Review
Open Access |  10.1172/jci.insight.199693
10.1172/jci.insight.199693
New approaches to uncover COPD pathobiology and develop therapies
Yohannes Tesfaigzi,1 Ali Önder Yildirim,2,3,4 Francesca Polverino,5 Thomas M. Conlon,2 Venkataramana Sidhaye,6 Maor Sauler,7 S. Vamsee Raju,8 Renata Z. Jurkowska,9 Divay Chandra,10 Michael H. Cho,1,11 Edwin K. Silverman,11 Ramon C. Sun,12 Peter Castaldi,11 Purushothama Rao Tata,13 Kambez H. Benam,14 Linto Antony,8 Mareike Lehmann,2,15,16 Beata Kosmider,17 Karim Bahmed,17 Zerihun H. Negasi,1 Kamakshi Bankoti,1 Carter Swaby,4,18 Dave A. Lagowala,19 Yeşim Vural,4,10 Hasan Bayram,4,20,21 Rosa Faner,22 George Washko,1 Dinh Son Bui,23 Bartolome Celli,1 Roxana Maria Wasnick,2 and Enid Neptune6
1Division of Pulmonary and Critical Care Medicine, Department of Medicine, Mass General Brigham and Harvard Medical School, Boston, Massachusetts, USA.
2Institute of Lung Health and Immunity (LHI), Helmholtz Munich, Comprehensive Pneumology Center (CPC-M), Member of the German Center for Lung Research (DZL), Munich, Germany.
3Institute of Experimental Pneumology, LMU University Hospital, Ludwig-Maximilian’s University, Munich, Germany.
4Koc University Research Center for Translational Medicine (KUTTAM), Istanbul, Turkey.
5Pulmonary and Critical Care Medicine, Baylor College of Medicine, Houston, Texas, USA.
6Department of Medicine, Division of Pulmonary and Critical Care Medicine, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
7Division of Pulmonary, Critical Care, and Sleep Medicine, Yale School of Medicine, New Haven, Connecticut, USA.
8Department of Medicine, Division of Pulmonary, Allergy and Critical Care Medicine, The University of Alabama at Birmingham, Birmingham, Alabama, USA.
9Division of Biomedicine, School of Biosciences, Cardiff University, Cardiff, United Kingdom.
10Division of Pulmonary, Allergy, Sleep and Critical Care Medicine, Department of Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
11Channing Division of Network Medicine, Brigham and Women’s Hospital and Harvard Medical School, Boston, Massachusetts, USA.
12Department of Biochemistry and Molecular Biology, College of Medicine, University of Florida, Gainesville, Florida, USA.
13Departments of Cell Biology and Medicine, Duke University School of Medicine, Durham, North Carolina, USA.
14Department of Medicine, Bioengineering, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
15Lung Aging and Regeneration, Institute for Lung Health (ILH), Giessen, Germany.
16Institute for Lung Research, Philipps-University Marburg, Universities of Giessen and Marburg Lung Center, German Center for Lung Research (DZL), Marburg, Germany.
17Department of Microbiology, Immunology and Inflammation, Center for Inflammation and Lung Research, Temple University, Philadelphia, Pennsylvania, USA.
18Department of Cell Biology, and
19Department of Environmental Health and Engineering, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
20Department of Cellular and Molecular Medicine, Graduate School of Health Sciences, and
21Department of Pulmonary Medicine, School of Medicine, Koc University, Istanbul, Turkey.
22Biomedicine Department, University of Barcelona, IDIBAPS, CIBER, Barcelona, Spain.
23Center for Epidemiology and Biostatistics, University of Melbourne, Melbourne, Victoria, Australia.
Address correspondence to: Yohannes Tesfaigzi, Pulmonary and Critical Care Medicine, Harvard Medical School, 75 Francis St, Boston, Massachusetts 02115, USA. Email: ytesfaigzi@bwh.harvard.edu.
Find articles by
Tesfaigzi, Y.
in:
PubMed
|
Google Scholar
|

1Division of Pulmonary and Critical Care Medicine, Department of Medicine, Mass General Brigham and Harvard Medical School, Boston, Massachusetts, USA.
2Institute of Lung Health and Immunity (LHI), Helmholtz Munich, Comprehensive Pneumology Center (CPC-M), Member of the German Center for Lung Research (DZL), Munich, Germany.
3Institute of Experimental Pneumology, LMU University Hospital, Ludwig-Maximilian’s University, Munich, Germany.
4Koc University Research Center for Translational Medicine (KUTTAM), Istanbul, Turkey.
5Pulmonary and Critical Care Medicine, Baylor College of Medicine, Houston, Texas, USA.
6Department of Medicine, Division of Pulmonary and Critical Care Medicine, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
7Division of Pulmonary, Critical Care, and Sleep Medicine, Yale School of Medicine, New Haven, Connecticut, USA.
8Department of Medicine, Division of Pulmonary, Allergy and Critical Care Medicine, The University of Alabama at Birmingham, Birmingham, Alabama, USA.
9Division of Biomedicine, School of Biosciences, Cardiff University, Cardiff, United Kingdom.
10Division of Pulmonary, Allergy, Sleep and Critical Care Medicine, Department of Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
11Channing Division of Network Medicine, Brigham and Women’s Hospital and Harvard Medical School, Boston, Massachusetts, USA.
12Department of Biochemistry and Molecular Biology, College of Medicine, University of Florida, Gainesville, Florida, USA.
13Departments of Cell Biology and Medicine, Duke University School of Medicine, Durham, North Carolina, USA.
14Department of Medicine, Bioengineering, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
15Lung Aging and Regeneration, Institute for Lung Health (ILH), Giessen, Germany.
16Institute for Lung Research, Philipps-University Marburg, Universities of Giessen and Marburg Lung Center, German Center for Lung Research (DZL), Marburg, Germany.
17Department of Microbiology, Immunology and Inflammation, Center for Inflammation and Lung Research, Temple University, Philadelphia, Pennsylvania, USA.
18Department of Cell Biology, and
19Department of Environmental Health and Engineering, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
20Department of Cellular and Molecular Medicine, Graduate School of Health Sciences, and
21Department of Pulmonary Medicine, School of Medicine, Koc University, Istanbul, Turkey.
22Biomedicine Department, University of Barcelona, IDIBAPS, CIBER, Barcelona, Spain.
23Center for Epidemiology and Biostatistics, University of Melbourne, Melbourne, Victoria, Australia.
Address correspondence to: Yohannes Tesfaigzi, Pulmonary and Critical Care Medicine, Harvard Medical School, 75 Francis St, Boston, Massachusetts 02115, USA. Email: ytesfaigzi@bwh.harvard.edu.
Find articles by Yildirim, A. in: PubMed | Google Scholar
1Division of Pulmonary and Critical Care Medicine, Department of Medicine, Mass General Brigham and Harvard Medical School, Boston, Massachusetts, USA.
2Institute of Lung Health and Immunity (LHI), Helmholtz Munich, Comprehensive Pneumology Center (CPC-M), Member of the German Center for Lung Research (DZL), Munich, Germany.
3Institute of Experimental Pneumology, LMU University Hospital, Ludwig-Maximilian’s University, Munich, Germany.
4Koc University Research Center for Translational Medicine (KUTTAM), Istanbul, Turkey.
5Pulmonary and Critical Care Medicine, Baylor College of Medicine, Houston, Texas, USA.
6Department of Medicine, Division of Pulmonary and Critical Care Medicine, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
7Division of Pulmonary, Critical Care, and Sleep Medicine, Yale School of Medicine, New Haven, Connecticut, USA.
8Department of Medicine, Division of Pulmonary, Allergy and Critical Care Medicine, The University of Alabama at Birmingham, Birmingham, Alabama, USA.
9Division of Biomedicine, School of Biosciences, Cardiff University, Cardiff, United Kingdom.
10Division of Pulmonary, Allergy, Sleep and Critical Care Medicine, Department of Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
11Channing Division of Network Medicine, Brigham and Women’s Hospital and Harvard Medical School, Boston, Massachusetts, USA.
12Department of Biochemistry and Molecular Biology, College of Medicine, University of Florida, Gainesville, Florida, USA.
13Departments of Cell Biology and Medicine, Duke University School of Medicine, Durham, North Carolina, USA.
14Department of Medicine, Bioengineering, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
15Lung Aging and Regeneration, Institute for Lung Health (ILH), Giessen, Germany.
16Institute for Lung Research, Philipps-University Marburg, Universities of Giessen and Marburg Lung Center, German Center for Lung Research (DZL), Marburg, Germany.
17Department of Microbiology, Immunology and Inflammation, Center for Inflammation and Lung Research, Temple University, Philadelphia, Pennsylvania, USA.
18Department of Cell Biology, and
19Department of Environmental Health and Engineering, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
20Department of Cellular and Molecular Medicine, Graduate School of Health Sciences, and
21Department of Pulmonary Medicine, School of Medicine, Koc University, Istanbul, Turkey.
22Biomedicine Department, University of Barcelona, IDIBAPS, CIBER, Barcelona, Spain.
23Center for Epidemiology and Biostatistics, University of Melbourne, Melbourne, Victoria, Australia.
Address correspondence to: Yohannes Tesfaigzi, Pulmonary and Critical Care Medicine, Harvard Medical School, 75 Francis St, Boston, Massachusetts 02115, USA. Email: ytesfaigzi@bwh.harvard.edu.
Find articles by
Polverino, F.
in:
PubMed
|
Google Scholar
|

1Division of Pulmonary and Critical Care Medicine, Department of Medicine, Mass General Brigham and Harvard Medical School, Boston, Massachusetts, USA.
2Institute of Lung Health and Immunity (LHI), Helmholtz Munich, Comprehensive Pneumology Center (CPC-M), Member of the German Center for Lung Research (DZL), Munich, Germany.
3Institute of Experimental Pneumology, LMU University Hospital, Ludwig-Maximilian’s University, Munich, Germany.
4Koc University Research Center for Translational Medicine (KUTTAM), Istanbul, Turkey.
5Pulmonary and Critical Care Medicine, Baylor College of Medicine, Houston, Texas, USA.
6Department of Medicine, Division of Pulmonary and Critical Care Medicine, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
7Division of Pulmonary, Critical Care, and Sleep Medicine, Yale School of Medicine, New Haven, Connecticut, USA.
8Department of Medicine, Division of Pulmonary, Allergy and Critical Care Medicine, The University of Alabama at Birmingham, Birmingham, Alabama, USA.
9Division of Biomedicine, School of Biosciences, Cardiff University, Cardiff, United Kingdom.
10Division of Pulmonary, Allergy, Sleep and Critical Care Medicine, Department of Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
11Channing Division of Network Medicine, Brigham and Women’s Hospital and Harvard Medical School, Boston, Massachusetts, USA.
12Department of Biochemistry and Molecular Biology, College of Medicine, University of Florida, Gainesville, Florida, USA.
13Departments of Cell Biology and Medicine, Duke University School of Medicine, Durham, North Carolina, USA.
14Department of Medicine, Bioengineering, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
15Lung Aging and Regeneration, Institute for Lung Health (ILH), Giessen, Germany.
16Institute for Lung Research, Philipps-University Marburg, Universities of Giessen and Marburg Lung Center, German Center for Lung Research (DZL), Marburg, Germany.
17Department of Microbiology, Immunology and Inflammation, Center for Inflammation and Lung Research, Temple University, Philadelphia, Pennsylvania, USA.
18Department of Cell Biology, and
19Department of Environmental Health and Engineering, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
20Department of Cellular and Molecular Medicine, Graduate School of Health Sciences, and
21Department of Pulmonary Medicine, School of Medicine, Koc University, Istanbul, Turkey.
22Biomedicine Department, University of Barcelona, IDIBAPS, CIBER, Barcelona, Spain.
23Center for Epidemiology and Biostatistics, University of Melbourne, Melbourne, Victoria, Australia.
Address correspondence to: Yohannes Tesfaigzi, Pulmonary and Critical Care Medicine, Harvard Medical School, 75 Francis St, Boston, Massachusetts 02115, USA. Email: ytesfaigzi@bwh.harvard.edu.
Find articles by
Conlon, T.
in:
PubMed
|
Google Scholar
|

1Division of Pulmonary and Critical Care Medicine, Department of Medicine, Mass General Brigham and Harvard Medical School, Boston, Massachusetts, USA.
2Institute of Lung Health and Immunity (LHI), Helmholtz Munich, Comprehensive Pneumology Center (CPC-M), Member of the German Center for Lung Research (DZL), Munich, Germany.
3Institute of Experimental Pneumology, LMU University Hospital, Ludwig-Maximilian’s University, Munich, Germany.
4Koc University Research Center for Translational Medicine (KUTTAM), Istanbul, Turkey.
5Pulmonary and Critical Care Medicine, Baylor College of Medicine, Houston, Texas, USA.
6Department of Medicine, Division of Pulmonary and Critical Care Medicine, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
7Division of Pulmonary, Critical Care, and Sleep Medicine, Yale School of Medicine, New Haven, Connecticut, USA.
8Department of Medicine, Division of Pulmonary, Allergy and Critical Care Medicine, The University of Alabama at Birmingham, Birmingham, Alabama, USA.
9Division of Biomedicine, School of Biosciences, Cardiff University, Cardiff, United Kingdom.
10Division of Pulmonary, Allergy, Sleep and Critical Care Medicine, Department of Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
11Channing Division of Network Medicine, Brigham and Women’s Hospital and Harvard Medical School, Boston, Massachusetts, USA.
12Department of Biochemistry and Molecular Biology, College of Medicine, University of Florida, Gainesville, Florida, USA.
13Departments of Cell Biology and Medicine, Duke University School of Medicine, Durham, North Carolina, USA.
14Department of Medicine, Bioengineering, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
15Lung Aging and Regeneration, Institute for Lung Health (ILH), Giessen, Germany.
16Institute for Lung Research, Philipps-University Marburg, Universities of Giessen and Marburg Lung Center, German Center for Lung Research (DZL), Marburg, Germany.
17Department of Microbiology, Immunology and Inflammation, Center for Inflammation and Lung Research, Temple University, Philadelphia, Pennsylvania, USA.
18Department of Cell Biology, and
19Department of Environmental Health and Engineering, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
20Department of Cellular and Molecular Medicine, Graduate School of Health Sciences, and
21Department of Pulmonary Medicine, School of Medicine, Koc University, Istanbul, Turkey.
22Biomedicine Department, University of Barcelona, IDIBAPS, CIBER, Barcelona, Spain.
23Center for Epidemiology and Biostatistics, University of Melbourne, Melbourne, Victoria, Australia.
Address correspondence to: Yohannes Tesfaigzi, Pulmonary and Critical Care Medicine, Harvard Medical School, 75 Francis St, Boston, Massachusetts 02115, USA. Email: ytesfaigzi@bwh.harvard.edu.
Find articles by Sidhaye, V. in: PubMed | Google Scholar
1Division of Pulmonary and Critical Care Medicine, Department of Medicine, Mass General Brigham and Harvard Medical School, Boston, Massachusetts, USA.
2Institute of Lung Health and Immunity (LHI), Helmholtz Munich, Comprehensive Pneumology Center (CPC-M), Member of the German Center for Lung Research (DZL), Munich, Germany.
3Institute of Experimental Pneumology, LMU University Hospital, Ludwig-Maximilian’s University, Munich, Germany.
4Koc University Research Center for Translational Medicine (KUTTAM), Istanbul, Turkey.
5Pulmonary and Critical Care Medicine, Baylor College of Medicine, Houston, Texas, USA.
6Department of Medicine, Division of Pulmonary and Critical Care Medicine, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
7Division of Pulmonary, Critical Care, and Sleep Medicine, Yale School of Medicine, New Haven, Connecticut, USA.
8Department of Medicine, Division of Pulmonary, Allergy and Critical Care Medicine, The University of Alabama at Birmingham, Birmingham, Alabama, USA.
9Division of Biomedicine, School of Biosciences, Cardiff University, Cardiff, United Kingdom.
10Division of Pulmonary, Allergy, Sleep and Critical Care Medicine, Department of Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
11Channing Division of Network Medicine, Brigham and Women’s Hospital and Harvard Medical School, Boston, Massachusetts, USA.
12Department of Biochemistry and Molecular Biology, College of Medicine, University of Florida, Gainesville, Florida, USA.
13Departments of Cell Biology and Medicine, Duke University School of Medicine, Durham, North Carolina, USA.
14Department of Medicine, Bioengineering, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
15Lung Aging and Regeneration, Institute for Lung Health (ILH), Giessen, Germany.
16Institute for Lung Research, Philipps-University Marburg, Universities of Giessen and Marburg Lung Center, German Center for Lung Research (DZL), Marburg, Germany.
17Department of Microbiology, Immunology and Inflammation, Center for Inflammation and Lung Research, Temple University, Philadelphia, Pennsylvania, USA.
18Department of Cell Biology, and
19Department of Environmental Health and Engineering, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
20Department of Cellular and Molecular Medicine, Graduate School of Health Sciences, and
21Department of Pulmonary Medicine, School of Medicine, Koc University, Istanbul, Turkey.
22Biomedicine Department, University of Barcelona, IDIBAPS, CIBER, Barcelona, Spain.
23Center for Epidemiology and Biostatistics, University of Melbourne, Melbourne, Victoria, Australia.
Address correspondence to: Yohannes Tesfaigzi, Pulmonary and Critical Care Medicine, Harvard Medical School, 75 Francis St, Boston, Massachusetts 02115, USA. Email: ytesfaigzi@bwh.harvard.edu.
Find articles by
Sauler, M.
in:
PubMed
|
Google Scholar
|

1Division of Pulmonary and Critical Care Medicine, Department of Medicine, Mass General Brigham and Harvard Medical School, Boston, Massachusetts, USA.
2Institute of Lung Health and Immunity (LHI), Helmholtz Munich, Comprehensive Pneumology Center (CPC-M), Member of the German Center for Lung Research (DZL), Munich, Germany.
3Institute of Experimental Pneumology, LMU University Hospital, Ludwig-Maximilian’s University, Munich, Germany.
4Koc University Research Center for Translational Medicine (KUTTAM), Istanbul, Turkey.
5Pulmonary and Critical Care Medicine, Baylor College of Medicine, Houston, Texas, USA.
6Department of Medicine, Division of Pulmonary and Critical Care Medicine, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
7Division of Pulmonary, Critical Care, and Sleep Medicine, Yale School of Medicine, New Haven, Connecticut, USA.
8Department of Medicine, Division of Pulmonary, Allergy and Critical Care Medicine, The University of Alabama at Birmingham, Birmingham, Alabama, USA.
9Division of Biomedicine, School of Biosciences, Cardiff University, Cardiff, United Kingdom.
10Division of Pulmonary, Allergy, Sleep and Critical Care Medicine, Department of Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
11Channing Division of Network Medicine, Brigham and Women’s Hospital and Harvard Medical School, Boston, Massachusetts, USA.
12Department of Biochemistry and Molecular Biology, College of Medicine, University of Florida, Gainesville, Florida, USA.
13Departments of Cell Biology and Medicine, Duke University School of Medicine, Durham, North Carolina, USA.
14Department of Medicine, Bioengineering, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
15Lung Aging and Regeneration, Institute for Lung Health (ILH), Giessen, Germany.
16Institute for Lung Research, Philipps-University Marburg, Universities of Giessen and Marburg Lung Center, German Center for Lung Research (DZL), Marburg, Germany.
17Department of Microbiology, Immunology and Inflammation, Center for Inflammation and Lung Research, Temple University, Philadelphia, Pennsylvania, USA.
18Department of Cell Biology, and
19Department of Environmental Health and Engineering, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
20Department of Cellular and Molecular Medicine, Graduate School of Health Sciences, and
21Department of Pulmonary Medicine, School of Medicine, Koc University, Istanbul, Turkey.
22Biomedicine Department, University of Barcelona, IDIBAPS, CIBER, Barcelona, Spain.
23Center for Epidemiology and Biostatistics, University of Melbourne, Melbourne, Victoria, Australia.
Address correspondence to: Yohannes Tesfaigzi, Pulmonary and Critical Care Medicine, Harvard Medical School, 75 Francis St, Boston, Massachusetts 02115, USA. Email: ytesfaigzi@bwh.harvard.edu.
Find articles by
Raju, S.
in:
PubMed
|
Google Scholar
|

1Division of Pulmonary and Critical Care Medicine, Department of Medicine, Mass General Brigham and Harvard Medical School, Boston, Massachusetts, USA.
2Institute of Lung Health and Immunity (LHI), Helmholtz Munich, Comprehensive Pneumology Center (CPC-M), Member of the German Center for Lung Research (DZL), Munich, Germany.
3Institute of Experimental Pneumology, LMU University Hospital, Ludwig-Maximilian’s University, Munich, Germany.
4Koc University Research Center for Translational Medicine (KUTTAM), Istanbul, Turkey.
5Pulmonary and Critical Care Medicine, Baylor College of Medicine, Houston, Texas, USA.
6Department of Medicine, Division of Pulmonary and Critical Care Medicine, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
7Division of Pulmonary, Critical Care, and Sleep Medicine, Yale School of Medicine, New Haven, Connecticut, USA.
8Department of Medicine, Division of Pulmonary, Allergy and Critical Care Medicine, The University of Alabama at Birmingham, Birmingham, Alabama, USA.
9Division of Biomedicine, School of Biosciences, Cardiff University, Cardiff, United Kingdom.
10Division of Pulmonary, Allergy, Sleep and Critical Care Medicine, Department of Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
11Channing Division of Network Medicine, Brigham and Women’s Hospital and Harvard Medical School, Boston, Massachusetts, USA.
12Department of Biochemistry and Molecular Biology, College of Medicine, University of Florida, Gainesville, Florida, USA.
