepatic RNA binding protein Human Antigen R (HuR) regulated the 3′ untranslated region (UTR) of Carcinoembryonic Antigen-Related Cell Adhesion Molecule 1 (Ceacam1) following ischemic stress. Hepatocyte-specific preinjury HuR-null mice exhibited elevated LDH-5 isoenzyme activity and reduced Ceacam1-S expression, reflecting tissue-specific injury. In situ hybridization demonstrated that the stability of Ceacam1 mRNA depended on HuR. Luciferase assays identified Ceacam1 3′UTR cis-elements responsive to high oxygen tension. HuR-targeting short-activating RNAs (saRNAs) preferentially induced the alternative splicing of Ceacam1-S. Antisense oligos directed to the Ceacam1 3′UTR protected WT mice against acute liver injury. In the clinical arm, increased HuR and CEACAM1 expression were associated with reduced proinflammatory phenotype and a lower incidence of EAD in patients with OLT (n = 164). Human discarded livers with elevated ELAVL1/CEACAM1 levels correlated with improved tissue homeostasis. These findings suggest that HuR regulation of Ceacam1 represents a key determinant of donor tissue quality and offers a potential target for future therapeutic strategies in OLT recipients.
Authors
Brian Cheng, Tristan D. Tibbe, Siyuan Yao, Megan Wei, Zeriel Y. Wong, Taylor Torgerson, Richard Chiu, Aanchal S. Kasargod, Kojiro Nakamura, Monica Cappelletti, Myung Sim, Douglas G. Farmer, Fady Kaldas, Jerzy W. Kupiec-Weglinski, Kenneth J. Dery
Abstract
Background & Aims Liver cirrhosis is characterized by chronic inflammation and fibrosis, with Th17 cells playing a crucial role in its progression. Recent evidence suggests that dietary salt influences immune diseases by modulating Th17 differentiation. This study assessed the impact of dietary salt on Th17-driven inflammation in patients with compensated cirrhosis and explored its effects on liver injury in mouse models. Methods A non-drug, open-label, non-randomized study involved 37 patients with compensated cirrhosis, who were given personalized guidelines to reduce salt intake over three months. Changes in Th17-driven inflammation and liver function markers were assessed at baseline and after salt restriction. In parallel, the impact of a high-salt diet on hepatic CD4+ T cells was analyzed in mouse models of acute liver injury and fibrosis. Results High salt intake was associated with Th17-mediated inflammation and correlated with markers of impaired liver function in these patients. Importantly, moderating salt intake through a personalized nutritional intervention was sufficient to reduce CD4+ T cell- mediated inflammation. Furthermore, analysis of RNA-seq data revealed enrichment of salt-induced Th17 gene signatures in both liver tissue and peripheral cells from patients with liver disease. Similarly, mice fed a high salt diet showed hepatic enrichment of Th17 cells and exacerbated liver fibrosis upon injury. Mechanistic studies revealed that high sodium conditions activated NF-κB and induced IL-6 production in hepatocytes, which may promote Th17 responses. Conclusion Dietary salt exacerbates Th17-driven inflammation and contributes to cirrhosis progression. Salt reduction may represent a viable therapeutic approach to manage inflammation in compensated cirrhosis.
Authors
Amalia Tzoumpa, Beatriz Lozano-Ruiz, Yin Huang, Joanna Picó, Alba Moratalla, María Teresa Pomares, Iván Herrera, Juanjo Lozano, María Rodríguez-Soler, Cayetano Miralles, Pablo Bellot, Paula Piñero, Fabián Tarín, Pedro Zapater, Sonia Pascual, José Manuel González-Navajas
Abstract
Autoimmune hepatitis (AIH) and primary biliary cholangitis (PBC) are autoimmune liver diseases with strong female predominance. They are caused by T cell–mediated injury of hepatic parenchymal cells, but the mechanisms underlying this sex bias are unknown. Here, we investigated whether testosterone contributes to T cell activation in women with PBC. Compared with sex- and age-matched healthy controls (n = 23), cisgender (cis) women with PBC (n = 24) demonstrated decreased testosterone serum levels and proinflammatory CD4+ T cell profile in peripheral blood. Testosterone suppressed the expression of TNF and IFN-γ by human CD4+ T cells in vitro. In trans men receiving gender-affirming hormone therapy (GAHT) (n = 25), testosterone affected CD4+ T cell function by inhibiting Th1 and Th17 differentiation and by supporting the differentiation into regulatory Treg. Mechanistically, we provide evidence for a direct effect of testosterone on T cells using mice with T cell–specific deletion of the cytosolic androgen receptor. Supporting a role for testosterone in autoimmune liver disease, we observed an improved disease course and profound changes in T cell states in a trans man with AIH/primary sclerosing cholangitis (PSC) variant syndrome receiving GAHT. We here report a direct effect of testosterone on CD4+ T cells that may contribute to future personalized treatment strategies.
