Cell biology
Abstract
At-home blood collection devices (ABCDs) can facilitate study participation for remote and rural cohorts. Previous studies used ABCDs to interrogate samples by proteomics and sequencing approaches. We wanted to address the question of whether this approach could be used to assess live immune cells with high-parameter flow cytometry to enable remote immune monitoring. We first compared blood from standard venipuncture with ABCD blood draws, followed by assessment of the impact of sample shipping on immune cell viability and phenotyping. We found that capillary blood collected with a Tasso+ device and concurrently drawn venipuncture blood samples had highly congruent immune cell composition and phenotype. Shipment of Tasso+ samples via the United States Postal Service altered the myeloid compartment, but T cell numbers, subsets, and phenotypes remained remarkably stable compared with non-shipped samples. Finally, we describe a flow cytometry analysis framework that allowed for direct sample comparison even when samples were stained and analyzed over a time period of 1.5 years. Overall, our data highlight the feasibility of using ABCDs combined with subsequent flow cytometry analysis for remote immune monitoring. Additionally, our study also identifies areas that could be improved to further promote the use of ABCDs for immune monitoring.
Authors
Andrew J. Konecny, Fang Yun Lim, Eva Domenjo-Vila, Erika Lovas, Rachel L. Blazevic, Louise E. Kimball, Michael Boeckh, Alpana Waghmare, Martin Prlic
Abstract
Current treatment protocols for most types of cancers require chemotherapeutic agents that are associated with significant side effects, including chemotherapy-induced peripheral neuropathy (CIPN). Currently, there are no effective CIPN prevention strategies, and current treatment approaches remain limited. The enzyme purine nucleoside phosphorylase (PNPase) actively modulates both oxidative injury and cellular damage. Here, we tested the hypothesis that the signs and symptoms of CIPN are due to a chemotherapy-induced dysregulation of the purine metabolome. We assessed the effect of PNPase inhibition on paclitaxel-induced (PAC-induced) CIPN. Female adult Sprague-Dawley rats were treated with PAC and randomized to oral treatment with either the PNPase inhibitor 8-aminoguanine (8-AG) or its vehicle. Some rats were injected with shRNA against PNPase prior to PAC injections. PAC-treated rats exhibited multiple abnormalities: mechanical allodynia and changes in damaging purines, intraepidermal nerve fiber (IENF) density, and signaling cascades involved in mitochondrial disruption and axonal damage. Inhibition of PNPase improved behavioral function (mechanical allodynia), rescued the loss/damage of IENF, and normalized markers for mitochondrial dysfunction and nerve damage. These findings support the hypothesis that inhibition of PNPase prevented (and potentially reversed) CIPN through several mechanisms that included a reduction in neuronal damage and development of mechanical allodynia.
Authors
Lori A. Birder, Amanda Wolf-Johnston, Jonathan Franks, Mara L.G. Sullivan, Simon C. Watkins, Anthony J. Kanai, Vladimir B. Ritov, Edwin K. Jackson
Abstract
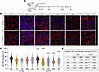
Chronic neuropathic pain is frequently comorbid with anxiety disorders, yet the neural circuits underlying this interaction remain poorly defined. The parafascicular nucleus of the thalamus (PF) integrates nociceptive and affective signals, but its specific regulatory mechanisms in pain-anxiety comorbidity are not well known. Using spared nerve injury (SNI) model mice, we combined viral neural tracing, chemogenetics, pharmacology, and electrophysiology to dissect the locus coeruleus (LC)-PF neural pathway. Viral tracing revealed monosynaptic projections from norepinephrinergic (NEergic) neurons in the dorsal LC to calcium/calmodulin dependent protein kinase IIα (CaMKIIα)- immunopositive neurons within the PF. Chemogenetic inhibition/activation of this pathway were performed in naïve and SNI mice, alongside intra-PF microinjection of the alpha-2 adrenergic receptor (ADRA2) antagonist yohimbine. Behavioral tests assessed mechanical/thermal hypersensitivity and anxiety-like behaviors. Results showed that 92.1% of PF-projecting LC neurons were NEergic, with 70.1% localized dorsally. Chemogenetic inhibition of LCNE-PFCaMKIIα neural pathway significantly alleviated both acute-phase mechanical hypersensitivity (< 7 days post-surgery) and chronic-phase anxiety-like behaviors in SNI mice, while activation of this pathway induced pain sensitization and anxiety-like behaviors in naïve mice. Intra-PF yohimbine reversed SNI-induced allodynia and anxiety-like behaviors. Electrophysiology confirmed yohimbine increased PF neuronal intrinsic excitability. These results suggest that the LCNE-PFCaMKIIα neural pathway promotes neuropathic pain and comorbid anxiety via ADRA2-mediated suppression of PF neuronal activity. Targeted inhibition of this circuit may represent a therapeutic strategy for pain-related affective disorders.
