Endocrinology
Abstract
Germline and somatic changes in DICER1 and DGCR8 microprocessors confer risk of developing benign and malignant thyroid lesions, yet the molecular events driving malignant transformation remain unclear. We trace the molecular trajectories from benignity to malignancy in DICER1- and DGCR8-mutated thyroid lesions using multiomic profiling on over 30 DICER1-/DGCR8-mutated samples. Our findings reveal a progressive, specific, and linear accumulation of genetic changes, which when combined with enhanced downregulation of miRNAs distinguished DICER1-/DGCR8-malignant lesions from their benign counterparts. Compensatory hypomethylation of miRNA-encoding genes characterized DICER1-/DGCR8-benign lesions, but as the tumors progressed to malignancy, methylation was partly reimposed, reversing the attempts to activate miRNA-encoded genes and further compromising miRNA production. Transcriptomic analyses revealed mutation-specific effects on the microenvironment, whereby DICER1 mutations activated canonical thyroid cancer progression pathways, whereas altered DGCR8 associated with immune-related changes. This work unveils specific molecular events underlying malignant progression of miRNA-biogenesis-related thyroid tumors and identifies potential biomarkers and disease etiology mechanisms.
Authors
Anne-Sophie Chong, Carla Roca, Paula Morales-Sánchez, Eduard Dorca, Verónica Barea, Ignacio Ruz-Caracuel, Pablo Valderrabano, Carlota Rovira, Cristina Jou, Dorothée Bouron-Dal Soglio, Rebecca D. Chernock, Giovana T. Torrezan, Marc Pusztaszeri, José M. Cameselle-Teijeiro, Xavier Matias-Guiu, Clara V. Alvarez, Héctor Salvador, Jonathan D. Wasserman, Luis Javier Leandro-García, William D. Foulkes, Eduardo Andrés-León, Paula Casano-Sancho, Barbara Rivera
Abstract
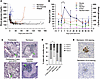
Mechanisms responsible for skeletal muscle kidney crosstalk have not been defined. We have determined that a circulating mediator, signal regulatory protein α (SIRPα), impairs intracellular insulin-mediated functions. To elucidate the effect of myokine SIRPα on diabetic kidney disease (DKD), flox mice and muscle-specific (m-specific) SIRPα-KO mice were subjected to an obesity-induced model of diabetes, high-fat diet (HFD; 60%) or insulin-deficient hyperglycemia model, streptozotocin (STZ), and were subsequently exposed to anti-SIRPα monoclonal antibodies. In the obesity-induced diabetic mice, serum SIRPα increased. Genetic deletion of muscle SIRPα protected against obesity and improved intracellular insulin signaling in muscle and adipose tissue, with reduced intramuscular fat deposition when compared with flox mice on HFD. Moreover, mSIRPα-KO mice displayed enhanced kidney tubular fatty acid oxidation (FAO) expression with suppressed intraorgan triglycerides deposition, and importantly, protection against DKD. Conversely, exogenous SIRPα impaired kidney proximal tubular cell FAO, ATP production, and exacerbated fibrosis. Finally, suppressing SIRPα in skeletal muscles or treatment with anti-SIRPα monoclonal antibodies in STZ-treated mice mitigated cachexia, hyperlipidemia, kidney triglyceride deposition, and renal dysfunction in spite of significant hyperglycemia. Importantly, serum SIRPα was upregulated in patients with DKD. In conclusion, SIRPα serves as a potential biomarker and therapeutic target in DKD.
Authors
Jiao Wu, Elisa Russo, Daniela Verzola, Qingtian Li, Helena Zhang, Bhuvaneswari Krishnan, David Sheikh-Hamad, Zhaoyong Hu, William E. Mitch, Sandhya S. Thomas
Abstract
Treatment with anti-CD3 monoclonal antibody (mAb) can delay or prevent type 1 diabetes in mice and humans by modulating the immune-mediated destruction of β cells. A single course of treatment may have lasting efficacy, but the mechanisms that account for these prolonged effects, i.e., “operational tolerance,” are not clear. Here, we used paired single-cell RNA and T cell receptor sequencing to characterize islet-infiltrating T cells and their counterpart in paired pancreatic lymph nodes from anti-CD3 mAb–treated nonobese diabetic (NOD) mice in remission. We found that after anti-CD3 mAb treatment, T cells that infiltrate the islets are more heterogeneous and have hybrid features including characteristics of T stem cell–like memory and reduced effector function compared with those from untreated prediabetic NOD mice. Autoantigen-reactive CD8+ T cells persist after treatment, but they also show features of stemness and reduced pathogenicity. Our findings describe the reshaping of islet-infiltrating and autoreactive T cells and β cells that lead to operational, but tenuous, tolerance to autoimmune diabetes following anti-CD3 mAb treatment.