Authors
Lara Henze, Nico Will, Dakyung Lee, Victor Haas, Christian Casar, Jasper Meyer, Stephanie Stein, Franziska Mangler, Silja Steinmann, Tobias Poch, Jenny Krause, Johannes Fuss, Johanna Schröder, Alexandra E. Kulle, Paul-Martin Holterhus, Stefan Bonn, Marcus Altfeld, Samuel Huber, Ansgar W. Lohse, Dorothee Schwinge, Christoph Schramm
Abstract
Oxidative stress driven by malfunctioning respiratory complex I (RC-I) is a crucial pathogenic factor in liver ischemia/reperfusion (I/R) injury. This study investigates the role of alkaline ceramidase 3 (ACER3) and its unsaturated long-chain ceramide (CER) substrates in regulating liver I/R injury through RC-I. Our findings demonstrated that I/R upregulated ACER3/Acer3 and decreased unsaturated long-chain CER levels in human and mouse livers. Both global and hepatocyte-specific Acer3 ablation, as well as treatment with CER(d18:1/18:1), led to a significant increase of CER(d18:1/18:1) levels in the liver, which mitigated the I/R-induced hepatocyte damage and inflammation in mice. Mechanistically, Acer3 modulated CER(d18:1/18:1) levels in mitochondria-associated membranes and endoplasmic reticulum (ER), thereby influencing the transport of CER(d18:1/18:1) from ER to mitochondria. Acer3 ablation and CER(d18:1/18:1) treatment elevated CER(d18:1/18:1) in mitochondria, where CER(d18:1/18:1) bound to the RC-I subunit Ndufa6 to inactivate RC-I and reduced reactive oxygen species production in the I/R-injured mouse liver. These findings underscore the role of CER(d18:1/18:1)-Ndufa6 interaction in suppressing RC-I-mediated oxidative-stress-driven pathogenesis in liver I/R Injury.
Authors
Kai Wang, Leyi Liao, Hanbiao Liang, Pengxiang Huang, Qingping Li, Baoxiong Zhuang, Chen Xie, Xiangyue Mo, Xuesong Deng, Jieyuan Li, Yang Lei, Minghui Zeng, Cungui Mao, Ruijuan Xu, Cuiting Liu, Xianqiu Wu, Jie Zhou, Biao Wang, Yiyi Li, Chuanjiang Li
Abstract
Biliary atresia (BA) is a pediatric liver disease that often necessitates parenteral nutrition (PN) to support growth due to impaired liver function. While soy oil lipid emulsions (SLE) are commonly used in PN, they may contribute to cholestatic liver injury. In contrast, mixed oil lipid emulsions (MLE) show promise in preventing cholestasis in non-BA infants, potentially by restoring bile flow. However, their effectiveness in cases of complete bile duct obstruction, as seen in BA, remains uncertain. To explore the potential benefits of MLE in BA, we utilized a neonatal pig model of bile duct ligation (BDL). Pigs underwent either BDL or sham surgery and were subsequently fed either MLE or SLE via PN, or enterally with formula. The MLE-BDL pigs exhibited significantly greater weight gain compared to those fed SLE or formula enterally. Additionally, MLE-BDL pigs showed higher serum bile acid and gamma-glutamyl transferase concentrations compared to SLE-BDL pigs. However, no significant differences in liver injury, assessed by ductular reaction or fibrosis, were observed between MLE- and SLE-BDL pigs. Based on weight gain alone, MLE may be a superior lipid emulsion for use in neonates with obstructive cholestasis.