13Departments of Cell Biology and Medicine, Duke University School of Medicine, Durham, North Carolina, USA.
14Department of Medicine, Bioengineering, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
15Lung Aging and Regeneration, Institute for Lung Health (ILH), Giessen, Germany.
16Institute for Lung Research, Philipps-University Marburg, Universities of Giessen and Marburg Lung Center, German Center for Lung Research (DZL), Marburg, Germany.
17Department of Microbiology, Immunology and Inflammation, Center for Inflammation and Lung Research, Temple University, Philadelphia, Pennsylvania, USA.
18Department of Cell Biology, and
19Department of Environmental Health and Engineering, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
20Department of Cellular and Molecular Medicine, Graduate School of Health Sciences, and
21Department of Pulmonary Medicine, School of Medicine, Koc University, Istanbul, Turkey.
22Biomedicine Department, University of Barcelona, IDIBAPS, CIBER, Barcelona, Spain.
23Center for Epidemiology and Biostatistics, University of Melbourne, Melbourne, Victoria, Australia.
Address correspondence to: Yohannes Tesfaigzi, Pulmonary and Critical Care Medicine, Harvard Medical School, 75 Francis St, Boston, Massachusetts 02115, USA. Email: ytesfaigzi@bwh.harvard.edu.
Find articles by
Jurkowska, R.
in:
PubMed
|
Google Scholar
|

1Division of Pulmonary and Critical Care Medicine, Department of Medicine, Mass General Brigham and Harvard Medical School, Boston, Massachusetts, USA.
2Institute of Lung Health and Immunity (LHI), Helmholtz Munich, Comprehensive Pneumology Center (CPC-M), Member of the German Center for Lung Research (DZL), Munich, Germany.
3Institute of Experimental Pneumology, LMU University Hospital, Ludwig-Maximilian’s University, Munich, Germany.
4Koc University Research Center for Translational Medicine (KUTTAM), Istanbul, Turkey.
5Pulmonary and Critical Care Medicine, Baylor College of Medicine, Houston, Texas, USA.
6Department of Medicine, Division of Pulmonary and Critical Care Medicine, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
7Division of Pulmonary, Critical Care, and Sleep Medicine, Yale School of Medicine, New Haven, Connecticut, USA.
8Department of Medicine, Division of Pulmonary, Allergy and Critical Care Medicine, The University of Alabama at Birmingham, Birmingham, Alabama, USA.
9Division of Biomedicine, School of Biosciences, Cardiff University, Cardiff, United Kingdom.
10Division of Pulmonary, Allergy, Sleep and Critical Care Medicine, Department of Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
11Channing Division of Network Medicine, Brigham and Women’s Hospital and Harvard Medical School, Boston, Massachusetts, USA.
12Department of Biochemistry and Molecular Biology, College of Medicine, University of Florida, Gainesville, Florida, USA.
13Departments of Cell Biology and Medicine, Duke University School of Medicine, Durham, North Carolina, USA.
14Department of Medicine, Bioengineering, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
15Lung Aging and Regeneration, Institute for Lung Health (ILH), Giessen, Germany.
16Institute for Lung Research, Philipps-University Marburg, Universities of Giessen and Marburg Lung Center, German Center for Lung Research (DZL), Marburg, Germany.
17Department of Microbiology, Immunology and Inflammation, Center for Inflammation and Lung Research, Temple University, Philadelphia, Pennsylvania, USA.
18Department of Cell Biology, and
19Department of Environmental Health and Engineering, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
20Department of Cellular and Molecular Medicine, Graduate School of Health Sciences, and
21Department of Pulmonary Medicine, School of Medicine, Koc University, Istanbul, Turkey.
22Biomedicine Department, University of Barcelona, IDIBAPS, CIBER, Barcelona, Spain.
23Center for Epidemiology and Biostatistics, University of Melbourne, Melbourne, Victoria, Australia.
Address correspondence to: Yohannes Tesfaigzi, Pulmonary and Critical Care Medicine, Harvard Medical School, 75 Francis St, Boston, Massachusetts 02115, USA. Email: ytesfaigzi@bwh.harvard.edu.
Find articles by Chandra, D. in: PubMed | Google Scholar
1Division of Pulmonary and Critical Care Medicine, Department of Medicine, Mass General Brigham and Harvard Medical School, Boston, Massachusetts, USA.
2Institute of Lung Health and Immunity (LHI), Helmholtz Munich, Comprehensive Pneumology Center (CPC-M), Member of the German Center for Lung Research (DZL), Munich, Germany.
3Institute of Experimental Pneumology, LMU University Hospital, Ludwig-Maximilian’s University, Munich, Germany.
4Koc University Research Center for Translational Medicine (KUTTAM), Istanbul, Turkey.
5Pulmonary and Critical Care Medicine, Baylor College of Medicine, Houston, Texas, USA.
6Department of Medicine, Division of Pulmonary and Critical Care Medicine, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
7Division of Pulmonary, Critical Care, and Sleep Medicine, Yale School of Medicine, New Haven, Connecticut, USA.
8Department of Medicine, Division of Pulmonary, Allergy and Critical Care Medicine, The University of Alabama at Birmingham, Birmingham, Alabama, USA.
9Division of Biomedicine, School of Biosciences, Cardiff University, Cardiff, United Kingdom.
10Division of Pulmonary, Allergy, Sleep and Critical Care Medicine, Department of Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
11Channing Division of Network Medicine, Brigham and Women’s Hospital and Harvard Medical School, Boston, Massachusetts, USA.
12Department of Biochemistry and Molecular Biology, College of Medicine, University of Florida, Gainesville, Florida, USA.
13Departments of Cell Biology and Medicine, Duke University School of Medicine, Durham, North Carolina, USA.
14Department of Medicine, Bioengineering, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
15Lung Aging and Regeneration, Institute for Lung Health (ILH), Giessen, Germany.
16Institute for Lung Research, Philipps-University Marburg, Universities of Giessen and Marburg Lung Center, German Center for Lung Research (DZL), Marburg, Germany.
17Department of Microbiology, Immunology and Inflammation, Center for Inflammation and Lung Research, Temple University, Philadelphia, Pennsylvania, USA.
18Department of Cell Biology, and
19Department of Environmental Health and Engineering, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
20Department of Cellular and Molecular Medicine, Graduate School of Health Sciences, and
21Department of Pulmonary Medicine, School of Medicine, Koc University, Istanbul, Turkey.
22Biomedicine Department, University of Barcelona, IDIBAPS, CIBER, Barcelona, Spain.
23Center for Epidemiology and Biostatistics, University of Melbourne, Melbourne, Victoria, Australia.
Address correspondence to: Yohannes Tesfaigzi, Pulmonary and Critical Care Medicine, Harvard Medical School, 75 Francis St, Boston, Massachusetts 02115, USA. Email: ytesfaigzi@bwh.harvard.edu.
Find articles by Cho, M. in: PubMed | Google Scholar
1Division of Pulmonary and Critical Care Medicine, Department of Medicine, Mass General Brigham and Harvard Medical School, Boston, Massachusetts, USA.
2Institute of Lung Health and Immunity (LHI), Helmholtz Munich, Comprehensive Pneumology Center (CPC-M), Member of the German Center for Lung Research (DZL), Munich, Germany.
3Institute of Experimental Pneumology, LMU University Hospital, Ludwig-Maximilian’s University, Munich, Germany.
4Koc University Research Center for Translational Medicine (KUTTAM), Istanbul, Turkey.
5Pulmonary and Critical Care Medicine, Baylor College of Medicine, Houston, Texas, USA.
6Department of Medicine, Division of Pulmonary and Critical Care Medicine, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
7Division of Pulmonary, Critical Care, and Sleep Medicine, Yale School of Medicine, New Haven, Connecticut, USA.
8Department of Medicine, Division of Pulmonary, Allergy and Critical Care Medicine, The University of Alabama at Birmingham, Birmingham, Alabama, USA.
9Division of Biomedicine, School of Biosciences, Cardiff University, Cardiff, United Kingdom.
10Division of Pulmonary, Allergy, Sleep and Critical Care Medicine, Department of Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
11Channing Division of Network Medicine, Brigham and Women’s Hospital and Harvard Medical School, Boston, Massachusetts, USA.
12Department of Biochemistry and Molecular Biology, College of Medicine, University of Florida, Gainesville, Florida, USA.
13Departments of Cell Biology and Medicine, Duke University School of Medicine, Durham, North Carolina, USA.
14Department of Medicine, Bioengineering, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
15Lung Aging and Regeneration, Institute for Lung Health (ILH), Giessen, Germany.
16Institute for Lung Research, Philipps-University Marburg, Universities of Giessen and Marburg Lung Center, German Center for Lung Research (DZL), Marburg, Germany.
17Department of Microbiology, Immunology and Inflammation, Center for Inflammation and Lung Research, Temple University, Philadelphia, Pennsylvania, USA.
18Department of Cell Biology, and
19Department of Environmental Health and Engineering, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
20Department of Cellular and Molecular Medicine, Graduate School of Health Sciences, and
21Department of Pulmonary Medicine, School of Medicine, Koc University, Istanbul, Turkey.
22Biomedicine Department, University of Barcelona, IDIBAPS, CIBER, Barcelona, Spain.
23Center for Epidemiology and Biostatistics, University of Melbourne, Melbourne, Victoria, Australia.
Address correspondence to: Yohannes Tesfaigzi, Pulmonary and Critical Care Medicine, Harvard Medical School, 75 Francis St, Boston, Massachusetts 02115, USA. Email: ytesfaigzi@bwh.harvard.edu.
Find articles by Silverman, E. in: PubMed | Google Scholar
1Division of Pulmonary and Critical Care Medicine, Department of Medicine, Mass General Brigham and Harvard Medical School, Boston, Massachusetts, USA.
2Institute of Lung Health and Immunity (LHI), Helmholtz Munich, Comprehensive Pneumology Center (CPC-M), Member of the German Center for Lung Research (DZL), Munich, Germany.
3Institute of Experimental Pneumology, LMU University Hospital, Ludwig-Maximilian’s University, Munich, Germany.
4Koc University Research Center for Translational Medicine (KUTTAM), Istanbul, Turkey.
5Pulmonary and Critical Care Medicine, Baylor College of Medicine, Houston, Texas, USA.
6Department of Medicine, Division of Pulmonary and Critical Care Medicine, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
7Division of Pulmonary, Critical Care, and Sleep Medicine, Yale School of Medicine, New Haven, Connecticut, USA.
8Department of Medicine, Division of Pulmonary, Allergy and Critical Care Medicine, The University of Alabama at Birmingham, Birmingham, Alabama, USA.
9Division of Biomedicine, School of Biosciences, Cardiff University, Cardiff, United Kingdom.
10Division of Pulmonary, Allergy, Sleep and Critical Care Medicine, Department of Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
11Channing Division of Network Medicine, Brigham and Women’s Hospital and Harvard Medical School, Boston, Massachusetts, USA.
12Department of Biochemistry and Molecular Biology, College of Medicine, University of Florida, Gainesville, Florida, USA.
13Departments of Cell Biology and Medicine, Duke University School of Medicine, Durham, North Carolina, USA.
14Department of Medicine, Bioengineering, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
15Lung Aging and Regeneration, Institute for Lung Health (ILH), Giessen, Germany.
16Institute for Lung Research, Philipps-University Marburg, Universities of Giessen and Marburg Lung Center, German Center for Lung Research (DZL), Marburg, Germany.
17Department of Microbiology, Immunology and Inflammation, Center for Inflammation and Lung Research, Temple University, Philadelphia, Pennsylvania, USA.
18Department of Cell Biology, and
19Department of Environmental Health and Engineering, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
20Department of Cellular and Molecular Medicine, Graduate School of Health Sciences, and
21Department of Pulmonary Medicine, School of Medicine, Koc University, Istanbul, Turkey.
22Biomedicine Department, University of Barcelona, IDIBAPS, CIBER, Barcelona, Spain.
23Center for Epidemiology and Biostatistics, University of Melbourne, Melbourne, Victoria, Australia.
Address correspondence to: Yohannes Tesfaigzi, Pulmonary and Critical Care Medicine, Harvard Medical School, 75 Francis St, Boston, Massachusetts 02115, USA. Email: ytesfaigzi@bwh.harvard.edu.
Find articles by Sun, R. in: PubMed | Google Scholar
1Division of Pulmonary and Critical Care Medicine, Department of Medicine, Mass General Brigham and Harvard Medical School, Boston, Massachusetts, USA.
2Institute of Lung Health and Immunity (LHI), Helmholtz Munich, Comprehensive Pneumology Center (CPC-M), Member of the German Center for Lung Research (DZL), Munich, Germany.
3Institute of Experimental Pneumology, LMU University Hospital, Ludwig-Maximilian’s University, Munich, Germany.
4Koc University Research Center for Translational Medicine (KUTTAM), Istanbul, Turkey.
5Pulmonary and Critical Care Medicine, Baylor College of Medicine, Houston, Texas, USA.
6Department of Medicine, Division of Pulmonary and Critical Care Medicine, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
7Division of Pulmonary, Critical Care, and Sleep Medicine, Yale School of Medicine, New Haven, Connecticut, USA.
8Department of Medicine, Division of Pulmonary, Allergy and Critical Care Medicine, The University of Alabama at Birmingham, Birmingham, Alabama, USA.
9Division of Biomedicine, School of Biosciences, Cardiff University, Cardiff, United Kingdom.
10Division of Pulmonary, Allergy, Sleep and Critical Care Medicine, Department of Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
11Channing Division of Network Medicine, Brigham and Women’s Hospital and Harvard Medical School, Boston, Massachusetts, USA.
12Department of Biochemistry and Molecular Biology, College of Medicine, University of Florida, Gainesville, Florida, USA.
13Departments of Cell Biology and Medicine, Duke University School of Medicine, Durham, North Carolina, USA.
14Department of Medicine, Bioengineering, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
15Lung Aging and Regeneration, Institute for Lung Health (ILH), Giessen, Germany.
16Institute for Lung Research, Philipps-University Marburg, Universities of Giessen and Marburg Lung Center, German Center for Lung Research (DZL), Marburg, Germany.
17Department of Microbiology, Immunology and Inflammation, Center for Inflammation and Lung Research, Temple University, Philadelphia, Pennsylvania, USA.
18Department of Cell Biology, and
19Department of Environmental Health and Engineering, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
20Department of Cellular and Molecular Medicine, Graduate School of Health Sciences, and
21Department of Pulmonary Medicine, School of Medicine, Koc University, Istanbul, Turkey.
22Biomedicine Department, University of Barcelona, IDIBAPS, CIBER, Barcelona, Spain.
23Center for Epidemiology and Biostatistics, University of Melbourne, Melbourne, Victoria, Australia.
Address correspondence to: Yohannes Tesfaigzi, Pulmonary and Critical Care Medicine, Harvard Medical School, 75 Francis St, Boston, Massachusetts 02115, USA. Email: ytesfaigzi@bwh.harvard.edu.
Find articles by Castaldi, P. in: PubMed | Google Scholar
1Division of Pulmonary and Critical Care Medicine, Department of Medicine, Mass General Brigham and Harvard Medical School, Boston, Massachusetts, USA.
2Institute of Lung Health and Immunity (LHI), Helmholtz Munich, Comprehensive Pneumology Center (CPC-M), Member of the German Center for Lung Research (DZL), Munich, Germany.
3Institute of Experimental Pneumology, LMU University Hospital, Ludwig-Maximilian’s University, Munich, Germany.
4Koc University Research Center for Translational Medicine (KUTTAM), Istanbul, Turkey.
5Pulmonary and Critical Care Medicine, Baylor College of Medicine, Houston, Texas, USA.
6Department of Medicine, Division of Pulmonary and Critical Care Medicine, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
7Division of Pulmonary, Critical Care, and Sleep Medicine, Yale School of Medicine, New Haven, Connecticut, USA.
8Department of Medicine, Division of Pulmonary, Allergy and Critical Care Medicine, The University of Alabama at Birmingham, Birmingham, Alabama, USA.
9Division of Biomedicine, School of Biosciences, Cardiff University, Cardiff, United Kingdom.
10Division of Pulmonary, Allergy, Sleep and Critical Care Medicine, Department of Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
11Channing Division of Network Medicine, Brigham and Women’s Hospital and Harvard Medical School, Boston, Massachusetts, USA.
12Department of Biochemistry and Molecular Biology, College of Medicine, University of Florida, Gainesville, Florida, USA.
13Departments of Cell Biology and Medicine, Duke University School of Medicine, Durham, North Carolina, USA.
14Department of Medicine, Bioengineering, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
15Lung Aging and Regeneration, Institute for Lung Health (ILH), Giessen, Germany.
16Institute for Lung Research, Philipps-University Marburg, Universities of Giessen and Marburg Lung Center, German Center for Lung Research (DZL), Marburg, Germany.
17Department of Microbiology, Immunology and Inflammation, Center for Inflammation and Lung Research, Temple University, Philadelphia, Pennsylvania, USA.
18Department of Cell Biology, and
19Department of Environmental Health and Engineering, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
20Department of Cellular and Molecular Medicine, Graduate School of Health Sciences, and
21Department of Pulmonary Medicine, School of Medicine, Koc University, Istanbul, Turkey.
22Biomedicine Department, University of Barcelona, IDIBAPS, CIBER, Barcelona, Spain.
23Center for Epidemiology and Biostatistics, University of Melbourne, Melbourne, Victoria, Australia.
Address correspondence to: Yohannes Tesfaigzi, Pulmonary and Critical Care Medicine, Harvard Medical School, 75 Francis St, Boston, Massachusetts 02115, USA. Email: ytesfaigzi@bwh.harvard.edu.
Find articles by Tata, P. in: PubMed | Google Scholar
1Division of Pulmonary and Critical Care Medicine, Department of Medicine, Mass General Brigham and Harvard Medical School, Boston, Massachusetts, USA.
2Institute of Lung Health and Immunity (LHI), Helmholtz Munich, Comprehensive Pneumology Center (CPC-M), Member of the German Center for Lung Research (DZL), Munich, Germany.
3Institute of Experimental Pneumology, LMU University Hospital, Ludwig-Maximilian’s University, Munich, Germany.
4Koc University Research Center for Translational Medicine (KUTTAM), Istanbul, Turkey.
5Pulmonary and Critical Care Medicine, Baylor College of Medicine, Houston, Texas, USA.
6Department of Medicine, Division of Pulmonary and Critical Care Medicine, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
7Division of Pulmonary, Critical Care, and Sleep Medicine, Yale School of Medicine, New Haven, Connecticut, USA.
8Department of Medicine, Division of Pulmonary, Allergy and Critical Care Medicine, The University of Alabama at Birmingham, Birmingham, Alabama, USA.
9Division of Biomedicine, School of Biosciences, Cardiff University, Cardiff, United Kingdom.
10Division of Pulmonary, Allergy, Sleep and Critical Care Medicine, Department of Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
11Channing Division of Network Medicine, Brigham and Women’s Hospital and Harvard Medical School, Boston, Massachusetts, USA.
12Department of Biochemistry and Molecular Biology, College of Medicine, University of Florida, Gainesville, Florida, USA.
13Departments of Cell Biology and Medicine, Duke University School of Medicine, Durham, North Carolina, USA.
14Department of Medicine, Bioengineering, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
15Lung Aging and Regeneration, Institute for Lung Health (ILH), Giessen, Germany.
16Institute for Lung Research, Philipps-University Marburg, Universities of Giessen and Marburg Lung Center, German Center for Lung Research (DZL), Marburg, Germany.
17Department of Microbiology, Immunology and Inflammation, Center for Inflammation and Lung Research, Temple University, Philadelphia, Pennsylvania, USA.
18Department of Cell Biology, and
19Department of Environmental Health and Engineering, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
20Department of Cellular and Molecular Medicine, Graduate School of Health Sciences, and
21Department of Pulmonary Medicine, School of Medicine, Koc University, Istanbul, Turkey.
22Biomedicine Department, University of Barcelona, IDIBAPS, CIBER, Barcelona, Spain.
23Center for Epidemiology and Biostatistics, University of Melbourne, Melbourne, Victoria, Australia.
Address correspondence to: Yohannes Tesfaigzi, Pulmonary and Critical Care Medicine, Harvard Medical School, 75 Francis St, Boston, Massachusetts 02115, USA. Email: ytesfaigzi@bwh.harvard.edu.
Find articles by
Benam, K.
in:
PubMed
|
Google Scholar
|

1Division of Pulmonary and Critical Care Medicine, Department of Medicine, Mass General Brigham and Harvard Medical School, Boston, Massachusetts, USA.
2Institute of Lung Health and Immunity (LHI), Helmholtz Munich, Comprehensive Pneumology Center (CPC-M), Member of the German Center for Lung Research (DZL), Munich, Germany.
3Institute of Experimental Pneumology, LMU University Hospital, Ludwig-Maximilian’s University, Munich, Germany.
4Koc University Research Center for Translational Medicine (KUTTAM), Istanbul, Turkey.
5Pulmonary and Critical Care Medicine, Baylor College of Medicine, Houston, Texas, USA.
6Department of Medicine, Division of Pulmonary and Critical Care Medicine, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
7Division of Pulmonary, Critical Care, and Sleep Medicine, Yale School of Medicine, New Haven, Connecticut, USA.
8Department of Medicine, Division of Pulmonary, Allergy and Critical Care Medicine, The University of Alabama at Birmingham, Birmingham, Alabama, USA.
9Division of Biomedicine, School of Biosciences, Cardiff University, Cardiff, United Kingdom.
10Division of Pulmonary, Allergy, Sleep and Critical Care Medicine, Department of Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
11Channing Division of Network Medicine, Brigham and Women’s Hospital and Harvard Medical School, Boston, Massachusetts, USA.
12Department of Biochemistry and Molecular Biology, College of Medicine, University of Florida, Gainesville, Florida, USA.
