Hepatology
Abstract
Serine-rich splicing factor 3 (SRSF3) is crucial for the metabolic functions of the liver. The genetic deletion of SRSF3 in mouse hepatocytes impairs hepatic lipid and glucose metabolism and leads to fibrosis and formation of hepatocellular adenoma that progresses to hepatocellular carcinoma. SRSF3 protein is proteosomally degraded in metabolic-dysfunction associated fatty liver disease (MAFLD) and metabolic-dysfunction-associated steatohepatitis (MASH). We show here that depleting SRSF3 protein in hepatocytes promoted R-loop accumulation and increased DNA damage in the liver. Prevention of SRSF3 degradation in vivo protected hepatocytes from DNA double-strand breaks in mice with MASH. This protection extended to other DNA-damaging agents such as camptothecin, palmitic acid, or hydrogen peroxide when tested on HepG2 cells in vitro. SRSF3 interacted with TRIM28 and MDC1, which are components of the ATM DNA-damage repair complex, and knockdown of any of these 3 proteins reduced the expression of the other 2 proteins, suggesting they form a functional complex. Lastly, by preventing degradation of SRSF3, we were able to reduce tumors in a diethyl-nitrosamine–induced (DEN-induced) model of cirrhotic HCC. These findings suggest that maintenance of SRSF3 protein stability is crucial for preventing DNA damage and protecting liver from early metabolic liver disease and progression to HCC.
Authors
Panyisha Wu, Manasi Das, Yanting Wang, Yichun Ji, Yuli Wu, Deepak Kumar, Lily J. Jih, Nicholas J.G. Webster
Abstract
Neutrophils play a pivotal role in the progression of metabolic dysfunction–associated steatohepatitis (MASH) by mediating inflammatory responses. However, the heterogeneity of neutrophil subsets in MASH and their specific contributions to disease progression remain unclear. In this study, analysis of liver biopsies from 265 patients revealed a strong association between elevated neutrophil counts and MASH severity, particularly fibrosis. Five distinct neutrophil subsets were identified in human liver tissue, with PAD4+ neutrophils serving as key drivers in MASH progression. Mechanistically, PAD4+ neutrophils generate neutrophil extracellular traps (NETs) and activate hepatic stellate cells via the TAOK1-dependent MAPK signaling pathway. Inhibition of PAD4+ neutrophils in vivo attenuated the progression of liver fibrosis without exacerbating liver injury. Collectively, these findings elucidate the pivotal involvement of PAD4+ neutrophils in MASH progression and identify them as promising therapeutic targets for mitigating fibrosis and inflammation.
Authors
Jiajia Shen, Shanshan Huang, Yaohui Wang, Qingyuan Wang, Shibo Lin, Wei Guan, Yingyun Gong, Yiming Si, Ming Zhao, Hongwen Zhou, Hui Liang
Abstract
Next generation sequencing can identify previously uncharacterized gene expression patterns in disease. Beyond differentially expressed genes analysis, we investigated the ability of within-population diversity (α-diversity) of the transcriptome to reveal additional biological information in alcohol-associated liver disease (ALD), comparing Differential Shannon diversity (DSD) to transcriptome heterogeneity changes. RNA sequencing data from normal livers and patients with early ALD and severe AH were analyzed. α-diversity indices and Percent Shannon Diversity of a gene, which refers to this gene's contribution to total Shannon entropy, were calculated. Ingenuity pathway analysis identified canonical pathways determined by differentially expressed genes (DEG) and DSD approaches. ALD significantly decreased hepatic transcriptome α-diversity correlating with increased relative contribution of select genes. These changes were driven by lower abundance gene expression loss. DEG and DSD analyses showed overlapping genes and canonical pathways, but DSD also identified additional genes and pathways not highlighted by DEG, including fatty acid oxidation, extracellular matrix degradation, and cholesterol metabolism pathways that may represent additional therapeutic targets. Importantly, DSD more effectively identified differences between ASH and AH. Overall, α-diversity analysis revealed that ALD progressively reduces transcriptome heterogeneity, and that DSD provides complementary insights into disease mechanisms missed by standard approaches.