Authors
Greg Guthrie, Caitlin Vonderohe, Valeria Meléndez Hebib, Barbara Stoll, Douglas Burrin
Abstract
Metabolic dysfunction–associated steatotic liver disease (MASLD) is the most common chronic liver disease worldwide for which there is only one approved treatment. Adenosine monophosphate–activated protein kinase (AMPK) is an interesting therapeutic target since it acts as a central regulator of cellular metabolism. Despite efforts to target AMPK, no direct activators have yet been approved for treatment of this disease. This study investigated the effect of the AMPK activator ATX-304 in a preclinical mouse model of progressive fatty liver disease. The data demonstrated that ATX-304 diminishes body fat mass, lowers blood cholesterol levels, and mitigates general liver steatosis and the development of liver fibrosis, but with pronounced local heterogeneities. The beneficial effects of ATX-304 treatment were accompanied by a shift in the liver metabolic program, including increased fatty acid oxidation, reduced lipid synthesis, as well as remodeling of cholesterol and lipid transport. We also observed variations in lipid distribution among liver lobes in response to ATX-304, and a shift in the zonal distribution of lipid droplets upon treatment. Taken together, our data suggested that ATX-304 holds promise as a potential treatment for MASLD.
Authors
Emanuel Holm, Isabeau Vermeulen, Saba Parween, Ana López-Pérez, Berta Cillero-Pastor, Michiel Vandenbosch, Silvia Remeseiro, Andreas Hörnblad
Abstract
BACKGROUND. Alterations in circulating metabolites have been described in obese metabolic dysfunction-associated steatotic liver disease (MASLD), but data on lean MASLD are lacking. We investigated serum metabolites, including microbial bile acids (BAs) and short-chain fatty acids (SCFAs), and their association with lean and obese MASLD. METHODS. Serum samples from 204 subjects of European descent were allocated to four groups: lean healthy (n=61), lean MASLD (n=49), obese healthy (n=47) and obese MASLD (n=47). LC/MS-based metabolomics was performed followed by linear model analysis. MASLD prediction was assessed based on LASSO regression. Functional effects of significantly altered molecules were confirmed in organotypic 3D primary human liver cultures. RESULTS. Lean MASLD was characterized by elevated isobutyrate, along with higher methionine sulfoxide, propionate and phosphatidylcholines. Patients with obese MASLD had increased sarcosine and decreased lysine and asymmetric dimethylarginine. Using metabolites, sex and body mass index, MASLD vs. healthy could be predicted with a median AUC of 86.5% and 85.6% in the lean and obese subgroups, respectively. Functional experiments in organotypic 3D primary human liver cultures showed that propionate and isobutyrate induced lipid accumulation and altered expression of genes involved in lipid and glucose metabolism. CONCLUSION. Our results indicate that lean MASLD is characterized by a distinct metabolite pattern related to amino acid metabolism, lipids and SCFAs, while metabolic pathways of lipid accumulation are differentially activated by microbial metabolites. Our findings highlight an important role of microbial metabolites in MASLD pathogenesis, with implications for the predictive and mechanistic assessment of liver disease across different weight categories. FUNDING. The work received funding from the Robert Bosch Stiftung, Stuttgart, Germany, the Swedish Research Council [grant numbers 2021-02801, 2023-03015 and 2024-03401], the ERC Consolidator Grant 3DMASH [101170408], Ruth and Richard Julin Foundation for Gastroenterology [grant number 2021-00158], the SciLifeLab and Wallenberg National Program for Data-Driven Life Science [WASPDDLS22:006], and the Novo Nordisk Foundation [NNF23OC0085944 and NNF23OC0084420]. JT was supported by PMU-FFF [grant number E-18/28/148-FEL].