13Departments of Cell Biology and Medicine, Duke University School of Medicine, Durham, North Carolina, USA.
14Department of Medicine, Bioengineering, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
15Lung Aging and Regeneration, Institute for Lung Health (ILH), Giessen, Germany.
16Institute for Lung Research, Philipps-University Marburg, Universities of Giessen and Marburg Lung Center, German Center for Lung Research (DZL), Marburg, Germany.
17Department of Microbiology, Immunology and Inflammation, Center for Inflammation and Lung Research, Temple University, Philadelphia, Pennsylvania, USA.
18Department of Cell Biology, and
19Department of Environmental Health and Engineering, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
20Department of Cellular and Molecular Medicine, Graduate School of Health Sciences, and
21Department of Pulmonary Medicine, School of Medicine, Koc University, Istanbul, Turkey.
22Biomedicine Department, University of Barcelona, IDIBAPS, CIBER, Barcelona, Spain.
23Center for Epidemiology and Biostatistics, University of Melbourne, Melbourne, Victoria, Australia.
Address correspondence to: Yohannes Tesfaigzi, Pulmonary and Critical Care Medicine, Harvard Medical School, 75 Francis St, Boston, Massachusetts 02115, USA. Email: ytesfaigzi@bwh.harvard.edu.
Find articles by Antony, L. in: PubMed | Google Scholar
1Division of Pulmonary and Critical Care Medicine, Department of Medicine, Mass General Brigham and Harvard Medical School, Boston, Massachusetts, USA.
2Institute of Lung Health and Immunity (LHI), Helmholtz Munich, Comprehensive Pneumology Center (CPC-M), Member of the German Center for Lung Research (DZL), Munich, Germany.
3Institute of Experimental Pneumology, LMU University Hospital, Ludwig-Maximilian’s University, Munich, Germany.
4Koc University Research Center for Translational Medicine (KUTTAM), Istanbul, Turkey.
5Pulmonary and Critical Care Medicine, Baylor College of Medicine, Houston, Texas, USA.
6Department of Medicine, Division of Pulmonary and Critical Care Medicine, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
7Division of Pulmonary, Critical Care, and Sleep Medicine, Yale School of Medicine, New Haven, Connecticut, USA.
8Department of Medicine, Division of Pulmonary, Allergy and Critical Care Medicine, The University of Alabama at Birmingham, Birmingham, Alabama, USA.
9Division of Biomedicine, School of Biosciences, Cardiff University, Cardiff, United Kingdom.
10Division of Pulmonary, Allergy, Sleep and Critical Care Medicine, Department of Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
11Channing Division of Network Medicine, Brigham and Women’s Hospital and Harvard Medical School, Boston, Massachusetts, USA.
12Department of Biochemistry and Molecular Biology, College of Medicine, University of Florida, Gainesville, Florida, USA.
13Departments of Cell Biology and Medicine, Duke University School of Medicine, Durham, North Carolina, USA.
14Department of Medicine, Bioengineering, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
15Lung Aging and Regeneration, Institute for Lung Health (ILH), Giessen, Germany.
16Institute for Lung Research, Philipps-University Marburg, Universities of Giessen and Marburg Lung Center, German Center for Lung Research (DZL), Marburg, Germany.
17Department of Microbiology, Immunology and Inflammation, Center for Inflammation and Lung Research, Temple University, Philadelphia, Pennsylvania, USA.
18Department of Cell Biology, and
19Department of Environmental Health and Engineering, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
20Department of Cellular and Molecular Medicine, Graduate School of Health Sciences, and
21Department of Pulmonary Medicine, School of Medicine, Koc University, Istanbul, Turkey.
22Biomedicine Department, University of Barcelona, IDIBAPS, CIBER, Barcelona, Spain.
23Center for Epidemiology and Biostatistics, University of Melbourne, Melbourne, Victoria, Australia.
Address correspondence to: Yohannes Tesfaigzi, Pulmonary and Critical Care Medicine, Harvard Medical School, 75 Francis St, Boston, Massachusetts 02115, USA. Email: ytesfaigzi@bwh.harvard.edu.
Find articles by Lehmann, M. in: PubMed | Google Scholar
1Division of Pulmonary and Critical Care Medicine, Department of Medicine, Mass General Brigham and Harvard Medical School, Boston, Massachusetts, USA.
2Institute of Lung Health and Immunity (LHI), Helmholtz Munich, Comprehensive Pneumology Center (CPC-M), Member of the German Center for Lung Research (DZL), Munich, Germany.
3Institute of Experimental Pneumology, LMU University Hospital, Ludwig-Maximilian’s University, Munich, Germany.
4Koc University Research Center for Translational Medicine (KUTTAM), Istanbul, Turkey.
5Pulmonary and Critical Care Medicine, Baylor College of Medicine, Houston, Texas, USA.
6Department of Medicine, Division of Pulmonary and Critical Care Medicine, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
7Division of Pulmonary, Critical Care, and Sleep Medicine, Yale School of Medicine, New Haven, Connecticut, USA.
8Department of Medicine, Division of Pulmonary, Allergy and Critical Care Medicine, The University of Alabama at Birmingham, Birmingham, Alabama, USA.
9Division of Biomedicine, School of Biosciences, Cardiff University, Cardiff, United Kingdom.
10Division of Pulmonary, Allergy, Sleep and Critical Care Medicine, Department of Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
11Channing Division of Network Medicine, Brigham and Women’s Hospital and Harvard Medical School, Boston, Massachusetts, USA.
12Department of Biochemistry and Molecular Biology, College of Medicine, University of Florida, Gainesville, Florida, USA.
13Departments of Cell Biology and Medicine, Duke University School of Medicine, Durham, North Carolina, USA.
14Department of Medicine, Bioengineering, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
15Lung Aging and Regeneration, Institute for Lung Health (ILH), Giessen, Germany.
16Institute for Lung Research, Philipps-University Marburg, Universities of Giessen and Marburg Lung Center, German Center for Lung Research (DZL), Marburg, Germany.
17Department of Microbiology, Immunology and Inflammation, Center for Inflammation and Lung Research, Temple University, Philadelphia, Pennsylvania, USA.
18Department of Cell Biology, and
19Department of Environmental Health and Engineering, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
20Department of Cellular and Molecular Medicine, Graduate School of Health Sciences, and
21Department of Pulmonary Medicine, School of Medicine, Koc University, Istanbul, Turkey.
22Biomedicine Department, University of Barcelona, IDIBAPS, CIBER, Barcelona, Spain.
23Center for Epidemiology and Biostatistics, University of Melbourne, Melbourne, Victoria, Australia.
Address correspondence to: Yohannes Tesfaigzi, Pulmonary and Critical Care Medicine, Harvard Medical School, 75 Francis St, Boston, Massachusetts 02115, USA. Email: ytesfaigzi@bwh.harvard.edu.
Find articles by Kosmider, B. in: PubMed | Google Scholar
1Division of Pulmonary and Critical Care Medicine, Department of Medicine, Mass General Brigham and Harvard Medical School, Boston, Massachusetts, USA.
2Institute of Lung Health and Immunity (LHI), Helmholtz Munich, Comprehensive Pneumology Center (CPC-M), Member of the German Center for Lung Research (DZL), Munich, Germany.
3Institute of Experimental Pneumology, LMU University Hospital, Ludwig-Maximilian’s University, Munich, Germany.
4Koc University Research Center for Translational Medicine (KUTTAM), Istanbul, Turkey.
5Pulmonary and Critical Care Medicine, Baylor College of Medicine, Houston, Texas, USA.
6Department of Medicine, Division of Pulmonary and Critical Care Medicine, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
7Division of Pulmonary, Critical Care, and Sleep Medicine, Yale School of Medicine, New Haven, Connecticut, USA.
8Department of Medicine, Division of Pulmonary, Allergy and Critical Care Medicine, The University of Alabama at Birmingham, Birmingham, Alabama, USA.
9Division of Biomedicine, School of Biosciences, Cardiff University, Cardiff, United Kingdom.
10Division of Pulmonary, Allergy, Sleep and Critical Care Medicine, Department of Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
11Channing Division of Network Medicine, Brigham and Women’s Hospital and Harvard Medical School, Boston, Massachusetts, USA.
12Department of Biochemistry and Molecular Biology, College of Medicine, University of Florida, Gainesville, Florida, USA.
13Departments of Cell Biology and Medicine, Duke University School of Medicine, Durham, North Carolina, USA.
14Department of Medicine, Bioengineering, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
15Lung Aging and Regeneration, Institute for Lung Health (ILH), Giessen, Germany.
16Institute for Lung Research, Philipps-University Marburg, Universities of Giessen and Marburg Lung Center, German Center for Lung Research (DZL), Marburg, Germany.
17Department of Microbiology, Immunology and Inflammation, Center for Inflammation and Lung Research, Temple University, Philadelphia, Pennsylvania, USA.
18Department of Cell Biology, and
19Department of Environmental Health and Engineering, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
20Department of Cellular and Molecular Medicine, Graduate School of Health Sciences, and
21Department of Pulmonary Medicine, School of Medicine, Koc University, Istanbul, Turkey.
22Biomedicine Department, University of Barcelona, IDIBAPS, CIBER, Barcelona, Spain.
23Center for Epidemiology and Biostatistics, University of Melbourne, Melbourne, Victoria, Australia.
Address correspondence to: Yohannes Tesfaigzi, Pulmonary and Critical Care Medicine, Harvard Medical School, 75 Francis St, Boston, Massachusetts 02115, USA. Email: ytesfaigzi@bwh.harvard.edu.
Find articles by Bahmed, K. in: PubMed | Google Scholar
1Division of Pulmonary and Critical Care Medicine, Department of Medicine, Mass General Brigham and Harvard Medical School, Boston, Massachusetts, USA.
2Institute of Lung Health and Immunity (LHI), Helmholtz Munich, Comprehensive Pneumology Center (CPC-M), Member of the German Center for Lung Research (DZL), Munich, Germany.
3Institute of Experimental Pneumology, LMU University Hospital, Ludwig-Maximilian’s University, Munich, Germany.
4Koc University Research Center for Translational Medicine (KUTTAM), Istanbul, Turkey.
5Pulmonary and Critical Care Medicine, Baylor College of Medicine, Houston, Texas, USA.
6Department of Medicine, Division of Pulmonary and Critical Care Medicine, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
7Division of Pulmonary, Critical Care, and Sleep Medicine, Yale School of Medicine, New Haven, Connecticut, USA.
8Department of Medicine, Division of Pulmonary, Allergy and Critical Care Medicine, The University of Alabama at Birmingham, Birmingham, Alabama, USA.
9Division of Biomedicine, School of Biosciences, Cardiff University, Cardiff, United Kingdom.
10Division of Pulmonary, Allergy, Sleep and Critical Care Medicine, Department of Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
11Channing Division of Network Medicine, Brigham and Women’s Hospital and Harvard Medical School, Boston, Massachusetts, USA.
12Department of Biochemistry and Molecular Biology, College of Medicine, University of Florida, Gainesville, Florida, USA.
13Departments of Cell Biology and Medicine, Duke University School of Medicine, Durham, North Carolina, USA.
14Department of Medicine, Bioengineering, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
15Lung Aging and Regeneration, Institute for Lung Health (ILH), Giessen, Germany.
16Institute for Lung Research, Philipps-University Marburg, Universities of Giessen and Marburg Lung Center, German Center for Lung Research (DZL), Marburg, Germany.
17Department of Microbiology, Immunology and Inflammation, Center for Inflammation and Lung Research, Temple University, Philadelphia, Pennsylvania, USA.
18Department of Cell Biology, and
19Department of Environmental Health and Engineering, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
20Department of Cellular and Molecular Medicine, Graduate School of Health Sciences, and
21Department of Pulmonary Medicine, School of Medicine, Koc University, Istanbul, Turkey.
22Biomedicine Department, University of Barcelona, IDIBAPS, CIBER, Barcelona, Spain.
23Center for Epidemiology and Biostatistics, University of Melbourne, Melbourne, Victoria, Australia.
Address correspondence to: Yohannes Tesfaigzi, Pulmonary and Critical Care Medicine, Harvard Medical School, 75 Francis St, Boston, Massachusetts 02115, USA. Email: ytesfaigzi@bwh.harvard.edu.
Find articles by Negasi, Z. in: PubMed | Google Scholar
1Division of Pulmonary and Critical Care Medicine, Department of Medicine, Mass General Brigham and Harvard Medical School, Boston, Massachusetts, USA.
2Institute of Lung Health and Immunity (LHI), Helmholtz Munich, Comprehensive Pneumology Center (CPC-M), Member of the German Center for Lung Research (DZL), Munich, Germany.
3Institute of Experimental Pneumology, LMU University Hospital, Ludwig-Maximilian’s University, Munich, Germany.
4Koc University Research Center for Translational Medicine (KUTTAM), Istanbul, Turkey.
5Pulmonary and Critical Care Medicine, Baylor College of Medicine, Houston, Texas, USA.
6Department of Medicine, Division of Pulmonary and Critical Care Medicine, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
7Division of Pulmonary, Critical Care, and Sleep Medicine, Yale School of Medicine, New Haven, Connecticut, USA.
8Department of Medicine, Division of Pulmonary, Allergy and Critical Care Medicine, The University of Alabama at Birmingham, Birmingham, Alabama, USA.
9Division of Biomedicine, School of Biosciences, Cardiff University, Cardiff, United Kingdom.
10Division of Pulmonary, Allergy, Sleep and Critical Care Medicine, Department of Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
11Channing Division of Network Medicine, Brigham and Women’s Hospital and Harvard Medical School, Boston, Massachusetts, USA.
12Department of Biochemistry and Molecular Biology, College of Medicine, University of Florida, Gainesville, Florida, USA.
13Departments of Cell Biology and Medicine, Duke University School of Medicine, Durham, North Carolina, USA.
14Department of Medicine, Bioengineering, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
15Lung Aging and Regeneration, Institute for Lung Health (ILH), Giessen, Germany.
16Institute for Lung Research, Philipps-University Marburg, Universities of Giessen and Marburg Lung Center, German Center for Lung Research (DZL), Marburg, Germany.
17Department of Microbiology, Immunology and Inflammation, Center for Inflammation and Lung Research, Temple University, Philadelphia, Pennsylvania, USA.
18Department of Cell Biology, and
19Department of Environmental Health and Engineering, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
20Department of Cellular and Molecular Medicine, Graduate School of Health Sciences, and
21Department of Pulmonary Medicine, School of Medicine, Koc University, Istanbul, Turkey.
22Biomedicine Department, University of Barcelona, IDIBAPS, CIBER, Barcelona, Spain.
23Center for Epidemiology and Biostatistics, University of Melbourne, Melbourne, Victoria, Australia.
Address correspondence to: Yohannes Tesfaigzi, Pulmonary and Critical Care Medicine, Harvard Medical School, 75 Francis St, Boston, Massachusetts 02115, USA. Email: ytesfaigzi@bwh.harvard.edu.
Find articles by Bankoti, K. in: PubMed | Google Scholar
1Division of Pulmonary and Critical Care Medicine, Department of Medicine, Mass General Brigham and Harvard Medical School, Boston, Massachusetts, USA.
2Institute of Lung Health and Immunity (LHI), Helmholtz Munich, Comprehensive Pneumology Center (CPC-M), Member of the German Center for Lung Research (DZL), Munich, Germany.
3Institute of Experimental Pneumology, LMU University Hospital, Ludwig-Maximilian’s University, Munich, Germany.
4Koc University Research Center for Translational Medicine (KUTTAM), Istanbul, Turkey.
5Pulmonary and Critical Care Medicine, Baylor College of Medicine, Houston, Texas, USA.
6Department of Medicine, Division of Pulmonary and Critical Care Medicine, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
7Division of Pulmonary, Critical Care, and Sleep Medicine, Yale School of Medicine, New Haven, Connecticut, USA.
8Department of Medicine, Division of Pulmonary, Allergy and Critical Care Medicine, The University of Alabama at Birmingham, Birmingham, Alabama, USA.
9Division of Biomedicine, School of Biosciences, Cardiff University, Cardiff, United Kingdom.
10Division of Pulmonary, Allergy, Sleep and Critical Care Medicine, Department of Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
11Channing Division of Network Medicine, Brigham and Women’s Hospital and Harvard Medical School, Boston, Massachusetts, USA.
12Department of Biochemistry and Molecular Biology, College of Medicine, University of Florida, Gainesville, Florida, USA.
13Departments of Cell Biology and Medicine, Duke University School of Medicine, Durham, North Carolina, USA.
14Department of Medicine, Bioengineering, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
15Lung Aging and Regeneration, Institute for Lung Health (ILH), Giessen, Germany.
16Institute for Lung Research, Philipps-University Marburg, Universities of Giessen and Marburg Lung Center, German Center for Lung Research (DZL), Marburg, Germany.
17Department of Microbiology, Immunology and Inflammation, Center for Inflammation and Lung Research, Temple University, Philadelphia, Pennsylvania, USA.
18Department of Cell Biology, and
19Department of Environmental Health and Engineering, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
20Department of Cellular and Molecular Medicine, Graduate School of Health Sciences, and
21Department of Pulmonary Medicine, School of Medicine, Koc University, Istanbul, Turkey.
22Biomedicine Department, University of Barcelona, IDIBAPS, CIBER, Barcelona, Spain.
23Center for Epidemiology and Biostatistics, University of Melbourne, Melbourne, Victoria, Australia.
Address correspondence to: Yohannes Tesfaigzi, Pulmonary and Critical Care Medicine, Harvard Medical School, 75 Francis St, Boston, Massachusetts 02115, USA. Email: ytesfaigzi@bwh.harvard.edu.
Find articles by Swaby, C. in: PubMed | Google Scholar
1Division of Pulmonary and Critical Care Medicine, Department of Medicine, Mass General Brigham and Harvard Medical School, Boston, Massachusetts, USA.
2Institute of Lung Health and Immunity (LHI), Helmholtz Munich, Comprehensive Pneumology Center (CPC-M), Member of the German Center for Lung Research (DZL), Munich, Germany.
3Institute of Experimental Pneumology, LMU University Hospital, Ludwig-Maximilian’s University, Munich, Germany.
4Koc University Research Center for Translational Medicine (KUTTAM), Istanbul, Turkey.
5Pulmonary and Critical Care Medicine, Baylor College of Medicine, Houston, Texas, USA.
6Department of Medicine, Division of Pulmonary and Critical Care Medicine, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
7Division of Pulmonary, Critical Care, and Sleep Medicine, Yale School of Medicine, New Haven, Connecticut, USA.
8Department of Medicine, Division of Pulmonary, Allergy and Critical Care Medicine, The University of Alabama at Birmingham, Birmingham, Alabama, USA.
9Division of Biomedicine, School of Biosciences, Cardiff University, Cardiff, United Kingdom.
10Division of Pulmonary, Allergy, Sleep and Critical Care Medicine, Department of Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
11Channing Division of Network Medicine, Brigham and Women’s Hospital and Harvard Medical School, Boston, Massachusetts, USA.
12Department of Biochemistry and Molecular Biology, College of Medicine, University of Florida, Gainesville, Florida, USA.
13Departments of Cell Biology and Medicine, Duke University School of Medicine, Durham, North Carolina, USA.
14Department of Medicine, Bioengineering, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
15Lung Aging and Regeneration, Institute for Lung Health (ILH), Giessen, Germany.
16Institute for Lung Research, Philipps-University Marburg, Universities of Giessen and Marburg Lung Center, German Center for Lung Research (DZL), Marburg, Germany.
17Department of Microbiology, Immunology and Inflammation, Center for Inflammation and Lung Research, Temple University, Philadelphia, Pennsylvania, USA.
18Department of Cell Biology, and
19Department of Environmental Health and Engineering, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
20Department of Cellular and Molecular Medicine, Graduate School of Health Sciences, and
21Department of Pulmonary Medicine, School of Medicine, Koc University, Istanbul, Turkey.
22Biomedicine Department, University of Barcelona, IDIBAPS, CIBER, Barcelona, Spain.
23Center for Epidemiology and Biostatistics, University of Melbourne, Melbourne, Victoria, Australia.
Address correspondence to: Yohannes Tesfaigzi, Pulmonary and Critical Care Medicine, Harvard Medical School, 75 Francis St, Boston, Massachusetts 02115, USA. Email: ytesfaigzi@bwh.harvard.edu.
Find articles by Lagowala, D. in: PubMed | Google Scholar
1Division of Pulmonary and Critical Care Medicine, Department of Medicine, Mass General Brigham and Harvard Medical School, Boston, Massachusetts, USA.
2Institute of Lung Health and Immunity (LHI), Helmholtz Munich, Comprehensive Pneumology Center (CPC-M), Member of the German Center for Lung Research (DZL), Munich, Germany.
3Institute of Experimental Pneumology, LMU University Hospital, Ludwig-Maximilian’s University, Munich, Germany.
4Koc University Research Center for Translational Medicine (KUTTAM), Istanbul, Turkey.
5Pulmonary and Critical Care Medicine, Baylor College of Medicine, Houston, Texas, USA.
6Department of Medicine, Division of Pulmonary and Critical Care Medicine, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
7Division of Pulmonary, Critical Care, and Sleep Medicine, Yale School of Medicine, New Haven, Connecticut, USA.
8Department of Medicine, Division of Pulmonary, Allergy and Critical Care Medicine, The University of Alabama at Birmingham, Birmingham, Alabama, USA.
9Division of Biomedicine, School of Biosciences, Cardiff University, Cardiff, United Kingdom.
10Division of Pulmonary, Allergy, Sleep and Critical Care Medicine, Department of Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
11Channing Division of Network Medicine, Brigham and Women’s Hospital and Harvard Medical School, Boston, Massachusetts, USA.