Authors
Ying Wu, Maxwell Spurrell, Ana Lledó-Delgado, Songyan Deng, Dejiang Wang, Yang Liu, Mahsa Nouri Barkestani, Ana Luisa Perdigoto, Kevan C. Herold
Abstract
Serine-rich splicing factor 3 (SRSF3) is crucial for the metabolic functions of the liver. The genetic deletion of SRSF3 in mouse hepatocytes impairs hepatic lipid and glucose metabolism and leads to fibrosis and formation of hepatocellular adenoma that progresses to hepatocellular carcinoma. SRSF3 protein is proteosomally degraded in metabolic-dysfunction associated fatty liver disease (MAFLD) and metabolic-dysfunction-associated steatohepatitis (MASH). We show here that depleting SRSF3 protein in hepatocytes promoted R-loop accumulation and increased DNA damage in the liver. Prevention of SRSF3 degradation in vivo protected hepatocytes from DNA double-strand breaks in mice with MASH. This protection extended to other DNA-damaging agents such as camptothecin, palmitic acid, or hydrogen peroxide when tested on HepG2 cells in vitro. SRSF3 interacted with TRIM28 and MDC1, which are components of the ATM DNA-damage repair complex, and knockdown of any of these 3 proteins reduced the expression of the other 2 proteins, suggesting they form a functional complex. Lastly, by preventing degradation of SRSF3, we were able to reduce tumors in a diethyl-nitrosamine–induced (DEN-induced) model of cirrhotic HCC. These findings suggest that maintenance of SRSF3 protein stability is crucial for preventing DNA damage and protecting liver from early metabolic liver disease and progression to HCC.
Authors
Panyisha Wu, Manasi Das, Yanting Wang, Yichun Ji, Yuli Wu, Deepak Kumar, Lily J. Jih, Nicholas J.G. Webster
Abstract
Activation of lung fibroblasts in response to epithelial injury and inflammation provokes pulmonary fibrosis (PF). Endogenous molecular brakes counteracting fibroblast activity can be targets for therapies. Preclinical studies of synthetic C-type natriuretic peptide (CNP) indicated that this hormone might provide such a brake. As shown here, CNP exerts antifibrotic effects in cultured lung fibroblasts as well as precision cut lung slices from patients with PF, supporting clinical relevance. Therefore, augmenting or supplementing endogenous CNP could improve the treatment of such patients. To unravel whether paracrine CNP counteracts inflammation-driven PF, we studied mice with fibroblast-restricted knock-out of guanylyl-cyclase-B (GC-B), its cGMP-synthesizing receptor. Fibroblast GC-B-KO mice had enhanced bleomycin-induced lung inflammation, with increased expression of proinflammatory, profibrotic cytokines. Nevertheless, subsequent PF was not exacerbated. Molecular studies revealed that inflammation led to inhibition of CNP signaling in resident myofibroblasts, namely GC-B downregulation and induction of CNP/cGMP-degrading pathways. Despite this, a single subcutaneous injection of the recently developed long-acting CNP analog, MS~[Gln6,14]CNP-38, abrogated experimental lung inflammation and fibrosis. We conclude that CNP signaling in lung fibroblasts has anti-inflammatory and antifibrotic effects. Attenuation of this endogenous brake participates in the pathogenesis of PF and rescuing this pathway with long-acting CNP-analogs may have therapeutic potential.