Authors
Sudrishti Chaudhary, Jia-Jun Liu, Silvia Liu, Marissa Di, Juliane I. Beier, Ramon Bataller, Josepmaria Argemi, Panayiotis V. Benos, Gavin E. Arteel
Abstract
Iron regulatory protein 1 (IRP1) is a post-transcriptional regulator of cellular iron metabolism. In mice, loss of IRP1 causes polycythemia through translational de-repression of hypoxia-inducible factor 2α (HIF2α) mRNA, which increases renal erythropoietin production. Here we show that Irp1-/- mice develop fasting hypoglycemia and are protected against high-fat diet–induced hyperglycemia and hepatic steatosis. Discovery-based proteomics of Irp1-/- livers revealed a mitochondrial dysfunction signature. Seahorse flux analysis in primary hepatocytes and differentiated skeletal muscle myotubes confirmed impaired respiratory capacity, with a shift from oxidative phosphorylation to glycolytic ATP production. This metabolic rewiring was associated with enhanced insulin sensitivity and increased glucose uptake in skeletal muscle. Under metabolic stress, IRP1 deficiency altered the redox balance of mitochondrial iron, resulting in inefficient energy production and accumulation of amino acids and metabolites in skeletal muscle, rendering them unavailable for hepatic gluconeogenesis. These findings identify IRP1 as a critical regulator of systemic energy homeostasis.
Authors
Wen Gu, Nicole Wilkinson, Carine Fillebeen, Darren Blackburn, Korin Sahinyan, Eric Bonneil, Tao Zhao, Zhi Luo, Vahab Soleimani, Vincent Richard, Christoph H. Borchers, Albert Koulman, Benjamin Jenkins, Bernhard Michalke, Hans Zischka, Judith Sailer, Vivek Venkataramani, Othon Iliopoulos, Gary Sweeney, Kostas Pantopoulos
Abstract
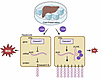
Recombinant hepatitis B surface antigen (rHBsAg) vaccine with various adjuvants fails to break T and B cell tolerance in hosts with chronic hepatitis B (CHB). This study aims to explore the mechanisms to break immune tolerance that allows the host to respond to rHBsAg, achieving a cure for CHB. We engineered an anti–PD-L1–IFN-α (aPD-L1–IFN-α) heterodimeric fusion protein to allow rHBsAg to rejuvenate T and B cell responses in hepatitis B virus–tolerant (HBV-tolerant) mice. S.c. coimmunization with aPD-L1–IFN-α and rHBsAg significantly enhanced antigen uptake and maturation of both macrophage and dendritic cell (DC) subsets in draining lymph nodes. Macrophages drove early B cell activation, while cDC1s primed CD8+ T cells, breaking tolerance and leading to both B cell and cytotoxic T lymphocyte (CTL) differentiation. This strategy elicited not only anti-HBsAg neutralizing antibodies but also HBsAg-specific CD8+ T cell responses, achieving a functional cure without systemic toxicity. The efficacy of the aPD-L1–IFN-α adjuvant depended on both PD-L1 cis-targeting and IFN-α receptor signaling in antigen-presenting cells. These findings establish aPD-L1–IFN-α as a translatable adjuvant to break the strong tolerance induced by CHB, providing a dual-pathway strategy to induce HBV-specific T and B cell responses.