12Department of Biochemistry and Molecular Biology, College of Medicine, University of Florida, Gainesville, Florida, USA.
13Departments of Cell Biology and Medicine, Duke University School of Medicine, Durham, North Carolina, USA.
14Department of Medicine, Bioengineering, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
15Lung Aging and Regeneration, Institute for Lung Health (ILH), Giessen, Germany.
16Institute for Lung Research, Philipps-University Marburg, Universities of Giessen and Marburg Lung Center, German Center for Lung Research (DZL), Marburg, Germany.
17Department of Microbiology, Immunology and Inflammation, Center for Inflammation and Lung Research, Temple University, Philadelphia, Pennsylvania, USA.
18Department of Cell Biology, and
19Department of Environmental Health and Engineering, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
20Department of Cellular and Molecular Medicine, Graduate School of Health Sciences, and
21Department of Pulmonary Medicine, School of Medicine, Koc University, Istanbul, Turkey.
22Biomedicine Department, University of Barcelona, IDIBAPS, CIBER, Barcelona, Spain.
23Center for Epidemiology and Biostatistics, University of Melbourne, Melbourne, Victoria, Australia.
Address correspondence to: Yohannes Tesfaigzi, Pulmonary and Critical Care Medicine, Harvard Medical School, 75 Francis St, Boston, Massachusetts 02115, USA. Email: ytesfaigzi@bwh.harvard.edu.
Find articles by Vural, Y. in: PubMed | Google Scholar
1Division of Pulmonary and Critical Care Medicine, Department of Medicine, Mass General Brigham and Harvard Medical School, Boston, Massachusetts, USA.
2Institute of Lung Health and Immunity (LHI), Helmholtz Munich, Comprehensive Pneumology Center (CPC-M), Member of the German Center for Lung Research (DZL), Munich, Germany.
3Institute of Experimental Pneumology, LMU University Hospital, Ludwig-Maximilian’s University, Munich, Germany.
4Koc University Research Center for Translational Medicine (KUTTAM), Istanbul, Turkey.
5Pulmonary and Critical Care Medicine, Baylor College of Medicine, Houston, Texas, USA.
6Department of Medicine, Division of Pulmonary and Critical Care Medicine, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
7Division of Pulmonary, Critical Care, and Sleep Medicine, Yale School of Medicine, New Haven, Connecticut, USA.
8Department of Medicine, Division of Pulmonary, Allergy and Critical Care Medicine, The University of Alabama at Birmingham, Birmingham, Alabama, USA.
9Division of Biomedicine, School of Biosciences, Cardiff University, Cardiff, United Kingdom.
10Division of Pulmonary, Allergy, Sleep and Critical Care Medicine, Department of Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
11Channing Division of Network Medicine, Brigham and Women’s Hospital and Harvard Medical School, Boston, Massachusetts, USA.
12Department of Biochemistry and Molecular Biology, College of Medicine, University of Florida, Gainesville, Florida, USA.
13Departments of Cell Biology and Medicine, Duke University School of Medicine, Durham, North Carolina, USA.
14Department of Medicine, Bioengineering, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
15Lung Aging and Regeneration, Institute for Lung Health (ILH), Giessen, Germany.
16Institute for Lung Research, Philipps-University Marburg, Universities of Giessen and Marburg Lung Center, German Center for Lung Research (DZL), Marburg, Germany.
17Department of Microbiology, Immunology and Inflammation, Center for Inflammation and Lung Research, Temple University, Philadelphia, Pennsylvania, USA.
18Department of Cell Biology, and
19Department of Environmental Health and Engineering, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
20Department of Cellular and Molecular Medicine, Graduate School of Health Sciences, and
21Department of Pulmonary Medicine, School of Medicine, Koc University, Istanbul, Turkey.
22Biomedicine Department, University of Barcelona, IDIBAPS, CIBER, Barcelona, Spain.
23Center for Epidemiology and Biostatistics, University of Melbourne, Melbourne, Victoria, Australia.
Address correspondence to: Yohannes Tesfaigzi, Pulmonary and Critical Care Medicine, Harvard Medical School, 75 Francis St, Boston, Massachusetts 02115, USA. Email: ytesfaigzi@bwh.harvard.edu.
Find articles by Bayram, H. in: PubMed | Google Scholar
1Division of Pulmonary and Critical Care Medicine, Department of Medicine, Mass General Brigham and Harvard Medical School, Boston, Massachusetts, USA.
2Institute of Lung Health and Immunity (LHI), Helmholtz Munich, Comprehensive Pneumology Center (CPC-M), Member of the German Center for Lung Research (DZL), Munich, Germany.
3Institute of Experimental Pneumology, LMU University Hospital, Ludwig-Maximilian’s University, Munich, Germany.
4Koc University Research Center for Translational Medicine (KUTTAM), Istanbul, Turkey.
5Pulmonary and Critical Care Medicine, Baylor College of Medicine, Houston, Texas, USA.
6Department of Medicine, Division of Pulmonary and Critical Care Medicine, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
7Division of Pulmonary, Critical Care, and Sleep Medicine, Yale School of Medicine, New Haven, Connecticut, USA.
8Department of Medicine, Division of Pulmonary, Allergy and Critical Care Medicine, The University of Alabama at Birmingham, Birmingham, Alabama, USA.
9Division of Biomedicine, School of Biosciences, Cardiff University, Cardiff, United Kingdom.
10Division of Pulmonary, Allergy, Sleep and Critical Care Medicine, Department of Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
11Channing Division of Network Medicine, Brigham and Women’s Hospital and Harvard Medical School, Boston, Massachusetts, USA.
12Department of Biochemistry and Molecular Biology, College of Medicine, University of Florida, Gainesville, Florida, USA.
13Departments of Cell Biology and Medicine, Duke University School of Medicine, Durham, North Carolina, USA.
14Department of Medicine, Bioengineering, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
15Lung Aging and Regeneration, Institute for Lung Health (ILH), Giessen, Germany.
16Institute for Lung Research, Philipps-University Marburg, Universities of Giessen and Marburg Lung Center, German Center for Lung Research (DZL), Marburg, Germany.
17Department of Microbiology, Immunology and Inflammation, Center for Inflammation and Lung Research, Temple University, Philadelphia, Pennsylvania, USA.
18Department of Cell Biology, and
19Department of Environmental Health and Engineering, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
20Department of Cellular and Molecular Medicine, Graduate School of Health Sciences, and
21Department of Pulmonary Medicine, School of Medicine, Koc University, Istanbul, Turkey.
22Biomedicine Department, University of Barcelona, IDIBAPS, CIBER, Barcelona, Spain.
23Center for Epidemiology and Biostatistics, University of Melbourne, Melbourne, Victoria, Australia.
Address correspondence to: Yohannes Tesfaigzi, Pulmonary and Critical Care Medicine, Harvard Medical School, 75 Francis St, Boston, Massachusetts 02115, USA. Email: ytesfaigzi@bwh.harvard.edu.
Find articles by Faner, R. in: PubMed | Google Scholar
1Division of Pulmonary and Critical Care Medicine, Department of Medicine, Mass General Brigham and Harvard Medical School, Boston, Massachusetts, USA.
2Institute of Lung Health and Immunity (LHI), Helmholtz Munich, Comprehensive Pneumology Center (CPC-M), Member of the German Center for Lung Research (DZL), Munich, Germany.
3Institute of Experimental Pneumology, LMU University Hospital, Ludwig-Maximilian’s University, Munich, Germany.
4Koc University Research Center for Translational Medicine (KUTTAM), Istanbul, Turkey.
5Pulmonary and Critical Care Medicine, Baylor College of Medicine, Houston, Texas, USA.
6Department of Medicine, Division of Pulmonary and Critical Care Medicine, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
7Division of Pulmonary, Critical Care, and Sleep Medicine, Yale School of Medicine, New Haven, Connecticut, USA.
8Department of Medicine, Division of Pulmonary, Allergy and Critical Care Medicine, The University of Alabama at Birmingham, Birmingham, Alabama, USA.
9Division of Biomedicine, School of Biosciences, Cardiff University, Cardiff, United Kingdom.
10Division of Pulmonary, Allergy, Sleep and Critical Care Medicine, Department of Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
11Channing Division of Network Medicine, Brigham and Women’s Hospital and Harvard Medical School, Boston, Massachusetts, USA.
12Department of Biochemistry and Molecular Biology, College of Medicine, University of Florida, Gainesville, Florida, USA.
13Departments of Cell Biology and Medicine, Duke University School of Medicine, Durham, North Carolina, USA.
14Department of Medicine, Bioengineering, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
15Lung Aging and Regeneration, Institute for Lung Health (ILH), Giessen, Germany.
16Institute for Lung Research, Philipps-University Marburg, Universities of Giessen and Marburg Lung Center, German Center for Lung Research (DZL), Marburg, Germany.
17Department of Microbiology, Immunology and Inflammation, Center for Inflammation and Lung Research, Temple University, Philadelphia, Pennsylvania, USA.
18Department of Cell Biology, and
19Department of Environmental Health and Engineering, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
20Department of Cellular and Molecular Medicine, Graduate School of Health Sciences, and
21Department of Pulmonary Medicine, School of Medicine, Koc University, Istanbul, Turkey.
22Biomedicine Department, University of Barcelona, IDIBAPS, CIBER, Barcelona, Spain.
23Center for Epidemiology and Biostatistics, University of Melbourne, Melbourne, Victoria, Australia.
Address correspondence to: Yohannes Tesfaigzi, Pulmonary and Critical Care Medicine, Harvard Medical School, 75 Francis St, Boston, Massachusetts 02115, USA. Email: ytesfaigzi@bwh.harvard.edu.
Find articles by Washko, G. in: PubMed | Google Scholar
1Division of Pulmonary and Critical Care Medicine, Department of Medicine, Mass General Brigham and Harvard Medical School, Boston, Massachusetts, USA.
2Institute of Lung Health and Immunity (LHI), Helmholtz Munich, Comprehensive Pneumology Center (CPC-M), Member of the German Center for Lung Research (DZL), Munich, Germany.
3Institute of Experimental Pneumology, LMU University Hospital, Ludwig-Maximilian’s University, Munich, Germany.
4Koc University Research Center for Translational Medicine (KUTTAM), Istanbul, Turkey.
5Pulmonary and Critical Care Medicine, Baylor College of Medicine, Houston, Texas, USA.
6Department of Medicine, Division of Pulmonary and Critical Care Medicine, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
7Division of Pulmonary, Critical Care, and Sleep Medicine, Yale School of Medicine, New Haven, Connecticut, USA.
8Department of Medicine, Division of Pulmonary, Allergy and Critical Care Medicine, The University of Alabama at Birmingham, Birmingham, Alabama, USA.
9Division of Biomedicine, School of Biosciences, Cardiff University, Cardiff, United Kingdom.
10Division of Pulmonary, Allergy, Sleep and Critical Care Medicine, Department of Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
11Channing Division of Network Medicine, Brigham and Women’s Hospital and Harvard Medical School, Boston, Massachusetts, USA.
12Department of Biochemistry and Molecular Biology, College of Medicine, University of Florida, Gainesville, Florida, USA.
13Departments of Cell Biology and Medicine, Duke University School of Medicine, Durham, North Carolina, USA.
14Department of Medicine, Bioengineering, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
15Lung Aging and Regeneration, Institute for Lung Health (ILH), Giessen, Germany.
16Institute for Lung Research, Philipps-University Marburg, Universities of Giessen and Marburg Lung Center, German Center for Lung Research (DZL), Marburg, Germany.
17Department of Microbiology, Immunology and Inflammation, Center for Inflammation and Lung Research, Temple University, Philadelphia, Pennsylvania, USA.
18Department of Cell Biology, and
19Department of Environmental Health and Engineering, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
20Department of Cellular and Molecular Medicine, Graduate School of Health Sciences, and
21Department of Pulmonary Medicine, School of Medicine, Koc University, Istanbul, Turkey.
22Biomedicine Department, University of Barcelona, IDIBAPS, CIBER, Barcelona, Spain.
23Center for Epidemiology and Biostatistics, University of Melbourne, Melbourne, Victoria, Australia.
Address correspondence to: Yohannes Tesfaigzi, Pulmonary and Critical Care Medicine, Harvard Medical School, 75 Francis St, Boston, Massachusetts 02115, USA. Email: ytesfaigzi@bwh.harvard.edu.
Find articles by Bui, D. in: PubMed | Google Scholar
1Division of Pulmonary and Critical Care Medicine, Department of Medicine, Mass General Brigham and Harvard Medical School, Boston, Massachusetts, USA.
2Institute of Lung Health and Immunity (LHI), Helmholtz Munich, Comprehensive Pneumology Center (CPC-M), Member of the German Center for Lung Research (DZL), Munich, Germany.
3Institute of Experimental Pneumology, LMU University Hospital, Ludwig-Maximilian’s University, Munich, Germany.
4Koc University Research Center for Translational Medicine (KUTTAM), Istanbul, Turkey.
5Pulmonary and Critical Care Medicine, Baylor College of Medicine, Houston, Texas, USA.
6Department of Medicine, Division of Pulmonary and Critical Care Medicine, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
7Division of Pulmonary, Critical Care, and Sleep Medicine, Yale School of Medicine, New Haven, Connecticut, USA.
8Department of Medicine, Division of Pulmonary, Allergy and Critical Care Medicine, The University of Alabama at Birmingham, Birmingham, Alabama, USA.
9Division of Biomedicine, School of Biosciences, Cardiff University, Cardiff, United Kingdom.
10Division of Pulmonary, Allergy, Sleep and Critical Care Medicine, Department of Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
11Channing Division of Network Medicine, Brigham and Women’s Hospital and Harvard Medical School, Boston, Massachusetts, USA.
12Department of Biochemistry and Molecular Biology, College of Medicine, University of Florida, Gainesville, Florida, USA.
13Departments of Cell Biology and Medicine, Duke University School of Medicine, Durham, North Carolina, USA.
14Department of Medicine, Bioengineering, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
15Lung Aging and Regeneration, Institute for Lung Health (ILH), Giessen, Germany.
16Institute for Lung Research, Philipps-University Marburg, Universities of Giessen and Marburg Lung Center, German Center for Lung Research (DZL), Marburg, Germany.
17Department of Microbiology, Immunology and Inflammation, Center for Inflammation and Lung Research, Temple University, Philadelphia, Pennsylvania, USA.
18Department of Cell Biology, and
19Department of Environmental Health and Engineering, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
20Department of Cellular and Molecular Medicine, Graduate School of Health Sciences, and
21Department of Pulmonary Medicine, School of Medicine, Koc University, Istanbul, Turkey.
22Biomedicine Department, University of Barcelona, IDIBAPS, CIBER, Barcelona, Spain.
23Center for Epidemiology and Biostatistics, University of Melbourne, Melbourne, Victoria, Australia.
Address correspondence to: Yohannes Tesfaigzi, Pulmonary and Critical Care Medicine, Harvard Medical School, 75 Francis St, Boston, Massachusetts 02115, USA. Email: ytesfaigzi@bwh.harvard.edu.
Find articles by Celli, B. in: PubMed | Google Scholar
1Division of Pulmonary and Critical Care Medicine, Department of Medicine, Mass General Brigham and Harvard Medical School, Boston, Massachusetts, USA.
2Institute of Lung Health and Immunity (LHI), Helmholtz Munich, Comprehensive Pneumology Center (CPC-M), Member of the German Center for Lung Research (DZL), Munich, Germany.
3Institute of Experimental Pneumology, LMU University Hospital, Ludwig-Maximilian’s University, Munich, Germany.
4Koc University Research Center for Translational Medicine (KUTTAM), Istanbul, Turkey.
5Pulmonary and Critical Care Medicine, Baylor College of Medicine, Houston, Texas, USA.
6Department of Medicine, Division of Pulmonary and Critical Care Medicine, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
7Division of Pulmonary, Critical Care, and Sleep Medicine, Yale School of Medicine, New Haven, Connecticut, USA.
8Department of Medicine, Division of Pulmonary, Allergy and Critical Care Medicine, The University of Alabama at Birmingham, Birmingham, Alabama, USA.
9Division of Biomedicine, School of Biosciences, Cardiff University, Cardiff, United Kingdom.
10Division of Pulmonary, Allergy, Sleep and Critical Care Medicine, Department of Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
11Channing Division of Network Medicine, Brigham and Women’s Hospital and Harvard Medical School, Boston, Massachusetts, USA.
12Department of Biochemistry and Molecular Biology, College of Medicine, University of Florida, Gainesville, Florida, USA.
13Departments of Cell Biology and Medicine, Duke University School of Medicine, Durham, North Carolina, USA.
14Department of Medicine, Bioengineering, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
15Lung Aging and Regeneration, Institute for Lung Health (ILH), Giessen, Germany.
16Institute for Lung Research, Philipps-University Marburg, Universities of Giessen and Marburg Lung Center, German Center for Lung Research (DZL), Marburg, Germany.
17Department of Microbiology, Immunology and Inflammation, Center for Inflammation and Lung Research, Temple University, Philadelphia, Pennsylvania, USA.
18Department of Cell Biology, and
19Department of Environmental Health and Engineering, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
20Department of Cellular and Molecular Medicine, Graduate School of Health Sciences, and
21Department of Pulmonary Medicine, School of Medicine, Koc University, Istanbul, Turkey.
22Biomedicine Department, University of Barcelona, IDIBAPS, CIBER, Barcelona, Spain.
23Center for Epidemiology and Biostatistics, University of Melbourne, Melbourne, Victoria, Australia.
Address correspondence to: Yohannes Tesfaigzi, Pulmonary and Critical Care Medicine, Harvard Medical School, 75 Francis St, Boston, Massachusetts 02115, USA. Email: ytesfaigzi@bwh.harvard.edu.
Find articles by Wasnick, R. in: PubMed | Google Scholar
1Division of Pulmonary and Critical Care Medicine, Department of Medicine, Mass General Brigham and Harvard Medical School, Boston, Massachusetts, USA.
2Institute of Lung Health and Immunity (LHI), Helmholtz Munich, Comprehensive Pneumology Center (CPC-M), Member of the German Center for Lung Research (DZL), Munich, Germany.
3Institute of Experimental Pneumology, LMU University Hospital, Ludwig-Maximilian’s University, Munich, Germany.
4Koc University Research Center for Translational Medicine (KUTTAM), Istanbul, Turkey.
5Pulmonary and Critical Care Medicine, Baylor College of Medicine, Houston, Texas, USA.
6Department of Medicine, Division of Pulmonary and Critical Care Medicine, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
7Division of Pulmonary, Critical Care, and Sleep Medicine, Yale School of Medicine, New Haven, Connecticut, USA.
8Department of Medicine, Division of Pulmonary, Allergy and Critical Care Medicine, The University of Alabama at Birmingham, Birmingham, Alabama, USA.
9Division of Biomedicine, School of Biosciences, Cardiff University, Cardiff, United Kingdom.
10Division of Pulmonary, Allergy, Sleep and Critical Care Medicine, Department of Medicine, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
11Channing Division of Network Medicine, Brigham and Women’s Hospital and Harvard Medical School, Boston, Massachusetts, USA.
12Department of Biochemistry and Molecular Biology, College of Medicine, University of Florida, Gainesville, Florida, USA.
13Departments of Cell Biology and Medicine, Duke University School of Medicine, Durham, North Carolina, USA.
14Department of Medicine, Bioengineering, University of Pittsburgh, Pittsburgh, Pennsylvania, USA.
15Lung Aging and Regeneration, Institute for Lung Health (ILH), Giessen, Germany.
16Institute for Lung Research, Philipps-University Marburg, Universities of Giessen and Marburg Lung Center, German Center for Lung Research (DZL), Marburg, Germany.
17Department of Microbiology, Immunology and Inflammation, Center for Inflammation and Lung Research, Temple University, Philadelphia, Pennsylvania, USA.
18Department of Cell Biology, and
19Department of Environmental Health and Engineering, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
20Department of Cellular and Molecular Medicine, Graduate School of Health Sciences, and
21Department of Pulmonary Medicine, School of Medicine, Koc University, Istanbul, Turkey.
22Biomedicine Department, University of Barcelona, IDIBAPS, CIBER, Barcelona, Spain.
23Center for Epidemiology and Biostatistics, University of Melbourne, Melbourne, Victoria, Australia.
Address correspondence to: Yohannes Tesfaigzi, Pulmonary and Critical Care Medicine, Harvard Medical School, 75 Francis St, Boston, Massachusetts 02115, USA. Email: ytesfaigzi@bwh.harvard.edu.
Find articles by Neptune, E. in: PubMed | Google Scholar
Published February 23, 2026 - More info
JCI Insight. 2026;11(4):e199693. https://doi.org/10.1172/jci.insight.199693.
© 2026 Tesfaigzi et al. This work is licensed under the Creative Commons Attribution 4.0 International License. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
-
Abstract
Chronic obstructive pulmonary disease (COPD) was the third leading cause of global mortality in 2011 but receives limited attention and research funding. This Review describes the current knowledge on COPD risk factors, including genetic and epigenetic determinants and their interactions with the microbiome and environmental exposures. Preclinical models are being refined and single-cell transcriptomic, metabolomic, and proteomic technologies are being implemented to investigate the molecular mechanisms of disease progression. Patient cohorts to define biomarkers of early disease and the latest approaches to diagnose pre-COPD are essential to accelerate the development of novel and effective therapeutic interventions and translate new findings into clinical trials. This Review is a summary of topics covered by a symposium organized by the COPD-iNET consortium, an international network of researchers who have established a platform that facilitates collaboration of this multidisciplinary group of preclinical, translational, and clinical researchers.