Authors
Zhong-Yi Liu, Fei Li, Li-Ming Liu, Yao-Hua Liu, Jia Li, Zi-Ang Li, Jin Cheng, Tian-Yu Zhao, Hui-Min Tian, Dong-Ning Li, Sha-Sha Tao, Hui Li, Fen-Sheng Huang, Yun-Qing Li
Abstract
Dedifferentiated liposarcoma (DDLS), myxofibrosarcoma (MFS), and undifferentiated pleomorphic sarcoma (UPS) are the most common types of genetically complex sarcoma. There is an urgent need to develop effective targeted therapy for these deadly sarcoma types. Despite their genetic complexity, these sarcomas share genomic alterations causing PI3K/Akt/mTOR and MAPK pathway activation, and both pathways control translation mediated by the RNA helicase eIF4A. We therefore investigated eIF4A inhibition as a therapeutic strategy. The eIF4A inhibitor CR-1-31B effectively suppressed tumor growth and induced apoptosis in DDLS, MFS, and UPS patient-derived cell lines and mouse xenografts. Transcriptome-scale ribosome footprinting identified eIF4A-dependent mRNAs such as the Hippo pathway transcriptional coactivators YAP1 (YAP) and WWTR1 (TAZ). Combined knockdown of YAP and TAZ induced apoptosis in DDLS, MFS, and UPS cell lines, and their ectopic expression partially rescued cells from apoptosis induced by CR-1-31B. Genomic analysis of patient tumors revealed that YAP and WWTR1 were frequently amplified or gained in DDLS, MFS, and UPS and were associated with worse clinical outcomes. Together, our findings identify a new strategy for targeting the Hippo pathway in incurable forms of sarcoma based on inhibition of eIF4A-dependent translation of the key oncogenic transcription factors YAP and TAZ.
Authors
Young-Mi Kim, Prathibha Mohan, Urmila Sehrawat, Evan Seffar, Rafaela Muniz De Queiroz, Kalyani Chadalavada, Nikita Persaud, Tomoyo Okada, Anirudh Kulkarni, Jianan Lin, Nathalie Lailler, Shaleigh Smith, Bhumika Jadeja, Nicholas D. Socci, Zhengqing Ouyang, Hans-Guido Wendel, Samuel Singer
Abstract
Spinocerebellar Ataxia Type 14 (SCA14) is an autosomal dominant neurodegenerative disease caused by mutations in the gene encoding protein kinase C gamma (PKCγ), a Ca2+/diacylglycerol (DG)-dependent serine/threonine kinase dominantly expressed in cerebellar Purkinje cells. These mutations impair autoinhibitory constraints to increase the basal activity of the kinase, resulting in deficits in the cerebellum that are not observed upon simple deletion of the gene, and severe ataxia. To better understand the impact of aberrant PKCγ signaling in disease pathology, we developed a knock-in murine model of the SCA14 mutation ΔF48 in PKCγ. This fully-penetrant mutation is severe in humans and is mechanistically informative as it has high basal activity but is unresponsive to agonist stimulation. Genetic, behavioral, and molecular testing revealed that ΔF48 PKCγ mice have ataxia-related phenotypes and an altered cerebellar phosphoproteome driven primarily by enhanced Ca2+/calmodulin-dependent Kinase II (CaMKII) signaling, effects that were more severe in male mice. Analysis of existing human data revealed that SCA14 has a significantly earlier age of onset for males compared with females. Data from this clinically relevant mutation suggested that enhanced basal activity of PKCγ is sufficient to cause ataxia and that treatment strategies to modulate aberrant PKCγ may be particularly beneficial in males.
Authors
Sarah A. Wolfe, Yuliang Ma, Tomer M. Yaron-Barir, Carly Chang, Caila A. Pilo, Majid Ghassemian, Amanda J. Roberts, Sang Ryeul Lee, Benjamin A. Henson, Kristen Jepsen, Jared L. Johnson, Lewis C. Cantley, Susan S. Taylor, George Gorrie, Alexandra C. Newton
Abstract
Thoracic Aortic Aneurysm and Dissections (TAAD) is a progressive dilation of the aortic wall associated with degradation of the extracellular matrix (ECM), cystic medial degeneration, smooth muscle cell (SMC) dysfunction, and rarefaction. TAAD etiology and pathogenesis suggest that alteration of mechanical force propagation may contribute to SMC dysfunction. This study aims to determine the role of SMC focal adhesion proteins, which are key components of force transmission, in TAAD pathogenesis. scRNAseq analysis of human TAA aortas showed reduced expression of intracellular focal adhesion components, including PTK2 (FAK), VCL, ILK, and TES transcripts, in SMCs. Additionally, protein levels of FAK, ILK, and VCL were decreased in the aorta of patients with TAA. SMC-specific Ptk2, Vcl, and Ilk knockout mice treated with β-Aminopropionitrile (BAPN) exhibited increased mortality, aortic dilation, ECM breakdown, and SMC loss. Mechanistically, knocking down FAK, ILK, and VCL exacerbated gliotoxin-induced SMC anoikis, whereas overexpressing full-length wild-type (WT) and dead-kinase FAK conferred resistance to apoptosis and cell detachment, indicating that FAK's protective effects depend on its expression rather than its enzymatic activity. Inhibition of FAK kinase activity did not affect SMC apoptosis in vitro or aortic dilation in vivo. Our findings demonstrated that the expression of focal adhesion proteins protects against TAAD progression and SMC anoikis independently of FAK kinase activity.