Authors
Chao-Yang Meng, Yong Liang, Longxin Xu, Hongjia Li, Jingya Guo, Hairong Xu, Fan Wang, Yang-Xin Fu, Hua Peng
Abstract
Toll-like receptor 7 (TLR7) agonists are promising immunostimulatory agents for the treatment of chronic infections and cancer. However, their systemic toxicity remains a challenge. In this study, SA-5, a novel liver-targeted, orally available TLR7 agonist, was evaluated for pharmacokinetics, safety, and efficacy in young and aged macaques across 1–10 mg/kg repeated doses. Safety was evaluated through hematologic, biochemical, and flow cytometric profiling, while efficacy was assessed via IFN-α production, gene expression of interferon-stimulated genes, and plasmacytoid dendritic cell activation. A principal component analysis (PCA)-based composite scoring system was used to integrate multimodal parameters. SA-5 induced dose-dependent type I IFN with limited systemic inflammation, with 3 mg/kg showing optimal balance. SA-5 had comparable immunostimulatory activity to GS-9620 but with reduced adverse biomarker shifts. In aged macaques, efficacy was maintained with modestly increased safety responses. These findings support SA-5 as a safer next-generation TLR7 agonist effective across age groups, highlighting integrated biomarker profiling in preclinical immunomodulatory drug development.
Authors
Shokichi Takahama, Takahiro Tomiyama, Sachiyo Yoshio, Yuta Nagatsuka, Hirotomo Murakami, Takuto Nogimori, Mami Kochi, Shoko Ochiai, Hidenori Kimura, Akihisa Fukushima, Tatsuya Kanto, Takuya Yamamoto
Abstract
Authors
Carolina M. Larrain, Jack H. Victory, Priyanka P. Desai, Lindsay R. Friedman, Hannah Stepp, Rachel Ashe, Kirsten Remmert, Surajit Sinha, Emily C. Smith, Nicole Russell, Tracey Pu, Alyssa V. Eade, Justine F. Burke, Jason Ho, Michael B. Yaffe, David E. Kleiner, Keith Schmidt, William D. Figg, Jonathan M. Hernandez
Abstract
Chronic liver injury results in activation of quiescent Hepatic Stellate Cells (qHSCs) into Collagen Type I-producing activated HSCs that make liver fibrotic. We identified ETS1/2 (E26 transformation-specific transcription factors 1/2) as lineage-specific transcription factors regulating HSC phenotypes. Here we investigated the role of ETS1/2 in HSCs in liver fibrosis using toxic liver injury models and 3D human liver spheroids. Liver fibrosis was induced in wild-type and HSC-specific Ets1 (Ets1ΔHSC) and Ets2 (Ets2ΔHSC) knockout mice by administration of carbon tetrachloride for 6 weeks, following cessation of liver injury for 2 weeks. Liver fibrosis was more severe in Ets1ΔHSC, and to lesser extent in Ets2ΔHSC, compared to wild-type mice. Regression of liver fibrosis was suppressed only in Ets1ΔHSC, indicating Ets1 as the predominant isoform maintaining quiescent-like phenotype in HSCs. Similar results were obtained in a MASH model using 3D human liver spheroids. Knockdown of ETS1 in human HSCs caused upregulation of fibrogenic genes in MASH human liver spheroids and prevented fibrosis regression. ETS1 regulated the qHSC phenotype via CRTC2/PGC1α/PPARγ pathway. Knockdown of CRTC2 (cAMP response element-binding protein (CREB)-regulated transcription co-activator 2) abrogated PPARγ responses and facilitated HSC activation. These findings suggest that ETS1 may represent a therapeutic target for anti-fibrotic therapy.