-
The worldwide burden of chronic obstructive pulmonary disease
Worldwide, chronic obstructive pulmonary disease (COPD) affects approximately 400–600 million people, significantly strains health care systems (1), and is the third leading cause of death (2–4). What is less emphasized is that the definition of COPD as a clinical disorder has evolved. Beyond tobacco exposure, the recognition of early life events, distinct permissive or directive immune responses to environmental triggers, and a staged evolution in the disorder reflects nuances delivered by the intensive clinical translational and basic research efforts pursued over the past 25 years. Despite the profound disease burden, compared with other less common lung diseases, COPD research has historically received limited attention and resources (5, 6).
What is achievable for COPD in 2026? Efficient, integrative, and respectful use of advanced in vitro and in vivo testing modalities informed by in silico datasets cohere into a standard of team science providing mechanistic validation for therapeutic targets. Candidate therapeutics are fueled by promising delivery systems and highly targeted agents, such as nanobodies, customized vectors, small molecules with defined spectra of activity, and repurposed pharmacologics capable of accelerated approval for use. Clinical trials can adopt the creativity of COVID-era studies that incorporate multiple agents, shorter time scales, and both surrogate and definitive readouts. The cures are ready for launch. This Review will focus on the current frontier of COPD investigations that have the potential to transform COPD research.
Why this, why now? In response to the great need to accelerate progress in COPD research, an international network of basic and translational researchers has formed the COPD-iNET consortium to facilitate knowledge exchange and form new research collaborations (7). The second annual COPD-iNET symposium brought together leading experts in the field to explore and discuss the latest findings, align research priorities, and integrate findings toward developing reliable diagnostics and treatments for COPD. The symposium, held in Boston, Massachusetts, was generously supported by the American Lung Association (ALA). Over 115 participants gathered in person to address five key COPD research areas (Figure 1) — genetics, environmental factors, model systems, drug development, and new technologies. The goal of COPD-iNET is to provide a platform that facilitates multidisciplinary research involving basic, translational, and clinical data to be harmonized for meta-analyses. This platform will accelerate the drug development pipeline and increase the success rate of efficacy in COPD subtypes. This Review summarizes key insights across these domains and outlines key challenges and future directions to study the molecular mechanisms and development of therapies for COPD. Certain areas of interest in COPD are beyond the scope of this Review and are best served by more intensive and detailed articles.
 Figure 1
Figure 1COPD-iNET symposium focused on five key areas critical to understanding the mechanistic underpinnings of COPD. Genetic and environmental factors drive each other to cause disease progression. Cohorts with early-stage COPD help unravel the complex interactions leading to disease. Advances in single-cell technologies offer detailed insights into cellular changes. At the same time, improved preclinical models support the development and screening of therapeutic candidates capable of interrupting the cycle of gene-and-environment interaction to halt COPD progression.
-
COPD definition and subtypes
In the late 1990s and early 2000s, COPD classification was significantly transformed due to efforts of the American Thoracic Society and the European Respiratory Society, who published the first guidelines aimed at improving COPD diagnosis, classification, and management (8). Next, the Global Initiative for Chronic Obstructive Lung Disease (GOLD) established worldwide recommendations to standardize COPD diagnosis and management (9). Together, with the classical 4 stages (stage 1–4) of spirometrically recognized airflow obstruction severity, GOLD introduced the concept of “GOLD stages,” with stage 0 defined as individuals experiencing chronic respiratory symptoms, but with normal spirometry. Abnormal spirometry is defined by a ratio of forced expiratory volume in one second to forced vital capacity (FEV1/FVC) of less than 0.7 and severity defined by reduced FEV1 (10) (Table 1).
Clinically, COPD is a progressive disorder characterized by largely irreversible airflow limitation. COPD encompasses two major histological variants: emphysema, characterized by alveolar destruction; and chronic bronchitis, defined by mucus hypersecretion, chronic inflammation, airway wall thickening, and alveolar remodeling, all of which reduce quality of life (11). Most patients have a combination of these manifestations, and disease heterogeneity creates a challenge to classify COPD into distinct subtypes. Recently dupilumab, an IL-4/IL-13 receptor–targeting mAb, reduced exacerbations and improved lung function (12) in patients with COPD who also had a high eosinophil count; however, this success is limited to a small percentage of patients. The advancement of disease-modifying therapies for COPD is still required, as the mortality rate remains high.
-
“Pre-COPD” as an entity and available cohorts
Observational studies of long-term smokers consistently show a constellation of respiratory symptomatology that precedes obstructive lung physiology (13). The “pre-COPD” concept emerged (14) for certain clinical respiratory symptoms and physiological and imaging abnormalities in a heterogeneous group of individuals at high risk of developing clinical overt COPD (15). Early and pre-COPD risk factors often overlap and are based on their strong links to early lung function decline and disease progression and highlights a growing recognition that COPD develops long before spirometric obstruction and clinical symptoms become apparent (16, 17).
Several methods are now established and used to define changes in the lung to detect pre-COPD. Oscillometry requires minimal patient cooperation, making it particularly well suited for pediatric use (18). Computerized CT scans identify structural abnormalities and CT remains one of the most potent tools in the early detection of pre-COPD (19). MRI offers a radiation-free approach that is exceptionally sensitive to soft-tissue changes. Hyperpolarized helium or xenon MRI can detect lung ventilation abnormalities, even when CT scans and spirometry appear normal (20). Analyses of electronic health records, imaging data, and wearable device data may allow continuous monitoring in real-time and help clinicians to predict which individuals at risk to progress to COPD (21–23) (Figure 2).
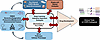 Figure 2
Figure 2Evolving landscape of COPD research. GWAS provide information on susceptibility genes and DNA methylation. ChIP-seq and ATAC-seq from appropriate tissues provide epigenetic modifications that are associated with environmental factors. Data from specific tissues and cell types generate QTL information that points to genes and reliable information on pathways involved in affecting cellular phenotypes and pathways that could be initiators of disease. This in turn can be used to develop appropriate preclinical COPD models that capture the gene-and-environment interaction. Applying deep learning algorithms to scRNA-seq and spatial RNA-seq data from preclinical and pre-COPD cohort samples, together with the GWAS and QTL data, can be used to understand COPD heterogeneity. An iterative process of data analysis and retesting in experimental models and findings from pre-COPD cohorts helps to prioritize for testing appropriate drugs that will be successful in clinical trials and have minimal side effects.
A landmark study analyzed lung function trajectories of individuals between ages 25 and 75 from three independent cohorts — the Framingham Offspring Cohort, the Copenhagen City Heart Study, and the Lovelace Smokers Cohort. While some individuals reached 100% predicted FEV1 in early adulthood, others only reached 75%, with both groups showing either stable or rapidly declining lung function (24). Those with low baseline lung function and rapid decline had a 35-fold higher risk of developing COPD within 18 months and a 2.5-fold higher mortality risk compared with those with higher lung function (16). In the CARDIA Lung Study, longitudinal lung function trajectories were linked to COPD development or pre-COPD (25). Preserved ratio impaired spirometry (PRISm) — defined as a reduced FEV1 with preserved FEV1/FVC ratio (26) — is prevalent (13% of the COPDGene cohort and 7.1% in the general population of adults >45 years of age) and associated with increased respiratory symptoms, systemic inflammation, and a cardiovascular mortality rate of 18.7% (27).
ALA launched the Lung Health Cohort, a new, population-based study focused on characterizing lung health in millennials (ages 25–35) without diagnosed severe respiratory disease (28). The Ghana randomized air pollution and health study (GRAPHS) enrolled 1,414 nonsmoking pregnant women and has followed their children for over eight years. Early findings show that high prenatal exposure to household air pollution is linked to impaired lung function in infancy and early childhood (29). The Tasmanian longitudinal health study (TAHS) identified three of six trajectories with increased COPD risk as measured at 7, 13, 18, 45, 50, and 53 years of age (30, 31).
The Subpopulations and Intermediate Outcome Measures in COPD Study (SPIROMICS) cohort showed that elevated MUC5AC, but not MUC5B, in sputum is a biomarker for pre-COPD. Genetic and proteomic studies continue to explore reliable biomarkers to identify pre-COPD (32–34). Inflammatory markers in blood (35), sputum (36), and exhaled breath condensate have shown promise for detecting early inflammatory changes prior to spirometric decline. Notably, lower circulating CC16 levels and higher MMP levels have been associated with early lung function impairment. In the COPDGene study, both low CC16 (37) and soluble RAGE (38) were linked to increased risk of disease progression and poor outcomes. In COPDGene, individuals with high polygenic risk score (PRS) were more likely to exhibit early airflow limitations, even in the absence of spirometrically defined COPD (39, 40).
-
COPD-associated risk factors
Infants born prematurely with underdeveloped lungs have an increased COPD risk. These infants may experience reduced lung growth, airway obstruction, and impaired lung function that persist into childhood and adulthood (30, 41, 42) (Figure 2). Furthermore, frequent or severe respiratory tract infections in childhood, including influenza, respiratory syncytial virus (RSV), and bacterial infections, that cause bronchitis, pneumonia, and recurrent wheezing episodes can cause lasting damage to developing airways and lungs, leading to changes that prevent normal lung growth and accelerate age-related lung function decline, especially when combined with other risk factors, such as smoking or other environmental exposures (30, 41, 42). Childhood asthma has also been linked to developing early COPD, as persistent airway inflammation and recurrent obstruction can lead to long-term lung damage, especially when combined with other risk factors (42, 43).
This Review will primarily focus on the most recent concepts in COPD-related genetic risk factors, epigenetics, and gene-environment interactions, as these topics have previously been well covered (44–46).
COPD susceptibility genes. The most widely described genetic factor contributing to COPD development, particularly emphysema, is α-1 antitrypsin deficiency (AATD), a hereditary condition first described in 1963 (47). AATD is usually caused by homozygosity at the SNP rs28929474 in serpin family A member 1 (SERPINA1), which encodes a missense variant of the AAT protein. Other loss-of-function alleles, including rare nonsense variants, can exist as homozygotes or complex heterozygotes and associate with COPD. AAT primarily functions to inactivate neutrophil elastase (48). The prevalence of severe AATD is estimated at 1%–2% of the population (49). As with other susceptibilities, smoking increases the risk of COPD in AATD, and this exacerbation is an early example of gene-by-environment interaction (50).
GWAS has successfully identified thousands of genetic risk loci for human traits and chronic diseases (51) by scanning the entire genome of many individuals to find genetic differences (typically SNPs) that correlate with a particular condition or phenotype. For COPD, GWAS has identified SNPs in or near HHIP, FAM13A, and MFAP2 (52–54), and numerous genome-wide loci associated with FEV1/FVC ratio and FEV1 have been identified (55, 56) (Figure 2).
While the contribution of genetic variants to COPD development is well established, functional validation remains challenging. First, many analyses have focused on cohorts of patients with late-stage COPD, a point by which it is unclear what effect a genetic variant had on disease initiation in the early stages and what is the result of secondary damage at later stages. Because patients at early COPD stages do not present with respiratory symptoms, it is difficult to obtain cells initially affected by the variant. Second, GWAS results alone usually do not provide definitive information on functional mechanisms. Third, determination of the genes affected by GWAS loci (target genes) can be challenging, as most of the causal variants are located in noncoding sections of genome (57) (intergenic or intragenic regions) (58), indicating that these loci may regulate gene expression via complex interactions with distal regulatory elements. A molecular understanding of causative SNPs has been challenging, because a single SNP or multiple SNPs can affect one or multiple cell types, and each can amplify the response to pollutants and the resulting cellular interactions in the lung (59).
The ability to combine multiple genetic variants into a PRS can generate a numerical value that reflects an individual’s predictive risk of developing COPD independent of clinical risk factors (40, 60). Although powerful, genetic predisposition alone is not enough; interactions between genes and environmental factors must be considered. Indeed, integrating information from inherited (genetic) and environmental (epigenetic) DNA and chromatin changes can point to key genes and pathways associated with COPD development and progression (Figure 2).
Additional -omics approaches can also be integrated with genetics to investigate the molecular heterogeneity in COPD. For example, integration of transcriptomics, DNA methylation, and miRNA profiles was recently used to identify disease endotypes associated with clinical COPD characteristics, such as FEV1 or blood eosinophils (61). When undertaking such approaches it is important to consider that unsupervised clustering across cohorts to identify COPD subtypes may show modest reproducibility (62): however, trajectory analyses are more promising, as they integrate additional factors such as longitudinal lung function (63).
A successful strategy to identify GWAS target genes is to combine GWAS and expression quantitative trait locus (eQTL) studies, which test the association between genetic variants and RNA levels of nearby genes (Figure 2). These combined analyses identify genomic regions where GWAS and eQTL association signals coincide, and colocalization methods apply statistical analyses that distinguish causal from chance or correlational (linkage disequilbrium) GWAS-eQTL overlap by estimating the probability that both signals are caused by the same functional variant(s). QTLs at single-cell resolution could provide insight into molecular mechanisms underlying the pathobiology of COPD by exploring the interface of altered gene expression and the resulting biological consequence (64).
Environmental factors. COPD-associated genetic factors likely interact with environmental factors, such as smoking, occupational exposures, and air pollution, to cause disease. However, research on the cellular pathways and mechanisms that link environmental factors to genetic variants to drive disease is in its infancy. It is of great importance to understand the mechanisms underlying environmental factors that drive COPD development to ultimately develop therapies. Studies on the effects of different types of particulate matter (PM) derived from air pollution, cigarette smoke (CS), wood smoke (WS), and gases, including ozone (O3) and nitrogen oxides on cellular systems is complex. In addition, how societal stress conditions and fitness interact with genetic and epigenetic susceptibility factors have not been explored (Figure 3).
 Figure 3
Figure 3Risk factors and pathomechanisms driving COPD development. Starting from the early stages of embryonic development throughout growth into adulthood, the lung is exposed to many risk factors. Many of these risk factors can affect individuals to different extents and in different combinations, as do the many pathomechanisms that comprise a wide range of cellular pathways. More importantly, these pathomechanisms are also affected by comorbidities that enhance disease progression.
PM is a category of inhalable particles classified by size rather than chemical composition. PM is a complex mixture from both natural sources, such as vegetation and dust, and combustion emissions from cooking or heating stoves, wildfires, and other human activities, including cigarette smoking and industrial emissions (65). Localization of these particles in lung tissue largely depends on size — particles larger than 10 μm (PM10) typically settle in the nose and throat, those between 2.5 and 10 μm (PM2.5–10) deposit in larger airways, particles less than 2.5 μm (PM2.5) reach lower airways, and nanoparticles (<0.1 micrometers, PM0.1) can be internalized into the alveoli (66). While in high-income countries, PM from CS is the primary cause for COPD, in both high- and low-income countries, PM from biomass smoke from cooking or heating stoves, dust storms, traffic, and wildfires contribute to the onset and progression of COPD (67, 68),
Long-term exposure to even low air pollutant levels can increase COPD incidence (69). The Framingham Heart Study showed a correlation between PM2.5 exposure and reduced lung function metrics like FEV1 and FVC (70). PM2.5 reduces FEV1, increases COPD risk (71), and caused lung function decline both in the Lovelace Smokers Cohort (72) and the SPIROMICS cohort (73). Additionally, a retrospective Korean cohort study found a significant association between long-term PM2.5 exposure and COPD development (66). Table 2 summarizes environmental factors, their main sources, and roles in COPD development. Gaseous pollutants, including nitrogen dioxide (NO2), O3, and sulfur dioxide (SO2), primarily originate from fossil fuel combustion.
Exposure of cells to pollution and the inflammatory milieu enhances oxidative damage, promoting cellular apoptosis, senescence, and destruction of alveolar walls. Airway remodeling is the persistent change in lung structures due to repeated epithelial damage, including goblet cell hyperplasia, which causes persistent and increased mucus production. Furthermore, inflammatory stressors can cause extensive changes to genomic structures, including epigenetic reprogramming of many lung cells, such as the airway epithelium, fibroblasts, and inflammatory cells. Importantly, small airway pathologies, such as narrowing of airways and thickening of airway walls due to smooth muscle hypertrophy and fibrosis, are thought to occur before the loss of alveolar tissue and lung function decline (74).
Populations from low- and high-income countries are exposed to biomass fuel smoke from open wood or dung fires, stoves to cook or heat homes, and from recent increased occurrences of wildfires (75, 76). While some wildfire pollutants are short-lived and disperse quickly from the fire site, PM can travel vast distances, far exceeding the size of the original fire area (77). Dust storms from the Middle East and Sahara Desert are associated with an increased hospitalization risk for patients with COPD (78).
Wildfires also have adverse effects on birth weight, respiratory, cardiovascular, and other diseases (79, 80). Systematic meta-analyses concluded that pollution from WS not only increases the risk for COPD exacerbations (81, 82) and pneumonia (83), but more than doubles the risk of COPD and chronic bronchitis (84–86), and increases emergency room visits, hospitalizations, and mortality (87–89). Coarse PM (PM2.5–10) extracted from the 2008 California wildfires rapidly induced cell death in murine macrophages in vitro, with significantly higher cytotoxicity than coarse PM collected from ambient air (90). Similar rapid cytotoxic effects on alveolar macrophages were observed using bronchoalveolar lavage in a murine model following intratracheal instillation of wildfire coarse PM (91).
Daily or occasional E-cigarette users have higher odds of developing COPD compared with non-users (92). A long-term cohort study of 10,326 Chinese adults reinforced this risk, with a significant correlation between E-cigarette use and respiratory symptoms or COPD, especially with concurrent combustible cigarette use (93). Waterpipe exposure elicits an inflammatory response similar to that of conventional smoking (94), and in vitro studies indicate that it causes epithelial barrier dysfunction and reduces lung cell proliferation, while increasing markers of cellular senescence (95, 96).
Combined effects of ambient air pollution on lung health. Population studies have demonstrated that PM2.5 from CS and WS have an additive effect on reducing lung function and risk for COPD (71), an effect that has also been validated in animal studies (97, 98). Therefore, stratifying PM2.5 into specific, relevant environmental exposures such as tobacco and wildfire smoke may be important to fully understand the effect of various sources of PM2.5.
-
Gene-by-environment interaction
Environmental exposures drive epigenetic changes. CS, PM, and biomass fuels have all been shown to induce profound epigenetic modifications (99, 100) that facilitate interactions between environmental factors and gene expression. DNA methylation and histone modifications modulate transcriptional activity without altering the underlying DNA sequence (101). Treatment with global demethylating agent 5-azacytidine mitigates CS-induced alveolar destruction in human precision-cut lung slices (PCLS) (102). Emerging evidence also suggests that DNA methylation may provide a sensitive biomarker for COPD detection and patient stratification (103, 104).
DNA methylation, which is catalyzed by DNA methyltransferases, is regulated by various establishment and maintenance enzymes (105). The ten-eleven translocation (TET) family of proteins facilitates DNA demethylation (106). Notably, TET1 and TET2 are reduced in response to CS and are low in COPD (107). In contrast, DNMT1, which maintains DNA methylation, and DNMT3a, responsible for de novo methylation (108), are elevated in lung tissues of patients with COPD, with DNMT3a showing a strong negative correlation with pulmonary function (109). While DNA methylation is primarily an epigenetic modification, the chemical structure of 5-methylcytosine (5mC) increases spontaneous deamination, leading to a CG-to-TG transition (110), often triggered by oxidative stress, a common consequence of environmental exposures. This suggests that even methylation can result in genetic changes (Figure 3).
Histone acetylation, catalyzed by histone acetyltransferases and removed by histone deacetylases, typically enhances DNA accessibility and promotes gene transcription. These proteins have been broadly linked to inflammation, corticosteroid resistance, and changes in epithelial barrier integrity and contribute to COPD (111, 112). Furthermore, histone methylation can alter chromatin accessibility and change gene activation. For instance, the histone methylation mark H3K4me3 is associated with open chromatin and active transcription, whereas H3K27me3 and H3K9me3 marks are associated with closed chromatin and inactive transcription (113, 114). These broad mechanisms may not adequately capture the complexity and variability within biological systems, highlighting the need for a more nuanced understanding of the factors influencing epigenetic responses. Several genome-wide studies, including recent high-resolution whole-genome bisulfite sequencing (WGBS) studies in purified lung cells support widespread DNA methylation changes in COPD (105).
Epigenetic profiling of chromatin accessibility, 3D interactions, DNA methylation, enhancer RNA, and specific histone modifications may help identify which variants affect gene expression in specific cell types. These approaches have potential to identify risk variants by providing functional annotation across the genome. Indeed, recent high-resolution data from purified lung cells indicate that DNA methylation changes in COPD cells often occur in regulatory regions, including enhancers (104). An additional potential mediator of genetic risk are short noncoding miRNAs (115, 116), which offer an exciting therapeutic potential due to their ability to transfer messages via extracellular vesicles (EVs) from cell to cell and propagate disease. Indeed, exciting data this year revealed that COPD airway epithelial cell–derived EVs enriched with miR-34a could spread cellular senescence to neighboring cells, potentially accounting for disease progression (117). The integration of genetic and epigenetic analyses may provide functional mechanisms linking genetic variants to chronicity of disease pathology.
Microbiome changes affected by environmental exposures. Environmental factors significantly influence the composition and diversity of the lung microbiome. Toxic exposures, including CS and air pollution, can disrupt the delicate balance of microbial communities in the pulmonary system, leading to dysbiosis. For instance, CS contains a wide array of harmful chemicals that can alter microbial populations and promote an inflammatory environment within the lungs (118).
Patients with moderate to severe COPD often show greater enrichment of oral bacteria in the lung (119), potentially due to swallowing difficulties and gastroesophageal reflux, which may allow oral bacteria to colonize the lower airways (120). Impaired mucociliary clearance in COPD can further contribute to microbiome dysbiosis (121). Additionally, dysbiosis in the oral cavity may impact airway health. A systematic review highlighted a correlation between periodontal disease and COPD, thus improving oral health may mitigate respiratory disease progression, especially in high-risk elderly patients (122).