Authors
Rene Weyer, Katharina Völker, Tamara Potapenko, Lisa Krebes, Marco Abesser, Anna-Lena Friedrich, Eva Lessmann, Ali Khadim, Clemens Ruppert, Elie El Agha, Dalia Sheta, Andreas Beilhack, Daniel V. Santi, Eric L. Schneider, Michaela Kuhn, Swati Dabral
Abstract
Obesity and type 2 diabetes (T2D) are metabolic diseases with increasing prevalence worldwide. Obesity often leads to T2D. Insulin resistance and impaired β cell function contribute to the onset of hyperglycemia. Previously, we reported that ablation of Gc, encoding a secreted protein with a primary role in vitamin D transport, improved pancreatic β cell function in models of diet-induced insulin resistance. Here, we show that Gc ablation had systemic insulin-sensitizing effects to prevent weight gain, hyperglycemia, and glucose intolerance; lower nonesterified fatty acids and triglycerides; and augment glucose uptake in skeletal muscle and adipose in male mice fed a high-fat diet. Interestingly, weight loss in Gc-ablated mice resulted from selective fat mass loss with preserved lean mass. Moreover, acute Gc inhibition prevented glucose intolerance caused by high-fat feeding. The data suggest that Gc inhibition can increase insulin production in β cells and insulin action in peripheral tissues, while reducing fat mass.
Authors
Richard Gill, Taiyi Kuo
Abstract
Autoimmune diabetes encompasses rapidly progressive type 1 diabetes mellitus (T1D) and indolent latent autoimmune diabetes in adults (LADA), representing distinct inflammatory set points along a shared autoimmune spectrum. Yet the immunological mechanisms that determine these divergent inflammatory states remain unresolved. We performed single-cell RNA sequencing with paired T and B cell receptor profiling on over 400,000 peripheral blood mononuclear cells (PBMCs) from patients with LADA, newly diagnosed T1D, and healthy controls. PBMC composition was comparable across cohorts, indicating that qualitative rather than quantitative immune differences underlie disease heterogeneity. In T1D, pan-lineage activation of NF-κB, EGFR, MAPK, and hypoxia pathways, coupled with a TNF-centered communication hub, enhanced MHC signaling, and disrupted adhesion, promoted systemic inflammation. LADA, by contrast, exhibited global suppression of NF-κB/EGFR activity, retention of moderate JAK/STAT tone, reinforced natural killer cell inhibitory checkpoints via HLA-C–KIR2DL3/3DL1 interaction, and stabilized CD8⁺ T cell synapses through HLA-C–CD8 binding, collectively restraining effector activation. Single-cell V(D)J analysis revealed multiclonal, patient-unique adaptive repertoires, emphasizing the primacy of signaling context over receptor convergence. These findings define autoimmune diabetes as an inflammatory–inhibitory set-point continuum, positioning the NF-κB/EGFR–JAK/STAT gradient and HLA-C–KIR axis as potential therapeutic targets to preserve residual β-cell function.
Authors
Ivan I. Golodnikov, Elizaveta S. Podshivalova, Vadim I. Chechekhin, Anatoliy V. Zubritskiy, Alina A. Matrosova, Nikita A. Sergeev, Margarita D. Samsonova, Yaroslav V. Dvoryanchikov, Tatiana V. Nikonova, Ekaterina V. Bondarenko, Marina Yu. Loguinova, Yulia A. Medvedeva, Dmitry N. Laptev, Rita I. Khusainova, Ildar R. Minniakhmetov, Marina V. Shestakova, Natalia G. Mokrysheva, Ivan I. Dedov
Abstract
Saturated fatty acids impose lipotoxic stress on pancreatic β-cells, leading to β-cell failure and diabetes. In this study, we investigate the critical role of organellar Ca2+ disturbance on defective autophagy and β-cell lipotoxicity. Palmitate, a saturated fatty acid, induced perilysosomal Ca2+ elevation, sustained mTORC1 activation on the lysosomal membrane, suppression of the lysosomal transient receptor potential mucolipin 1 (TRPML1) channel, and accumulation of undigested autophagosomes in β-cells. These Ca2+ aberrations with autophagy defects by palmitate were prevented by an mTORC1 inhibitor or a mitochondrial superoxide scavenger. To alleviate perilysosomal Ca2+ overload, strategies such as lowering extracellular Ca2+, employing voltage-gated Ca2+ channel blocker or ATP-sensitive K+ channel opener effectively abrogated mTORC1 activation and preserved autophagy. Furthermore, redirecting perilysosomal Ca2+ into the endoplasmic reticulum (ER) with an ER Ca2+ ATPase activator, restores TRPML1 activity, promotes autophagic flux, and improves survival of β-cells exposed to palmitate-induced lipotoxicity. Our findings suggest oxidative stress-Ca2+ overload-mTORC1 pathway involvement in TRPML1 suppression and defective autophagy during β-cell lipotoxicity. Restoring perilysosomal Ca2+ homeostasis emerges as a promising therapeutic strategy for metabolic diseases.