Authors
Wonseok Lee, Xiao Liu, Sara Brin Rosenthal, Charlene Miciano, Sadatsugu Sakane, Kanani Hokutan, Debanjan Dhar, Hyun Young Kim, David A. Brenner, Tatiana Kisseleva
Abstract
Genetic variants in lipid metabolism influence the risk of developing metabolic dysfunction-associated steatotic liver disease (MASLD), cirrhosis, and end-stage liver disease (ESLD). The mechanisms by which these variants drive disease are poorly understood. Because of the PNPLA3-I148M variant's strong correlation with all stages of the MASLD spectrum and the lack of tractable therapeutic targets, we sought to understand its impact on cellular function and liver metabolism. Primary human hepatocytes (HAH) and iPSC-derived hepatocytes (iHeps) from healthy individuals possessing the PNPLA3-I148M mutation were characterized for changes in lipid metabolism, cellular stress, and survival. Using lipidomics, metabolomics, stable isotope tracing, and flux propensity analysis, we created a comprehensive metabolic profile of the changes associated with the PNPLA3-I148M variant. Functional analysis showed that the presence of the PNPLA3-I148M variant increased endoplasmic reticulum stress, mitochondrial dysfunction, and peroxisomal β-oxidation, ultimately leading to cell death via ferroptosis. Nutritional interventions, ferroptosis-specific inhibitors, and genetic approaches modulating GPX4 activity in PNPLA3-I148M HAH and iHeps decreased programmed cell death. Our findings indicate that therapies targeting ferroptosis in patients carrying the PNPLA3-I148M variant could affect the development of MASLD and ESLD and highlight the utility of iPSC-based models for the study of genetic contributions to hepatic disorders.
Authors
Rodrigo M. Florentino, Olamide Animasahun, Nils Haep, Minal Nenwani, Kehinde Omoloja, Leyla Nurcihan Altay, Abhinav Achreja, Kazutoyo Morita, Takashi Motomura, Ricardo Diaz-Aragon, Lanuza AP Faccioli, Yiyue Sun, Zhenghao Liu, Zhiping Hu, Bo Yang, Fulei Wuchu, Ajay Shankaran, Miya Paserba, Annalisa M. Baratta, Shohrat Arazov, Zehra N. Kocas-Kilicarslan, Noah Meurs, Jaideep Behari, Edgar N. Tafaleng, Jonathan Franks, Alina Ostrowska, Takahiro Tomiyama, Kyohei Yugawa, Akinari Morinaga, Zi Wang, Kazuki Takeishi, Dillon C. Gavlock, Mark Miedel, D. Lansing Taylor, Ira J. Fox, Tomoharu Yoshizumi, Deepak Nagrath, Alejandro Soto-Gutierrez
Abstract
Hepatic ischemia-reperfusion injury (IRI) disrupts cellular signaling pathways and contributes to early allograft dysfunction (EAD) in orthotopic liver transplantation (OLT). In this study, we found that the hepatic RNA binding protein Human Antigen R (HuR) regulated the 3′ untranslated region (UTR) of Carcinoembryonic Antigen-Related Cell Adhesion Molecule 1 (Ceacam1) following ischemic stress. Hepatocyte-specific preinjury HuR-null mice exhibited elevated LDH-5 isoenzyme activity and reduced Ceacam1-S expression, reflecting tissue-specific injury. In situ hybridization demonstrated that the stability of Ceacam1 mRNA depended on HuR. Luciferase assays identified Ceacam1 3′UTR cis-elements responsive to high oxygen tension. HuR-targeting short-activating RNAs (saRNAs) preferentially induced the alternative splicing of Ceacam1-S. Antisense oligos directed to the Ceacam1 3′UTR protected WT mice against acute liver injury. In the clinical arm, increased HuR and CEACAM1 expression were associated with reduced proinflammatory phenotype and a lower incidence of EAD in patients with OLT (n = 164). Human discarded livers with elevated ELAVL1/CEACAM1 levels correlated with improved tissue homeostasis. These findings suggest that HuR regulation of Ceacam1 represents a key determinant of donor tissue quality and offers a potential target for future therapeutic strategies in OLT recipients.
Authors
Brian Cheng, Tristan D. Tibbe, Siyuan Yao, Megan Wei, Zeriel Y. Wong, Taylor Torgerson, Richard Chiu, Aanchal S. Kasargod, Kojiro Nakamura, Monica Cappelletti, Myung Sim, Douglas G. Farmer, Fady Kaldas, Jerzy W. Kupiec-Weglinski, Kenneth J. Dery
No posts were found with this tag.