-
Advances in preclinical COPD models
Effective drug development requires laboratory models that closely recapitulate the complexity of multifactorial etiology and patient heterogeneity to increase the likelihood for effective clinical translation (123). Table 3 highlights current and emerging preclinical models, including in vitro/ex vivo and animal models for COPD research and lists their strengths and weaknesses.
-
In vitro and ex vivo models
Air-liquid interface cultures allow basal cells to differentiate into a pseudostratified mucociliary epithelium (124). Organs-on-chip, also known as microphysiological systems (MPS), are biomimetic devices that incorporate living cells within perfusable microfluidic channels and/or chambers (125–128). These systems replicate key features of human organs by recreating multicellular architectures, tissue-tissue interfaces, biochemical gradients, mechanical forces, and dynamic vascular perfusion. Multiple human lung MPS have been developed to model distinct lung regions, including small airways, alveoli, parenchymal microvasculature, and stroma (125, 129, 130). These models reproduce hallmark features, including smoke-induced oxidative stress, inflammation, and epithelial barrier disruption, while also enabling the evaluation of therapeutics and precision medicine strategies (131).
PCLS provide a valuable ex vivo approach that preserves native tissue architecture and cellular diversity of the diseased lung. PCLS are typically prepared by filling lungs with agarose and cutting into thin (100–500 μm) slices, thus maintaining viable cells in their original spatial relationships, including epithelial-mesenchymal interactions and intact microvasculature (132–134). PCLS derived from patients with COPD or animal models facilitate direct translational comparisons, potentially improving predictive validity (135). This model permits detailed investigation of regional heterogeneity, a critical COPD aspect of not easily addressed in isolated cell cultures (136).
Lung organoids are 3D structures derived from stem/progenitor cells that self-organize to recapitulate aspects of lung development and architecture. Organoids bridge the gap between traditional cell culture systems and animal models, providing intermediate complexity with enhanced physiological relevance (137). Organoids have been successfully used to identify novel regenerative therapies in COPD (138). COPD-derived organoids revealed a role for dose-dependent hedgehog-mediated signaling in proximal-distal identity of fibroblast maintenance and the effect of its dysregulation on alveolar regeneration and emphysema (139). In particular, induced pluripotent stem cell–derived (iPSC-derived) organoids have been instrumental in modeling the effect of GWAS-identified COPD genes on modulating alveolar type 2 (AT2) pneumocyte cell function (140). Future studies need to expand tissue engineering approaches to reconstruct anatomical sites, like respiratory bronchiolar cells, that currently lack well-established genetic models (141).
In summary, in vitro and ex vivo enable detailed mechanistic studies under controlled conditions, providing high-throughput screening platforms and enhancing translation through direct investigation of human tissues.
-
Animal COPD models
Mice have dominated preclinical COPD research due to their well-characterized genetics, strain availability, lower maintenance costs, smaller size, and shorter lifespan. Genetic factors across murine species influence susceptibility to CS-induced emphysema. In a screen of 34 inbred mouse strains, A/J mice were most susceptible and CBA/J mice were least vulnerable due to an Abi3bp variant (142). Compared with male C57BL/6 mice, female animals are resistant to CS-induced emphysema, while these sex-specific differences are not observed in C3H mice (97). In contrast, CS-exposed female B6C3F1 mice develop emphysema (143, 144). Mice have notable limitations, including less robust airway pathology, limited airflow obstruction despite parenchymal changes, and immune response patterns that differ from humans (145). Rat inflammatory profiles more closely resemble human disease, particularly regarding neutrophil recruitment, protease expression, and pronounced small airway remodeling and enhanced mucous cell metaplasia (146, 147).
The major advantage of mouse models is the development of animals with gene-targeted deletion that avail investigation of specific genes and molecular pathways in COPD pathogenesis. For example, AATD models are relevant given the established clinical link between AATD and early-onset emphysema (148). Furthermore, transgenic models have been invaluable in validating genetic insights from large population-based approaches. CS-exposed, Fam13a-deficient mice are protected against emphysema compared with WT controls, providing direct functional validation of this GWAS-identified risk locus (149).
Ferrets, sheep, and nonhuman primates (NHPs) have been used to overcome anatomical and physiological limitations of rodent models. Viral or bacterial challenges of smoke-exposed ferrets produce exaggerated inflammatory responses, worsened lung function, and prolonged recovery periods characteristic of COPD exacerbations (150). NHPs share approximately 93%–99% genetic homology with humans and possess comparable lung anatomy (151). Long-term CS exposure in NHPs produces emphysematous changes, airway remodeling, and mucus hyperproduction that closely parallels human disease (152). NHP models are particularly valuable for investigating age-related COPD aspects and evaluating biologics, which often show species-specific immune responses (153).
Two-hit models. Acute infections exacerbate COPD progression and mortality. In mice, CS exposure combined with bacterial LPS administration amplifies inflammatory responses and accelerates pathological changes compared with smoke/elastase alone (154, 155). Similarly, smoke exposure combined with viral infection (influenza, RSV, or rhinovirus) mirrors the virus-triggered exacerbations common in patients with COPD (156, 157). These approaches demonstrate synergistic effects on disease manifestation, dramatically reducing the experimental duration (158). Furthermore, integration of genetic factors with environmental exposures, as shown by combining AATD with CS exposure, recapitulates accelerated emphysema development (159).
-
Pathomechanisms of COPD
Oxidative stress injury, resident cell senescence/death, and compromised wound repair are pivotal in COPD pathology and elicited by several mechanisms, including ROS production due to dysfunctional mitochondria, membrane-bound NADPH oxidases, and neutrophil-derived myeloperoxidase (MPO) (160). ROS also cause DNA damage, including bulky chemical adducts, methylated bases, oxidized purine and pyrimidine bases, abasic sites, and single- and double-strand breaks. Modifications of DNA bases that require base excision repair (BER) or nucleotide excision repair (NER) persist due to COPD-related defects in the genes responsible for these repair processes (161).
Pathological changes in COPD include compositional and quantitative changes in the ECM (162), collagen deposition, and reduced elastin (163). Regulatory proteins within the ECM, such as extracellular SOD3, are reduced in lungs of patients with COPD, causing remodeling of elastin, fibronectin, and collagen to increase airway resistance and reduce elastic recoil (162, 164). Furthermore, CS can increase MMP-12 activity in macrophages, disrupting the balance between proteolysis and antiproteolysis and inhibiting normal ECM repair (165–167).
Advances in single-cell technologies, particularly scRNA-seq, have dramatically expanded our understanding of COPD by identifying key cellular sources of pathobiology. These approaches offer unprecedented resolution of cell-type-specific transcriptional programs and state changes that underlie tissue remodeling, inflammation, and impaired regeneration. Critically, these technologies have contextualized findings from genetic and animal studies, pinpointing the specific cell types and complex intercellular interactions that contribute to COPD progression (Figure 2).
Lung epithelial dysfunction in COPD. Epithelial injury is central to COPD pathogenesis and occurs in AT2 pneumocytes, cells tasked with production of surfactant and serving as progenitors for alveolar type 1 (AT1) pneumocytes. scRNA-seq studies confirmed that AT2 cells exhibit two distinct functional states — one associated with homeostatic function and high surfactant production and another primed for epithelial repair (168–170). Progenitor AT2 cells give rise to a transitional AT2/AT1 population that is transcriptionally distinct from both lineages yet represents an intermediate cell state along the differentiation trajectory. In mice and organoid models, the intermediate state has been described as Krt8+ alveolar differentiation intermediates (ADI) (171), or prealveolar type 1 transitional state (PATS) (172). A similar population in humans is enriched in chronic lung diseases, such as idiopathic pulmonary fibrosis, and are termed KRT5–KRT17+ or aberrant basaloid cells (173–175).
The characterization of novel terminal airway–enriched secretory cells (TASCs) and respiratory airway secretory (RAS) cells or collectively, terminal and respiratory bronchiolar secretory cells (TRB-SCs), is another important discovery (176, 177). This population are facultative progenitor cells restricted to terminal and respiratory bronchioles, marked by SCGB3A2 and SFTPB expression, and capable of differentiating into AT2 cells after injury. Lineage tracing in mice and organoid models show that these progenitors are regulated by hypoxia (178, 179), Notch, and Wnt (180) signaling, and significantly contribute to alveolar repair after injury (181, 182). Data also suggest that in COPD, SCGB3A2+ airway progenitor cells are depleted or undergo conversion to pathological cell states (183). Airway-derived AT2 cells have reduced regenerative capacity relative to native AT2 cells (183, 184). Collectively, changes in progenitor cell dynamics may reduce epithelial regenerative capacity both in airways and parenchyma in COPD. Single-cell studies have also revealed key insights into proximal airway biology relative to COPD.
Immune, endothelial, and stromal cell dysfunction in COPD. Single-cell profiling has delineated diverse macrophage populations, including alveolar, interstitial, and monocyte-derived subsets, each with specialized roles in lung immunity and remodeling. Notably, CS-induced macrophages originate from recruited monocytes and exhibit PRMT7-driven epigenetic modifications that enhance macrophage activation, monocyte recruitment, and chronic inflammation, ultimately exacerbating lung damage and emphysema (185). Single-cell approaches have shown expansion of cytotoxic CD8+ T cells, particularly TEMRA and tissue-resident memory (TRM) subsets, in COPD lungs (186). These IFN-γ–producing cells can impair AT2 cell function and differentiation of basal cells into TASCs/RAS/TRB-SC cells, altering epithelial regeneration (187). PRMT1 is also downregulated in pulmonary ECs in lungs from humans with COPD and mouse models, and PRMT1 loss exaggerates senescence and cell death via dysregulated NF-κB signaling (188). Single-cell profiling of fibroblasts shows upregulation of ECM remodeling genes that drives fibrosis and airway remodeling, while strongly influencing epithelial and endothelial behaviors through complex cell-cell signaling networks (189). GWAS further support this relationship between COPD and fibroblast biology, as suggested by COPD-associated SNPs in ECM signaling genes and by the presence of emphysema and connective tissue dysfunction in individuals with Mendelian forms of Loeys-Dietz syndrome type 4 and autosomal dominant cutis laxa (190–192).
Multiomic approaches and spatial technologies. Multimodal high-throughput technologies have yielded novel insights into COPD pathobiology. Integration of GWAS with scRNA-seq has enabled cell-type-specific mapping of susceptibility genes and identified enrichment in fibroblasts, smooth muscle cells, and epithelial and endothelial cells (193). Integration of transcriptomic, miRNA, and methylation data from lung tissue revealed that patients with similar clinical features, including severe airflow limitation and emphysema, can harbor distinct molecular endotypes (61). One cluster was marked by elevated B and T cell signatures and downregulation of secretory and ciliated cell genes, while the other lacked immune activation and showed distinct epithelial features.
Spatial technologies are beginning to fundamentally reshape our understanding of lung architecture and disease progression. While scRNA-seq has revealed discrete cellular states and differentiation trajectories, it lacks spatial context, an essential dimension in diseases like COPD (194, 195). Spatial approaches have investigated terminal airway narrowing, an early COPD pathological event that precedes development of emphysematous destruction (196). Airway narrowing is closely associated with loss of elastin fibers at alveolar attachments, which anchor alveoli to the small airways and maintain lung elasticity. Spatial imaging studies show macrophage and neutrophil accumulation around these alveolar attachments, where they are thought to contribute to elastin degradation. In parallel, adaptive immune cells, particularly CD8+ T cells, localize to terminal bronchioles and promote pathological remodeling, further exacerbating airflow limitation (196). This approach revealed that lymphoid follicles in emphysematous lung tissue exhibited a transcriptional profile marked by aberrant B cell activation, autoimmune-associated transcriptional regulators, and enhanced antigen presentation (197). Together, these findings highlight the spatially organized immune-structural interactions that drive early COPD progression.
Spatial metabolomics. Spatial metabolomics, particularly through matrix-assisted laser desorption/ionization (MALDI) imaging, represents another rapidly expanding frontier (198, 199). This technology enables in situ mapping of metabolites, lipids, and glycans at resolutions approaching the single-cell level. Metabolomics offers a direct readout of cellular function and biochemical activity, capturing real-time metabolic consequences of cellular states within intact tissue (200, 201). MALDI-based platforms now support profiling of complex molecular classes, including oxidative stress, that are implicated in COPD pathogenesis.
By integrating information on cell identity, location, and function, spatial metabolomics complements transcriptomic and proteomic data, facilitating generation of new multidimensional mechanistic hypotheses.
-
Translational considerations
Currently, there are no curative or disease-modifying pharmacological therapies for COPD (202). While tobacco consumption and air pollution are leading COPD risk factors, they do not fully explain the risk of disease development or COPD heterogeneity. Genetics is an important contributor to COPD (203, 204), and advances in genotyping and sequencing technologies have made these discoveries possible. The effect size of each genetic signal is modest, limiting the efficacy of single-gene targeting approaches. But combinatorial analyses (i.e., PRS, genetics-genomics integration) invoking potentially targetable pathways are promising.
As is true for most chronic diseases, COPD has a long phase of pathobiological changes that can be detected before clinical diagnosis. Pre-COPD offers a unique opportunity to intervene before physiological reversibility and associated frailty and impaired lung function. Ongoing prospective studies will hopefully contribute to our understanding of early determinants of known comorbidities of patients with COPD, including hypertension, chronic kidney disease, irritable bowel syndrome, dementia, and cancer (205) (Figure 3).
Given the number of COPD-risk-associated loci (55), combinatorial therapy, rather than single agents, will likely be needed to address this disease effectively. In this context, RNA-based therapeutics such as antisense oligonucleotides (ASOs) offer advantages over traditional small-molecule-based drugs (206, 207). ASOs can be rapidly designed, qualify for expedited FDA approval, and allow early detection of off-target effects via transcriptomics (208–210). In 2023, the FDA approved tofersen, an ASO targeting SOD1 mutations in amyotrophic lateral sclerosis (ALS) (211). Given the oligogenic nature of ALS, researchers are now pursuing personalized ASO cocktails tailored to each patient’s specific genetic mutations and relevant nongenetic disease drivers (212, 213).
Too few trials of candidate agents for COPD are being conducted, a clear reflection of suboptimal prioritization of informative trial design. While two previous trials (214) showed limited benefits from early treatment, clinical trials investigating pharmacological interventions in early COPD and pre-COPD are actively underway and hold promising potential. In addition, a vast library of well-characterized FDA-approved medications with potential to be repurposed for new COPD indications are in the pipeline, a strategy widely employed for malignancies and more recently COVID-19 (215, 216). The selection of agents, based on effects on known pathways together with creative trial designs, including antihypertensives (217) and antiglycemics, have been explored for efficacy in COPD trials (218). While pharmacological innovations are essential, preventive strategies aimed at lifestyle modifications such as smoking cessation, reduction of occupational exposures, promotion of physical activity and fitness, and improved diet and nutritional support are equally vital.
-
Conclusions
The COPD-iNET symposium provided an important forum for experts from many fields to engage in discussions and knowledge exchange and underscored that the effects of COPD extend far beyond pulmonary pathology. As COPD associates with multiple comorbidities, mechanistic studies addressing COPD will have far-reaching impact beyond lung pathology and dysfunction. Issues raised in this Review represent the collective expertise and vision of a multidisciplinary group of investigators addressing COPD research and will serve as both a comprehensive resource for the current state of knowledge and a roadmap for future investigations. Our hope is that this worldwide effort in generating datasets that include underrepresented populations and integration of single-cell epigenetic, RNA, proteomic, and metabolomic datasets from patients and COPD models will help accelerate the development of novel therapeutic interventions for COPD. Sustained investment in collaborative network such as COPD-iNET, along with open data sharing and standardized phenotyping, will be crucial to translate these scientific advances into benefits for patients with COPD.
-
Funding support
This work is the result of NIH funding, in whole or in part, and is subject to the NIH Public Access Policy. Through acceptance of this federal funding, the NIH has been given a right to make the work publicly available in PubMed Central.
- NIH grants R01HL155948, R21HL173512, and R01HL153400 (to MS).
- NIH grants R01HL141380 and R01HL179364 (to DC).
- NIH grants R01HL133135, R01HL152728, P01HL114501, and contract no. 75N92023D00011 (to EKS).
- NIH grant R01HL151107 (to VS).
- NIH grants R01HL168199, R01HL162813, R01HL153248, and R01HL135142 (to MHC).
- NIH grant R01HL068111 (to YT).
- NIH grants R01HL140839 and R01HL171213 (to YT and PC).
- NIH grants R01HL154343 and R01HL160008 (to EN).
- NIH grants R01HL146557, R01HL160939, and R01HL153375 (to PRT).
- NIH grant R01ES032081 (to BK).
- Department of Defense grant W81XWH2110414 (to BK).
- Department of Defense grants W81XWH2210629 and HT94252310034 (to MS).
- UK Research and Innovation Future Leaders Fellowship MR/X032914/1 (to RZJ).
- German Center for Lung Research (to AÖY and ML).
- German Research Foundation (DFG) grant 512453064 (to ML).
- Von Behring Röntgen Foundation grant 71_0011 (to ML).
- American Lung Association (to the COPD-iNET Symposium 2024).
-
Acknowledgments
We acknowledge COPD-iNET (https://www.copd-inet.com/) for fostering scientific exchange and collaboration.
Address correspondence to: Yohannes Tesfaigzi, Pulmonary and Critical Care Medicine, Harvard Medical School, 75 Francis St, Boston, Massachusetts 02115, USA. Email: ytesfaigzi@bwh.harvard.edu.
-
Footnotes
Conflict of interest: EKS received institutional grant support from Bayer and Northpond Laboratories. YT received grant support from Astrazeneca and Verra Therapeutics.
Copyright: © 2026, Tesfaigzi et al. This is an open access article published under the terms of the Creative Commons Attribution 4.0 International License.
Reference information: JCI Insight. 2026;11(4):e199693. https://doi.org/10.1172/jci.insight.199693.
-
References
- Adeloye D, et al. Global, regional, and national prevalence of, and risk factors for, chronic obstructive pulmonary disease (COPD) in 2019: a systematic review and modelling analysis. Lancet Respir Med. 2022;10(5):447–458.
- GBD Chronic Respiratory Disease Collaborators. Prevalence and attributable health burden of chronic respiratory diseases, 1990-2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet Respir Med. 2020;8(6):585–596.
- GBD 2021 HAP Collaborators. Global, regional, and national burden of household air pollution, 1990-2021: a systematic analysis for the Global Burden of Disease Study 2021. Lancet. 2025;405(10485):1167–1181.
- Global Initiative for Chronic Obstructive Lung Disease. Global strategy for the diagnosis, management, and prevention of chronic obstructive pulmonary disease. https://goldcopd.org/ Accessed February 5, 2026.
- Bhatt SP, et al. Chronic obstructive pulmonary disease: hiding in plain sight, a statement from the COPD Foundation Medical and Scientific Advisory Committee. Lancet Respir Med. 2023;11(12):1041–1043.
- Pott H, et al. Breathing barriers: bridging lung health, research, and awareness. Lancet Respir Med. 2025;13(8):665–667.
- Yildirim AO, et al. COPD-iNET: a call to the lung community for action to combat the global epidemic of COPD. Eur Respir J. 2024;64(3):2400921.
- No authors listed. Standardization of spirometry--1987 update. Standardization of spirometry--1987 update. Statement of the American Thoracic Society. Am Rev Respir Dis. 1987;136(5):1285–1298.
- Rodriguez-Roisin R, et al. Global Initiative for Chronic Obstructive Lung Disease (GOLD) 20th anniversary: a brief history of time. Eur Respir J. 2017;50(1):1700671.
- Rodriguez-Roisin R, et al. Chronic respiratory symptoms with normal spirometry. A reliable clinical entity? Am J Respir Crit Care Med. 2017;195(1):17–22.
- Tuder RM, Petrache I. Pathogenesis of chronic obstructive pulmonary disease. J Clin Invest. 2012;122(8):2749–2755.
- Bhatt SP, et al. Dupilumab for COPD with blood eosinophil evidence of type 2 inflammation. N Engl J Med. 2024;390(24):2274–2283.
- Vestbo J, Lange P. Can GOLD Stage 0 provide information of prognostic value in chronic obstructive pulmonary disease? Am J Respir Crit Care Med. 2002;166(3):329–332.
- Celli BR, Agusti A. COPD: time to improve its taxonomy? ERJ Open Res. 2018;4(1):00132-2017.
- Celli B, et al. Definition and nomenclature of chronic obstructive pulmonary disease: time for its revision. Am J Respir Crit Care Med. 2022;206(11):1317–1325.
- Divo MJ, et al. From pre-COPD to COPD: a simple, low cost and easy to IMplement (SLIM) risk calculator. Eur Respir J. 2023;62(3):2300806.
- Han MK, et al. From GOLD 0 to pre-COPD. Am J Respir Crit Care Med. 2021;203(4):414–423.
- Sugawara H, et al. Association between annual change in FEV1 and comorbidities or impulse oscillometry in chronic obstructive pulmonary disease. BMC Pulm Med. 2022;22(1):185.
- Labaki WW, et al. The role of chest computed tomography in the evaluation and management of the patient with chronic obstructive pulmonary disease. Am J Respir Crit Care Med. 2017;196(11):1372–1379.
- Polverino F, et al. Lung MRI as a potential complementary diagnostic tool for early COPD. Am J Med. 2020;133(6):757–760.
- Robertson NM, et al. Integrating artificial intelligence in the diagnosis of COPD globally: a way forward. Chronic Obstr Pulm Dis. 2024;11(1):114–120.View this article via: PubMed Google Scholar
- Wang C, et al. Artificial intelligence enhanced sensors - enabling technologies to next-generation healthcare and biomedical platform. Bioelectron Med. 2023;9(1):17.