Authors
Ha Thu Nguyen, Luong Dai Ly, Thuy Thi Thanh Ngo, Soo Kyung Lee, Carlos Noriega Polo, Subo Lee, Taesic Lee, Seung-Kuy Cha, Xaviera Riani Yasasilka, Kae Won Cho, Myung-Shik Lee, Andreas Wiederkehr, Claes B. Wollheim, Kyu-Sang Park
Abstract
Reproductive disorders can result from a defective action of the neuropeptide gonadotropin-releasing hormone (GnRH), the master regulator of reproduction. We have previously shown that SELENOT, a newly-described thioredoxin-like selenoprotein highly expressed in endocrine and neuroendocrine cells, plays a role in hormone secretion and neuroprotection. However, whether SELENOT is involved in neuro-endocrine regulations in vivo is totally unknown. We found that SELENOT deficiency in the brain impaired sexual behavior, leading to a decline in fertility in both male and female mice. Biochemical and histological analyses of the gonadotrope axis of these mice revealed a higher expression of GnRH, which is associated with circulating luteinizing hormone (LH) excess, and elevated steroid hormones in males and a polycystic ovary syndrome (PCOS)-like phenotype in females. In addition, SELENOT deficiency impaired LH pulse secretion in both male and female mice. These alterations are reverted after administration of a GnRH antagonist. Together, our data demonstrate for the first time the role of a selenoprotein in the central control of sexual behavior and reproduction, and identify a new redox effector of GnRH neuron activity impacting both male and female reproductive function.
Authors
Ben Yamine Mallouki, Loubna Boukhzar, Ludovic Dumont, Azénor Abgrall, Marjorie Gras, Agathe Prieur, David Alexandre, David Godefroy, Yves Tillet, Luca Grumolato, Nathalie Rives, Fatiha Chigr, Youssef Anouar
Abstract
The present study aims to explore the role and possible underlying mechanisms of histone lactylation modifications in diabetes-associated cognitive impairment (DACD). In this study, behavioral tests, Hematoxylin & Eosin (HE) staining, and immunohistochemistry were used to evaluate cognitive function and the extent of cerebral tissue injury. We quantified the levels of lactic acid and Pan-lysine lactylation (Pan Kla) in the brains of type 2 diabetes mellitus (T2DM) mice and in high glucose–treated microglia. We also identified all Kla sites in isolated microglia. Gene Ontology (GO) enrichment analysis and Kyoto Encyclopedia of Genes and Genomes (KEGG) pathway analysis were subsequently conducted to identify the functions and pathways that were enriched at the differentially expressed modification sites. cleavage under targets and tagmentation (CUT&Tag) technology was used to identify candidate genes that are regulated by H3K18la. Small interfering RNA (siRNA) and H3K18R mutant sequences were used to knock down crucial components in key signaling pathways to assess the effects of histone lactylation on microglial polarization. We found that lactic acid levels were significantly greater in the brains of T2DM mice and high glucose-treated microglia than in those of their corresponding controls, which increased the level of Pan-Kla. We discovered that lactate can directly stimulate an increase in H3K18la. The global landscape of the lactylome reveals information about modification sites, indicating a correlation between the upregulation of H3K18la and protein lactylation and Toll-like receptor signaling. CUT&Tag demonstrated that enhanced H3K18la directly stimulates the nuclear factor kappa-B (NF-κB) signaling pathway by increasing binding to the promoter of Toll Like Receptor 4 (TLR4), thereby promoting M1 microglial polarization. The present study demonstrated that enhanced H3K18la directly stimulates TLR4 signaling to promote M1 microglial polarization, thereby facilitating DACD phenotypes. Targeting such loop may be a potential therapeutic approach for the treatment of DACD.
Authors
Ying Yang, Fei Chen, Lulu Song, Liping Yu, Jinping Zhang, Bo Zhang
No posts were found with this tag.