Authors
Mathias Haag, Stefan Winter, Aurino M. Kemas, Julia Tevini, Alexandra Feldman, Sebastian K. Eder, Thomas K. Felder, Christian Datz, Bernhard Paulweber, Gerhard Liebisch, Oliver Burk, Volker M. Lauschke, Elmar Aigner, Matthias Schwab
Abstract
Metabolic dysfunction-associated steatotic liver disease (MASLD)—characterized by excess accumulation of fat in the liver—now affects one third of the world’s population. As MASLD progresses, extracellular matrix components including collagen accumulate in the liver causing tissue fibrosis, a major determinant of disease severity and mortality. To identify transcriptional regulators of fibrosis, we computationally inferred the activity of transcription factors (TFs) relevant to fibrosis by profiling the matched transcriptomes and epigenomes of 108 human liver biopsies from a deeply characterized cohort of patients spanning the full histopathologic spectrum of MASLD. CRISPR-based genetic knockout of the top 100 TFs identified ZNF469 as a regulator of collagen expression in primary human hepatic stellate cells (HSCs). Gain- and loss-of-function studies established that ZNF469 regulates collagen genes and genes involved in matrix homeostasis through direct binding to gene bodies and regulatory elements. By integrating multiomic large-scale profiling of human biopsies with extensive experimental validation we demonstrate that ZNF469 is a transcriptional regulator of collagen in HSCs. Overall, these data nominate ZNF469 as a previously unrecognized determinant of MASLD-associated liver fibrosis.
Authors
Sebastian Steinhauser, David Estoppey, Dennis P. Buehler, Yanhua Xiong, Nicolas Pizzato, Amandine Rietsch, Fabian Wu, Nelly Leroy, Tiffany Wunderlin, Isabelle Claerr, Philipp Tropberger, Miriam Müller, Alexandra Vissieres, Lindsay M. Davison, Eric H. Farber-Eger, Quinn S. Wells, Quanhu Sheng, Sebastian Bergling, Sophia A Wild, Pierre Moulin, Jiancong Liang, Wayne J. English, Brandon Williams, Judith Knehr, Marc Altorfer, Alejandro Reyes, Johannes Voshol, Craig Mickanin, Dominic Hoepfner, Florian Nigsch, Mathias Frederiksen, Charles R. Flynn, Barna D. Fodor, Jonathan D. Brown, Christian Kolter
Abstract
The functional plasticity of tumor-infiltrating B (TIL-B) cells spans from anti-tumor responses to non-canonical immune suppression. Yet, how tumor microenvironment (TME) influences TIL-B development is still underappreciated. Our current study integrated single cell transcriptomics and BCR (B cell receptor) sequencing to profile TIL-B phenotypes and clonalities in hepatocellular carcinoma (HCC). Using trajectory and gene regulatory network analysis, we were able to characterize plasma cells, memory and naïve B cells within the HCC TME and further revealed a downregulation of BCR-signaling genes in plasma cells and a subset of inflammatory TNF+ memory B cells. Within the TME, non-switch memory B cell subset acquires an age-associated B cell phenotype (TBET+, CD11c+) and expressed higher levels of PD-L1, CD25 and granzyme B. We further demonstrated that the presence of HCC tumor cells could confer suppressive functions on peripheral blood B cells which in turn, dampen T cell co-stimulation. To the best of our knowledge, these findings represent novel mechanisms of non-canonical immune suppression in HCC. While previous studies identified atypical memory B cells in chronic hepatitis and across several solid cancer types, we further highlighted their potential role as regulatory B cells (Bregs) within both the TME and peripheral blood of HCC patients.
Authors
Shi Yong Neo, Timothy Wai Ho Shuen, Shruti Khare, Joni Chong, Maichan Lau, Niranjan Shirgaonkar, Levene Chua, Junzhe Zhao, Keene Lee, Charmaine Tan, Rebecca Ba, Janice Lim, Joelle Chua, Hui Shi Cheong, Hui Min Chai, Chung Yip Chan, Alexander Yaw Fui Chung, Peng Chung Cheow, Prema Raj Jeyaraj, Jin Yao Teo, Ye Xin Koh, Aik Yong Chok, Pierce Kah Hoe Chow, Brian Goh, Wei Keat Wan, Wei Qiang Leow, Tracy Jie Zhen Loh, Po Yin Tang, Jayanthi Karunanithi, Nye Thane Ngo, Tony Kiat Hon Lim, Shengli Xu, Ramanuj Dasgupta, Han Chong Toh, Kong-Peng Lam
Abstract
Authors
Jing Zeng, Derrick Zhao, Grayson Way, Andrew Fagan, Michael Fuchs, Puneet Puri, Brian C. Davis, Xuan Wang, Emily C. Gurley, Phillip B. Hylemon, Jian-Gao Fan, Masoumeh Sikaroodi, Patrick M. Gillevet, Huiping Zhou, Jasmohan S. Bajaj
No posts were found with this tag.