- Sikkema L, et al. An integrated cell atlas of the lung in health and disease. Nat Med. 2023;29(6):1563–1577.
- Lange P, et al. Lung-function trajectories leading to chronic obstructive pulmonary disease. N Engl J Med. 2015;373(2):111–122.
- Washko GR, et al. Adult life-course trajectories of lung function and the development of emphysema: the CARDIA Lung Study. Am J Med. 2020;133(2):222–230.e11.
- Wan ES, et al. Epidemiology, genetics, and subtyping of preserved ratio impaired spirometry (PRISm) in COPDGene. Respir Res. 2014;15(1):89.
- Arjomandi M, et al. Phenotypes and trajectories of tobacco-exposed persons with preserved spirometry: insights from lung volumes. Ann Am Thorac Soc. 2024;22(4):494–505.
- Reyfman PA, et al. Study protocol for a national cohort of adults focused on respiratory health: the American Lung Association Lung Health Cohort (ALA-LHC) study. BMJ Open. 2021;11(7):e053342.
- Lee AG, et al. Prenatal household air pollution is associated with impaired infant lung function with sex-specific effects. Evidence from GRAPHS, a cluster randomized cookstove intervention trial. Am J Respir Crit Care Med. 2019;199(6):738–746.
- Bui DS, et al. Childhood predictors of lung function trajectories and future COPD risk: a prospective cohort study from the first to the sixth decade of life. Lancet Respir Med. 2018;6(7):535–544.
- Perret JL, et al. Associations between life-course FEV1/FVC trajectories and respiratory symptoms up to middle age: analysis of data from two prospective cohort studies. Lancet Respir Med. 2025;13(2):130–140.
- Olvera N, et al. Circulating biomarkers in young individuals with low peak FEV1. Am J Respir Crit Care Med. 2023;207(3):354–358.
- Hernandez-Pacheco N, et al. Exploring the genetics of airflow limitation in lung function across the lifespan - a polygenic risk score study. EClinicalMedicine. 2024;75:102731.
- Olvera N, et al. Heterogeneity of reduced FEV1 in early adulthood: a looking forward, looking backwards analysis. Respirology. 2025;30(4):326–334.
- Ngo D, et al. Systemic markers of lung function and forced expiratory volume in 1 second decline across diverse cohorts. Ann Am Thorac Soc. 2023;20(8):1124–1135.
- Esther CR, JrIdentification of sputum biomarkers predictive of pulmonary exacerbations in COPD. Chest. 2022;161(5):1239–1249.
- Guerra S, et al. Relation between circulating CC16 concentrations, lung function, and development of chronic obstructive pulmonary disease across the lifespan: a prospective study. Lancet Respir Med. 2015;3(8):613–620.
- Cheng DT, et al. Systemic soluble receptor for advanced glycation endproducts is a biomarker of emphysema and associated with AGER genetic variants in patients with chronic obstructive pulmonary disease. Am J Respir Crit Care Med. 2013;188(8):948–957.
- Zemans RL, et al. Multiple biomarkers predict disease severity, progression and mortality in COPD. Respir Res. 2017;18(1):117.
- Moll M, et al. Chronic obstructive pulmonary disease and related phenotypes: polygenic risk scores in population-based and case-control cohorts. Lancet Respir Med. 2020;8(7):696–708.
- Bui DS, et al. Association between very to moderate preterm births, lung function deficits, and COPD at age 53 years: analysis of a prospective cohort study. Lancet Respir Med. 2022;10(5):478–484.
- Izadi N, et al. Factors associated with persistence of severe asthma from late adolescence to early adulthood. Am J Respir Crit Care Med. 2021;204(7):776–787.
- Tai A, et al. The association between childhood asthma and adult chronic obstructive pulmonary disease. Thorax. 2014;69(9):805–810.
- Cho MH, et al. Genetics of chronic obstructive pulmonary disease: understanding the pathobiology and heterogeneity of a complex disorder. Lancet Respir Med. 2022;10(5):485–496.
- Yang IA, et al. Chronic obstructive pulmonary disease in never-smokers: risk factors, pathogenesis, and implications for prevention and treatment. Lancet Respir Med. 2022;10(5):497–511.
- Agusti A, et al. Pathogenesis of chronic obstructive pulmonary disease: understanding the contributions of gene-environment interactions across the lifespan. Lancet Respir Med. 2022;10(5):512–524.
- Laurell CB, Eriksson S. The electrophoretic α1-globulin pattern of serum in α1-antitrypsin deficiency. 1963. COPD. 1963;10 Suppl 1:3–8.View this article via: PubMed Google Scholar
- Silverman EK, Sandhaus RA. Clinical practice. Alpha1-antitrypsin deficiency. N Engl J Med. 2009;360(26):2749–2757.
- de Serres FJ, Blanco I. Prevalence of α1-antitrypsin deficiency alleles PI*S and PI*Z worldwide and effective screening for each of the five phenotypic classes PI*MS, PI*MZ, PI*SS, PI*SZ, and PI*ZZ: a comprehensive review. Ther Adv Respir Dis. 2012;6(5):277–295.
- Silverman EK, et al. Family study of alpha 1-antitrypsin deficiency: effects of cigarette smoking, measured genotype, and their interaction on pulmonary function and biochemical traits. Genet Epidemiol. 1992;9(5):317–331.
- Visscher PM, et al. 10 years of GWAS discovery: biology, function, and translation. Am J Hum Genet. 2017;101(1):5–22.
- Hancock DB, et al. Meta-analyses of genome-wide association studies identify multiple loci associated with pulmonary function. Nat Genet. 2010;42(1):45–52.
- Soler Artigas M, et al. Genome-wide association and large-scale follow up identifies 16 new loci influencing lung function. Nat Genet. 2011;43(11):1082–1090.
- Cho MH, et al. Risk loci for chronic obstructive pulmonary disease: a genome-wide association study and meta-analysis. Lancet Respir Med. 2014;2(3):214–225.
- Sakornsakolpat P, et al. Genetic landscape of chronic obstructive pulmonary disease identifies heterogeneous cell-type and phenotype associations. Nat Genet. 2019;51(3):494–505.
- Shrine N, et al. Multi-ancestry genome-wide association analyses improve resolution of genes and pathways influencing lung function and chronic obstructive pulmonary disease risk. Nat Genet. 2023;55(3):410–422.
- Hindorff LA, et al. Potential etiologic and functional implications of genome-wide association loci for human diseases and traits. Proc Natl Acad Sci U S A. 2009;106(23):9362–9367.
- Hobbs BD, et al. Genetic loci associated with chronic obstructive pulmonary disease overlap with loci for lung function and pulmonary fibrosis. Nat Genet. 2017;49(3):426–432.
- Tesfaigzi Y, et al. Does chronic obstructive pulmonary disease originate from different cell types? Am J Respir Cell Mol Biol. 2023;69(5):500–507.
- Moll M, et al. Polygenic and transcriptional risk scores identify chronic obstructive pulmonary disease subtypes in the COPDGene and ECLIPSE cohort studies. EBioMedicine. 2024;110:105429.
- Olvera N, et al. Lung tissue multilayer network analysis uncovers the molecular heterogeneity of chronic obstructive pulmonary disease. Am J Respir Crit Care Med. 2024;210(10):1219–1229.
- Castaldi PJ, et al. Do COPD subtypes really exist? COPD heterogeneity and clustering in 10 independent cohorts. Thorax. 2017;72(11):998–1006.
- Castaldi PJ, et al. Machine learning characterization of COPD subtypes: insights from the COPDGene study. Chest. 2020;157(5):1147–1157.
- Natri HM, et al. Cell-type-specific and disease-associated expression quantitative trait loci in the human lung. Nat Genet. 2024;56(4):595–604.
- Gauderman WJ, et al. The effect of air pollution on lung development from 10 to 18 years of age. N Engl J Med. 2004;351(11):1057–1067.
- Morawska L, Buonanno G. The physics of particle formation and deposition during breathing. Nat Rev Phys. 2021;3(5):300–301.
- Huh J-Y, et al. The impact of air pollutants and meteorological factors on chronic obstructive pulmonary disease exacerbations: a nationwide study. Ann Am Thorac Soc. 2022;19(2):214–226.
- Sin DD, et al. Air pollution and COPD: GOLD 2023 committee report. Eur Respir J. 2023;61(5):2202469.
- Liu S, et al. Long-term exposure to low-level air pollution and incidence of asthma: the ELAPSE project. Eur Respir J. 2021;57(6):2003099.
- Rice MB, et al. Long-term exposure to traffic emissions and fine particulate matter and lung function decline in the Framingham heart study. Am J Respir Crit Care Med. 2015;191(6):656–664.
- Sood A, et al. Wood smoke exposure and gene promoter methylation are associated with increased risk for COPD in smokers. Am J Respir Crit Care Med. 2010;182(9):1098–1104.
- Leng S, et al. Wood smoke exposure affects lung aging, quality of life, and all-cause mortality in New Mexican smokers. Respir Res. 2022;23(1):236.
- Hansel NN, et al. Indoor pollution and lung function decline in current and former smokers: SPIROMICS AIR. Am J Respir Crit Care Med. 2023;208(10):1042–1051.
- Verleden SE, et al. Small airway loss in the physiologically ageing lung: a cross-sectional study in unused donor lungs. Lancet Respir Med. 2021;9(2):167–174.
- Camp PG, et al. COPD phenotypes in biomass smoke- versus tobacco smoke-exposed Mexican women. Eur Respir J. 2014;43(3):725–734.
- Perez-Bautista O, et al. Women with COPD by biomass show different serum profile of adipokines, incretins, and peptide hormones than smokers. Respir Res. 2018;19(1):239.
- Akdis CA, Nadeau KC. Human and planetary health on fire. Nat Rev Immunol. 2022;22(11):651–652.
- Boğan M, et al. Effect of desert dust storms and meteorological factors on respiratory diseases. Allergy. 2022;77(7):2243–2246.
- Romanello M, et al. The 2023 report of the Lancet Countdown on health and climate change: the imperative for a health-centred response in a world facing irreversible harms. Lancet. 2023;402(10419):2346–2394.
- Wu Y, et al. Association between wildfire-related PM(2.5) and epigenetic aging: a twin and family study in Australia. J Hazard Mater. 2025;481:136486. View this article via: CrossRef Google Scholar
- Vestbo J, et al. Should we view chronic obstructive pulmonary disease differently after ECLIPSE? A clinical perspective from the study team. Am J Respir Crit Care Med. 2014;189(9):1022–1030.
- Mannino DM, Buist AS. Global burden of COPD: risk factors, prevalence, and future trends. Lancet. 2007;370(9589):765–773.
- Salvi SS, Barnes PJ. Chronic obstructive pulmonary disease in non-smokers. Lancet. 2009;374(9691):733–743.
- Kurmi OP, et al. COPD and chronic bronchitis risk of indoor air pollution from solid fuel: a systematic review and meta-analysis. Thorax. 2010;65(3):221–228.
- Hu G, et al. Risk of COPD from exposure to biomass smoke: a metaanalysis. Chest. 2010;138(1):20–31.
- Po JY, et al. Respiratory disease associated with solid biomass fuel exposure in rural women and children: systematic review and meta-analysis. Thorax. 2011;66(3):232–239.
- Sood A, et al. ERS/ATS workshop report on respiratory health effects of household air pollution. Eur Respir J. 2018;51(1):1700698.
- Peng RD, et al. Emergency admissions for cardiovascular and respiratory diseases and the chemical composition of fine particle air pollution. Environ Health Perspect. 2009;117(6):957–963.
- Bell ML, et al. Hospital admissions and chemical composition of fine particle air pollution. Am J Respir Crit Care Med. 2009;179(12):1115–1120.
- Cedeno Laurent JG, et al. Physicochemical characterization of the particulate matter in New Jersey/New York City area, resulting from the Canadian Quebec wildfires in June 2023. Environ Sci Technol. 2024;58(33):14753–14763.
- Wegesser TC, et al. California wildfires of 2008: coarse and fine particulate matter toxicity. Environ Health Perspect. 2009;117(6):893–897.
- Antwi GO, Rhodes DL. Association between E-cigarette use and chronic obstructive pulmonary disease in non-asthmatic adults in the USA. J Public Health (Oxf). 2022;44(1):158–164.
- Song B, et al. Impact of electronic cigarette usage on the onset of respiratory symptoms and COPD among Chinese adults. Sci Rep. 2024;14(1):5598.
- Khabour OF, et al. Acute exposure to waterpipe tobacco smoke induces changes in the oxidative and inflammatory markers in mouse lung. Inhal Toxicol. 2012;24(10):667–675.
- Ghosh B, et al. Effect of sub-chronic exposure to cigarette smoke, electronic cigarette and waterpipe on human lung epithelial barrier function. BMC Pulm Med. 2020;20(1):216.
- Rammah M, et al. In vitro effects of waterpipe smoke condensate on endothelial cell function: a potential risk factor for vascular disease. Toxicol Lett. 2013;219(2):133–142.
- Awji EG, et al. Correlation of cigarette smoke-induced pulmonary inflammation and emphysema in C3H and C57Bl/6 Mice. Toxicol Sci. 2015;147(1):75–83.
- Tassew D, et al. Effects of wood smoke constituents on mucin gene expression in mice and human airway epithelial cells and on nasal epithelia of subjects with a susceptibility gene variant in Tp53. Environ Health Perspect. 2022;130(1):17010.
- Zong D, et al. The role of cigarette smoke-induced epigenetic alterations in inflammation. Epigenetics Chromatin. 2019;12(1):65.
- Gavito-Covarrubias D, et al. Epigenetic mechanisms of particulate matter exposure: air pollution and hazards on human health. Front Genet. 2023;14:1306600.
- Li Y, et al. The interplay between DNA and histone methylation: molecular mechanisms and disease implications. EMBO Rep. 2021;22(5):e51803.
- Yeung-Luk BH, et al. Epigenetic reprogramming drives epithelial disruption in chronic obstructive pulmonary disease. Am J Respir Cell Mol Biol. 2024;70(3):165–177.
- Casas-Recasens S, et al. Lung DNA methylation in chronic obstructive pulmonary disease: relationship with smoking status and airflow limitation severity. Am J Respir Crit Care Med. 2021;203(1):129–134.
- Schwartz U, et al. High-resolution transcriptomic and epigenetic profiling identifies novel regulators of COPD. EMBO J. 2023;42(12):e111272.
- Jurkowska RZ. Role of epigenetic mechanisms in the pathogenesis of chronic respiratory diseases and response to inhaled exposures: from basic concepts to clinical applications. Pharmacol Ther. 2024;264:108732.
- Zhang X, et al. TET (Ten-eleven translocation) family proteins: structure, biological functions and applications. Signal Transduct Target Ther. 2023;8(1):297.
- Zeng Z, et al. DNA dioxygenases TET2 deficiency promotes cigarette smoke induced chronic obstructive pulmonary disease by inducing ferroptosis of lung epithelial cell. Redox Biol. 2023;67:102916.
- Lyko F. The DNA methyltransferase family: a versatile toolkit for epigenetic regulation. Nat Rev Genet. 2018;19(2):81–92.
- Zeng H, et al. Oxidative stress mediates the apoptosis and epigenetic modification of the Bcl-2 promoter via DNMT1 in a cigarette smoke-induced emphysema model. Respir Res. 2020;21(1):229.
- Kreutzer DA, Essigmann JM. Oxidized, deaminated cytosines are a source of C → T transitions in vivo. Proc Natl Acad U S A. 1998;95(7):3578–3582.View this article via: CrossRef Google Scholar
- Lam H, et al. Histone deacetylase 6-mediated selective autophagy regulates COPD-associated cilia dysfunction. J Clin Invest. 2013;123(12):5212–5230.
- Szulakowski P, et al. The effect of smoking on the transcriptional regulation of lung inflammation in patients with chronic obstructive pulmonary disease. Am J Respir Crit Care Med. 2006;174(1):41–50.
- Igolkina AA, et al. H3K4me3, H3K9ac, H3K27ac, H3K27me3 and H3K9me3 histone tags suggest distinct regulatory evolution of open and condensed chromatin landmarks. Cells. 2019;8(9):1034.
- Ohm JE, et al. A stem cell-like chromatin pattern may predispose tumor suppressor genes to DNA hypermethylation and heritable silencing. Nat Genet. 2007;39(2):237–242.
- Conickx G, et al. MicroRNA profiling reveals a role for MicroRNA-218-5p in the pathogenesis of chronic obstructive pulmonary disease. Am J Respir Crit Care Med. 2017;195(1):43–56.
- Hobbs BD, Tantisira KG. MicroRNAs in COPD: small molecules with big potential. Eur Respir J. 2019;53(4):1900515.
- Devulder JV, et al. Chronic obstructive pulmonary disease airway epithelial cell-derived extracellular vesicles spread cellular senescence via MicroRNA-34a. Am J Respir Cell Mol Biol. 2025;73(2):210–220.
- Li R, et al. Lung microbiome: new insights into the pathogenesis of respiratory dis eases. Signal Transduct Target Ther. 2024;9(1):19.
- Sze MA, et al. The lung tissue microbiome in chronic obstructive pulmonary disease. Am J Respir Crit Care Med. 2012;185(10):1073–1080.
- Rascon-Aguilar IE, et al. Role of gastroesophageal reflux symptoms in exacerbations of COPD. Chest. 2006;130(4):1096–1101.
- Smaldone GC, et al. Regional impairment of mucociliary clearance in chronic obstructive pulmonary disease. Chest. 1993;103(5):1390–1396.
- Azarpazhooh A, Leake JL. Systematic review of the association between respiratory diseases and oral health. J Periodontol. 2006;77(9):1465–1482.
- Wright JL, et al. Animal models of chronic obstructive pulmonary disease. Am J Physiol Lung Cell Mol Physiol. 2008;295(1):L1–15.
- Gruenert DC, et al. Culture and transformation of human airway epithelial cells. Am J Physiol. 1995;268(3 pt 1):L347–L360.View this article via: PubMed Google Scholar
- Benam KH, et al. Breaking the in vitro barrier in respiratory medicine. Engineered microphysiological systems for chronic obstructive pulmonary disease and beyond. Am J Respir Crit Care Med. 2018;197(7):869–875.
- Niemeyer BF, et al. Advanced microengineered lung models for translational drug discovery. SLAS Discov. 2018;23(8):777–789.
- Benam KH, et al. Exploring new technologies in biomedical research. Drug Discov Today. 2019;24(6):1242–1247.
- Vo Q, Benam KH. Advancements in preclinical human-relevant modeling of pulmonary vasculature on-chip. Eur J Pharm Sci. 2024;195:106709.
- Vo Q, et al. On-chip reconstitution of uniformly shear-sensing 3D matrix-embedded multicellular blood microvessel. Adv Funct Mater. 2024;34(10):2304630.
- Huh D, et al. Reconstituting organ-level lung functions on a chip. Science. 2010;328(5986):1662–1668.
- Si L, et al. A human-airway-on-a-chip for the rapid identification of candidate antiviral therapeutics and prophylactics. Nat Biomed Eng. 2021;5(8):815–829.
- Koziol-White C, et al. Precision cut lung slices: an integrated ex vivo model for studying lung physiology, pharmacology, disease pathogenesis and drug discovery. Respir Res. 2024;25(1):231.
- Bailey KE, et al. Embedding of precision-cut lung slices in engineered hydrogel biomaterials supports extended ex vivo culture. Am J Respir Cell Mol Biol. 2020;62(1):14–22.
- Lehmann M, et al. Precision-cut lung slices: emerging tools for preclinical and translational lung research: an official American Thoracic Society Workshop report. Am J Respir Cell Mol Biol. 2024;72(1):16–31.
- Van Dijk EM, et al. Elastase-induced parenchymal disruption and airway hyper responsivenes s in mouse precision cut lung slices: toward an ex vivo COPD model. Front Physiol. 2016;7:657.
- Uhl FE, et al. Preclinical validation and imaging of Wnt-induced repair in human 3D lung tissue cultures. Eur Respir J. 2015;46(4):1150–1166.
- Chen J, Na F. Organoid technology and applications in lung diseases: Models, mechanism research and therapy opportunities. Front Bioeng Biotechnol. 2022;10:1066869.
- Wu X, et al. A transcriptomics-guided drug target discovery strategy identifies receptor ligands for lung regeneration. Sci Adv. 2022;8(12):eabj9949.
- Wang C, et al. Expansion of hedgehog disrupts mesenchymal identity and induces emphysema phenotype. J Clin Invest. 2018;128(10):4343–4358.
- Werder RB, et al. The COPD GWAS gene ADGRG6 instructs function and injury response in human iPSC-derived type II alveolar epithelial cells. Am J Hum Genet. 2023;110(10):1735–1749.
- Nikolaev M, et al. Homeostatic mini-intestines through scaffold-guided organoid morphogenesis. Nature. 2020;585(7826):574–578.
- Radder JE, et al. Variable susceptibility to cigarette smoke-induced emphysema in 34 inbred strains of mice implicates Abi3bp in emphysema susceptibility. Am J Respir Cell Mol Biol. 2017;57(3):367–375.
- March TH, et al. Cigarette smoke exposure produces more evidence of emphysema in B6C3F1 mice than in F344 rats. Toxicol Sci. 1999;51(2):289–299.
- Simborio H, et al. Mitochondrial dysfunction and impaired DNA damage repair through PICT1 dysregulation in alveolar type II cells in emphysema. Cell Commun Signal. 2024;22(1):562.
- Churg A, Wright JL. Testing drugs in animal models of cigarette smoke-induced chronic obstructive pulmonary disease. Proc Am Thorac Soc. 2009;6(6):550–552.
- March TH, et al. Enhanced pulmonary epithelial replication and axial airway mucosubstance changes in F344 rats exposed short-term to mainstream cigarette smoke. Toxicol Appl Pharmacol. 1999;161(2):171–179.
- Zou Y, et al. Upregulation of gelatinases and epithelial-mesenchymal transition in small airway remodeling associated with chronic exposure to wood smoke. PLoS One. 2014;9(5):e96708.
- DeMeo DL, Silverman EK. Alpha1-antitrypsin deficiency. 2: genetic aspects of alpha(1)-antitrypsin deficiency: phenotypes and genetic modifiers of emphysema risk. Thorax. 2004;59(3):259–264.
- Jiang J, et al. Gene signatures from scRNA-seq accurately quantify mast cells in biopsies in asthma. Clin Exp Allergy. 2020;50(12):1428–1431.
- Hunt BC, et al. Haemophilus influenzae persists in biofilm communities in a smoke-exposed ferret model of COPD. ERJ Open Res. 2020;6(3):00200-2020.
- Plopper CG, Hyde DM. The non-human primate as a model for studying COPD and asthma. Pulm Pharmacol Ther. 2008;21(5):755–766.
- Polverino F, et al. A novel nonhuman primate model of cigarette smoke-induced airway disease. Am J Pathol. 2015;185(3):741–755.
- Jang JH, et al. Connective tissue growth factor promotes pulmonary epithelial cell senescence and is associated with COPD severity. COPD. 2017;14(2):228–237.
- Xu X, et al. The heterogeneity of inflammatory response and emphysema in chronic obstructive pulmonary disease. Front Physiol. 2021;12:783396.
- Sajjan U, et al. Elastase- and LPS-exposed mice display altered responses to rhinovirus infection. Am J Physiol Lung Cell Mol Physiol. 2009;297(5):L931–L944.
- Kang MJ, et al. Cigarette smoke selectively enhances viral PAMP- and virus-induced pulmonary innate immune and remodeling responses in mice. J Clin Invest. 2008;118(8):2771–2784.
- Mebratu YA, et al. Inflammation and emphysema in cigarette smoke-exposed mice when instilled with poly (I:C) or infected with influenza A or respiratory syncytial viruses. Respir Res. 2016;17(1):75.
- Singanayagam A, et al. Airway mucins promote immunopathology in virus-exacerbated chronic obstructive pulmonary disease. J Clin Invest. 2022;132(8):e120901.
- Alam S, et al. Z α1-antitrypsin confers a proinflammatory phenotype that contributes to chronic obstructive pulmonary disease. Am J Respir Crit Care Med. 2014;189(8):909–931.
- Parums DV. Editorial: Global initiative for chronic obstructive lung disease (GOLD) 2023 guidelines for COPD, including COVID-19, climate change, and air pollution. Med Sci Monit. 2023;29:e942672. View this article via: PubMed Google Scholar
- Deslee G, et al. Cigarette smoke induces nucleic-acid oxidation in lung fibroblasts. Am J Respir Cell Mol Biol. 2010;43(5):576–584.
- Burgstaller G, et al. The instructive extracellular matrix of the lung: basic composition and alterations in chronic lung disease. Eur Respir J. 2017;50(1):1601805.
- Wright JL, Churg A. Smoke-induced emphysema in guinea pigs is associated with morphometric evidence of collagen breakdown and repair. Am J Physiol. 1995;268(1 pt 1):L17–L20.View this article via: PubMed Google Scholar
- Suki B, Bates JHT. Extracellular matrix mechanics in lung parenchymal diseases. Respir Physiol Neurobiol. 2008;163(1-3):33–43.
- Churg A, et al. Macrophage metalloelastase mediates acute cigarette smoke-induced inflammation via tumor necrosis factor-alpha release. Am J Respir Crit Care Med. 2003;167(8):1083–1089.
- Hunninghake GM, et al. MMP12, lung function, and COPD in high-risk populations. N Engl J Med. 2009;361(27):2599–2608.
- Spix B, et al. Lung emphysema and impaired macrophage elastase clearance in mucolipin 3 deficient mice. Nat Commun. 2022;13(1):318.
- Travaglini KJ, et al. A molecular cell atlas of the human lung from single-cell RNA sequencing. Nature. 2020;587(7835):619–625.
- Zacharias WJ, et al. Regeneration of the lung alveolus by an evolutionarily conserved epithelial progenitor. Nature. 2018;555(7695):251–255.
- Nabhan AN, et al. Single-cell Wnt signaling niches maintain stemness of alveolar type 2 cells. Science. 2018;359(6380):1118–1123.
- Strunz M, et al. Alveolar regeneration through a Krt8+ transitional stem cell state that persists in human lung fibrosis. Nat Commun. 2020;11(1):3559.
- Kobayashi H, et al. Production of IL-13 by human lung mast cells in response to Fcepsilon receptor cross-linkage. Clin Exp Allergy. 1998;28(10):1219–1227.
- Habermann AC, et al. Single-cell RNA sequencing reveals profibrotic roles of distinct epithelial and mesenchymal lineages in pulmonary fibrosis. Sci Adv. 2020;6(28):eaba1972.
- Adams TS, et al. Single-cell RNA-seq reveals ectopic and aberrant lung-resident cell populations in idiopathic pulmonary fibrosis. Sci Adv. 2020;6(28):eaba1983.
- Wang F, et al. Regulation of epithelial transitional states in murine and human pulmonary fibrosis. J Clin Invest. 2023;133(22):e165612.
- Basil MC, et al. Human distal airways contain a multipotent secretory cell that can regenerate alveoli. Nature. 2022;604(7904):120–126.
- Murthy PKL, et al. Human distal lung maps and lineage hierarchies reveal a bipotent progenitor. Nature. 2022;604(7904):111–119.
- McCall AS, et al. Hypoxia-inducible factor 2 regulates alveolar regeneration after repetitive injury in three-dimensional cellular and in vivo models. Sci Transl Med. 2025;17(780):eadk8623.
- Xi Y, et al. Local lung hypoxia determines epithelial fate decisions during alveolar regeneration. Nat Cell Biol. 2017;19(8):904–914.
- Hu Y, et al. Wnt/β-catenin signaling is critical for regenerative potential of distal lung epithelial progenitor cells in homeostasis and emphysema. Stem Cells. 2020;38(11):1467–1478.
- Ting C, et al. Biomarkers unveil insights into pathology of transitional epithelial states in pulmonary fibrosis. Am J Respir Crit Care Med. 2024;210(5):687–690.
- Kathiriya JJ, Peng T. An inflammatory switch for stem cell plasticity. Nat Cell Biol. 2021;23(9):928–929.
- Hu Y, et al. Airway-derived emphysema-specific alveolar type II cells exhibit impaired regenerative potential in COPD. Eur Respir J. 2024;64(6):2302071.
- Zepp JA, et al. Genomic, epigenomic, and biophysical cues controlling the emergence of the lung alveolus. Science. 2021;371(6534):eabc3172.
- Gunes Gunsel G, et al. The arginine methyltransferase PRMT7 promotes extravasation of monocytes resulting in tissue injury in COPD. Nat Commun. 2022;13(1):1303.
- Villasenor-Altamirano AB, et al. Activation of CD8+ T cells in chronic obstructive pulmonary disease lung. Am J Respir Crit Care Med. 2023;208(11):1177–1195.
- Wang C, et al. Dysregulated lung stroma drives emphysema exacerbation by potentiating resident lymphocytes to suppress an epithelial stem cell reservoir. Immunity. 2023;56(3):576–591.
- Tran TTV, et al. PRMT1 ablation in endothelial cells causes endothelial dysfunction and aggravates COPD attributable to dysregulated NF-κB signaling. Adv Sci (Weinh). 2025;12(19):e2411514. View this article via: PubMed Google Scholar
- Blackburn JB, et al. A single-cell RNA sequencing atlas of the chronic obstructive pulmonary disease distal lung to predict cell-cell communication. Am J Respir Cell Mol Biol. 2025;72(3):332–335.
- Parker MM, et al. Identification of an emphysema-associated genetic variant near TGFB2 with regulatory effects in lung fibroblasts. Elife. 2019;8:e42720.
- Lindsay ME, et al. Loss-of-function mutations in TGFB2 cause a syndromic presentation of thoracic aortic aneurysm. Nat Genet. 2012;44(8):922–927.
- Saferali A, et al. Characterisation of a COPD-associated nephronectin (NPNT) functional splicing genetic variant in human lung tissue via long-read sequencing. Eur Respir J. 2025;65(4):2401407.
- Sauler M, et al. Characterization of the COPD alveolar niche using single-cell RNA sequencing. Nat Commun. 2022;13(1):494.
- Vannan A, et al. Spatial transcriptomics identifies molecular niche dysregulation associated with distal lung remodeling in pulmonary fibrosis. Nat Genet. 2025;57(3):647–658.
- Madissoon E, et al. A spatially resolved atlas of the human lung characterizes a gland-associated immune niche. Nat Genet. 2023;55(1):66–77.
- Booth S, et al. A single-cell atlas of small airway disease in chronic obstructive pulmonary disease: a cross-sectional study. Am J Respir Crit Care Med. 2023;208(4):472–486.
- Rojas-Quintero J, et al. Spatial transcriptomics resolve an emphysema-specific lymphoid follicle B cell signature in COPD. Am J Respir Crit Care Med. 2024;209(1):48–58.
- Conroy LR, et al. Spatial metabolomics reveals glycogen as an actionable target for pulmonary fibrosis. Nat Commun. 2023;14(1):2759.
- Alexandrov T. Spatial metabolomics and imaging mass spectrometry in the age of artificial intelligence. Annu Rev Biomed Data Sci. 2020;3:61–87.
- Doglioni G, et al. Aspartate signalling drives lung metastasis via alternative translation. Nature. 2025;638(8049):244–250.
- Stevens NC, et al. Resolving multi-image spatial lipidomic responses to inhaled toxicants by machine learning. Nat Commun. 2025;16(1):2954.
- Vogelmeier CF, et al. Global strategy for the diagnosis, management, and prevention of chronic obstructive lung disease 2017 Report. GOLD executive summary. Am J Respir Crit Care Med. 2017;195(5):557–582.
- Ingebrigtsen T, et al. Genetic influences on chronic obstructive pulmonary disease - a twin study. Respir Med. 2010;104(12):1890–1895.
- Zhou JJ, et al. Heritability of chronic obstructive pulmonary disease and related phenotypes in smokers. Am J Respir Crit Care Med. 2013;188(8):941–947.
- Vutcovici M, et al. Inflammatory bowel disease and risk of mortality in COPD. Eur Respir J. 2016;47(5):1357–1364.
- Echigoya Y, Yokota T. Skipping multiple exons of dystrophin transcripts using cocktail antisense oligonucleotides. Nucleic Acid Ther. 2014;24(1):57–68.
- Gaponova S, et al. Single shot vs cocktail: a comparison of mono- and combinative application of miRNA-targeted mesyl oligonucleotides for efficient antitumor therapy. Cancers (Basel). 2022;14(18):4396.
- Shao Y, et al. Rational design and rapid screening of antisense oligonucleotides for prokaryotic gene modulation. Nucleic Acids Res. 2006;34(19):5660–5669.
- Hagedorn PH, et al. Identifying and avoiding off-target effects of RNase H-dependent antisense oligonucleotides in mice. Nucleic Acids Res. 2018;46(11):5366–5380.
- Sang A, et al. Mechanisms of action of the US Food and Drug Administration-approved antisense oligonucleotide drugs. BioDrugs. 2024;38(4):511–526.
- Saini A, Chawla PA. Breaking barriers with tofersen: Enhancing therapeutic opportunities in amyotrophic lateral sclerosis. Eur J Neurol. 2024;31(2):e16140.
- Helm J, et al. Towards personalized allele-specific antisense oligonucleotide therapies for toxic gain-of-function neurodegenerative diseases. Pharmaceutics. 2022;14(8):1708.
- Means JC, et al. Rapid and scalable personalized ASO screening in patient-derived organoids. Nature. 2025;638(8049):237–243.
- Han MK, et al. Bronchodilators in tobacco-exposed persons with symptoms and preserved lung function. N Engl J Med. 2022;387(13):1173–1184.
- Zhou G, et al. Repurposed drug studies on the primary prevention of SARS-CoV-2 infection during the pandemic: systematic review and meta-analysis. BMJ Open Respir Res. 2023;10(1):e001674.
- Calzetta L, et al. Novel drug discovery strategies for chronic obstructive pulmonary disease: the latest developments. Expert Opin Drug Discov. 2025;20(5):683–692.
- Wise RA, et al. Clinical trial of losartan for pulmonary emphysema: pulmonary trials cooperative losartan effects on emphysema progression clinical trial. Am J Respir Crit Care Med. 2022;206(7):838–845.
- Polverino F, et al. Metformin: experimental and clinical evidence for a potential role in emphysema treatment. Am J Respir Crit Care Med. 2021;204(6):651–666.
- Ghorani V, et al. Experimental animal models for COPD: a methodological review. Tob Induc Dis. 2017;15(1):25.
- Negasi ZH, et al. Persistence of emphysema following cessation of cigarette smoke exposure requires a susceptibility factor. Am J Physiol Lung Cell Mol Physiol. 2024;326(4):L431–L439.
- Wright JL, Churg A. Animal models of COPD: barriers, successes, and challenges. Pulm Pharmacol Ther. 2008;21(5):696–698.
- Gordon SB, et al. Respiratory risks from household air pollution in low and middle income countries. Lancet Respir Med. 2014;2(10):823–860.
- Thilakaratne R, et al. Wildfires and the changing landscape of air pollution-related health burden in California. Am J Respir Crit Care Med. 2023;207(7):887–898.
- Doubleday A, et al. Mortality associated with wildfire smoke exposure in Washington state, 2006–2017: a case-crossover study. Environ Health. 2020;19(1):4.
- Aguilera R, et al. Wildfire smoke impacts respiratory health more than fine particles from other sources: observational evidence from Southern California. Nat Commun. 2021;12(1):1493.
- Adam M, et al. Adult lung function and long-term air pollution exposure. ESCAPE: a multicentre cohort study and meta-analysis. Eur Respir J. 2014;45(1):38–50.
- Park J, et al. Impact of long-term exposure to ambient air pollution on the incidence of chronic obstructive pulmonary disease: a systematic review and meta-analysis. Environ Res. 2021;194:110703.
- Ling SH, van Eeden SF. Particulate matter air pollution exposure: role in the development and exacerbation of chronic obstructive pulmonary disease. Int J Chron Obstruct Pulmon Dis. 2009;:233–243.View this article via: CrossRef Google Scholar
- Ko FW, Hui DS. Air pollution and chronic obstructive pulmonary disease. Respirology. 2012;17(3):395–401.
- Lwin KS, et al. Effects of desert dust and sandstorms on human health: a scoping review. Geohealth. 2023;7(3):e2022GH000728.
- Aghababaeian H, et al. Global health impacts of dust storms: a systematic review. Environ Health Insights. 2021;15:11786302211018390.
- Owen KP, et al. Marijuana: respiratory tract effects. Clin Rev Allergy Immunol. 2014;46(1):65–81.
- Tashkin DP. Effects of marijuana smoking on the lung. Ann Am Thorac Soc. 2013;10(3):239–247.
- Park JA, et al. Vaping and lung inflammation and injury. Annu Rev Physiol. 2022;84(1):611–629.
- McAlinden KD, et al. The rise of electronic nicotine delivery systems and the emergence of electronic-cigarette-driven disease. Am J Physiol Lung Cell Mol Physiol. 2020;319(4):L585–L595.
- Maziak W, et al. Waterpipe smoking: the pressing need for risk communication. Expert Rev Respir Med. 2019;13(11):1109–1119.
- Duan RR, et al. Air pollution and chronic obstructive pulmonary disease. Chronic Dis Transl Med. 2020;6(4):260–269.View this article via: PubMed Google Scholar
- Chen Z, et al. Health effects of exposure to sulfur dioxide, nitrogen dioxide, ozone, and carbon monoxide between 1980 and 2019: a systematic review and meta-analysis. Indoor Air. 2022;32(11):e13170.
- Wang M, et al. Association between long-term exposure to ambient air pollution and change in quantitatively assessed emphysema and lung function. JAMA. 2019;322(6):546–556.
- Idrose NS, et al. A review of the respiratory health burden attributable to short-term exposure to pollen. Int J Environ Res Public Health. 2022;19(12):7541.
- Tischer C, et al. Association between domestic mould and mould components, and asthma and allergy in children: a systematic review. Eur Respir J. 2011;38(4):812–824.
- Martinez FD. Early-life origins of chronic obstructive pulmonary disease. N Engl J Med. 2016;375(9):871–878.
- Pleasants RA, et al. Defining and targeting health disparities in chronic obstructive pulmonary disease. Int J Chron Osbtruct Pulmon Dis. 2016;11:2475–2496.
- Li K, et al. Mechanism study of social media overload on health self-efficacy and anxiety. Heliyon. 2023;10(1):e23326.
- Gimeno-Santos E, et al. Determinants and outcomes of physical activity in patients with COPD: a systematic review. Thorax. 2014;69(8):731–739.
- McNicholas WT, et al. Sleep disorders in COPD: the forgotten dimension. Eur Respir Rev. 2013;22(129):365–375.
- Hanson C, et al. Influence of diet and obesity on COPD development and outcomes. Int J Chron Obstruct Pulmon Dis. 2014;9:723–733.
- Nishida K, et al. Cigarette smoke disrupts monolayer integrity by altering epithelial ce ll-cell adhesion and cortical tension. Am J Physiol Lung Cell Mol Physiol. 2017;313(3):L581–L591.
- Ghosh B, et al. Strong correlation between air-liquid interface cultures and in vivo transcriptomics of nasal brush biopsy. Am J Physiol Lung Cell Mol Physiol. 2020;318(5):L1056–L1062.
- Aghapour M, et al. Airway epithelial barrier dysfunction in chronic obstructive pulmonary disease: role of cigarette smoke exposure. Am J Respir Cell Mol Biol. 2018;58(2):157–169.
- Gindele JA, et al. Intermittent exposure to whole cigarette smoke alters the differentiation of primary small airway epithelial cells in the air-liquid interface culture. Sci Rep. 2020;10(1):6257.
- Lin CR, et al. Impaired alveolar re-epithelialization in pulmonary emphysema. Cells. 2022;11(13):2055.
- Bauer RN, et al. Interaction with epithelial cells modifies airway macrophage response to ozone. Am J Respir Cell Mol Biol. 2015;52(3):285–294.
- Tadokoro T, et al. IL-6/STAT3 promotes regeneration of airway ciliated cells from basal stem cells. Proc Natl Acad Sci U S A. 2014;111(35):E3641–E3649.
- Huang SX, et al. Efficient generation of lung and airway epithelial cells from human pluripotent stem cells. Nat Biotechnol. 2014;32(1):84–91.
- Werder RB, et al. CRISPR interference interrogation of COPD GWAS genes reveals the functional significance of desmoplakin in iPSC-derived alveolar epithelial cells. Sci Adv. 2022;8(28):eabo6566.
- Conlon TM, et al. Inhibition of LTβR signalling activates WNT-induced regeneration in lung. Nature. 2020;588(7836):151–156.
- Switalla S, et al. Natural innate cytokine response to immunomodulators and adjuvants in human precision-cut lung slices. Toxicol Appl Pharmacol. 2010;246(3):107–115.
- Hisata S, et al. Reversal of emphysema by restoration of pulmonary endothelial cells. J Exp Med. 2021;218(8):e20200938.
- Borel F, et al. Editing out five Serpina1 paralogs to create a mouse model of genetic emphysema. Proc Natl Acad Sci U S A. 2018;115(11):2788–2793.
- D’Armiento J, et al. Collagenase expression in the lungs of transgenic mice causes pulmonary emphysema. Cell. 1992;71(6):955–961.
- Byers DE, et al. Long-term IL-33-producing epithelial progenitor cells in chronic obstructive lung disease. J Clin Invest. 2013;123(9):3967–3982.
- Tang J, et al. Impaired p65 degradation by decreased chaperone-mediated autophagy activity facilitates epithelial-to-mesenchymal transition. Oncogenesis. 2017;6(10):e387.
- Ye D, et al. Hedgehog-interacting protein orchestrates alveologenesis and protects against bronchopulmonary dysplasia and emphysema. Sci Adv. 2025;11(19):eadu2958.
- Yun JH, et al. Hedgehog interacting protein-expressing lung fibroblasts suppress lymphocytic inflammation in mice. JCI Insight. 2021;6(17):e144575.
- Albrecht RA, et al. Moving forward: recent developments for the ferret biomedical research model. mBio. 2018;9(4):e01113-18.
- Jacob S, Poddar S. Mucous cells of the tracheobronchial tree in the ferret. Histochemistry. 1982;73(4):599–605.
- Raju SV, et al. A ferret model of COPD-related chronic bronchitis. JCI Insight. 2016;1(15):e87536.
- Stanford D, et al. Airway remodeling in ferrets with cigarette smoke induced COPD using microCT imaging. Am J Physiol Lung Cell Mol Physiol. 2020;319(1):L11–L20.
-
Version history
- Version 1 (February 23, 2026): Electronic publication
Article tools
-
View PDF

- Download citation information
- Send a comment
- Terms of use
- Standard abbreviations
- Need help? Email the journal
Metrics
Go to
- Top
- Abstract
- The worldwide burden of chronic obstructive pulmonary disease
- COPD definition and subtypes
- “Pre-COPD” as an entity and available cohorts
- COPD-associated risk factors
- Gene-by-environment interaction
- Advances in preclinical COPD models
- In vitro and ex vivo models
- Animal COPD models
- Pathomechanisms of COPD
- Translational considerations
- Conclusions
- Funding support
- Acknowledgments
- Footnotes
- References
- Version history