Authors
Zhenyuan Zhu, Mingjun Liu, Jianxin Wei, Deepa Suryanarayan, Parya Behzadi, Robert Edgar, Julie A. Phillippi, Cynthia St. Hilaire, Cristina Espinosa-Diez, Delphine Gomez
Abstract
Glioblastoma (GBM) is the most malignant primary brain tumor. The presence of glioma stem/initiating cells (GICs) is known to cause strong treatment resistance; therefore, GICs are a major target for GBM therapy, although there are no therapies targeting GICs clinically. To identify novel treatments for GBMs, we performed drug repositioning screening using GICs and identified T-type calcium channel blocker lomerizine—a migraine prophylactic drug. Lomerizine inhibited proliferation, migration, invasion, and cell cycle progression and induced apoptosis in GICs and differentiated glioma cells. Lomerizine had antitumor effects by inactivating STAT3 in all cell lines. Furthermore, lomerizine also dephosphorylated AKT and ERK only in GICs and strong tumor suppressive ability. Lomerizine also reduced tumor volume and prolonged overall survival in vivo. Based on our data from in vitro and in vivo experiments, lomerizine has potential as a novel GBM therapeutic agent targeting against both GICs and differentiated glioma cells and could benefit for GBM patients.
Authors
Toshiya Ichinose, Sho Tamai, Nozomi Hirai, Takashi Maejima, Kosuke Nambu, Hemragul Sabit, Shingo Tanaka, Masashi Kinoshita, Masahiko Kobayashi, Michihiro Mieda, Atsushi Hirao, Mitsutoshi Nakada
Abstract
Limb-girdle muscular dystrophy R2 (LGMD R2) is an autosomal recessive disorder caused by dysferlin deficiency, leading to progressive muscle weakness and wasting. The lack of reliable clinical biomarkers has limited disease monitoring and therapeutic evaluation. Here, we identified Disabled-2 (DAB2) as a molecular and clinical indicator of disease state in LGMD R2. Transcriptomic profiling revealed a significant upregulation of DAB2 in induced pluripotent stem cell–derived (iPSC-derived) myotubes from patients, a finding validated in muscle biopsies from 14 dysferlin-deficient individuals and in dysferlin-deficient Bla/J mice, where DAB2 levels increased with disease progression. Importantly, AAV-mediated expression of full-length dysferlin restored DAB2 levels, supporting its value as a dynamic readout of disease activity for both disease monitoring and therapeutic response. Given the established role of DAB2 in clathrin-mediated endocytosis, particularly in LDL receptor internalization and cholesterol homeostasis, and the pathological lipid accumulation reported in LGMD R2, we investigated its contribution to lipid dysregulation. High DAB2 expression paralleled lipid deposition in patient muscles, iPSC-derived myotubes, and mouse tissue, whereas siRNA-mediated DAB2 knockdown reduced lipid accumulation in LGMD R2 myotubes. Collectively, these findings suggest that DAB2 functions as a mechanistic link between dysferlin deficiency, altered lipid handling, and disease severity, and they highlight its potential as a prognostic marker and therapeutic response measure for LGMD R2.
Authors
Celine Bruge, Nathalie Bourg, Emilie Pellier, Quentin Miagoux, Manon Benabides, Noella Grossi, Hassan Hayat, Margot Jarrige, Helene Polveche, Valeria Agostini, Anthony Brureau, Stephane Vassilopoulos, Teresinha Evangelista, Gorka Fernández-Eulate, Tanya Stojkovic, Isabelle Richard, Xavier Nissan
Abstract
Modulation of miRNA expression in glomerular cells is associated with renal disease. Here, we investigated the role of miR-93-5p in mitigating glomerular damage in Alport syndrome and whether the disease-modifying activity of extracellular vesicles from human amniotic fluid stem cells (hAFSC-EVs) is mediated by their miR-93-5p cargo. We identified downregulation of miR-93-5p specifically in glomerular endothelial cells in Alport syndrome along disease progression. Silencing of miR-93-5p in hAFSC-EVs changed the transcriptomic and proteomic profile, regulating EV disease-modifying activity. Compared with naive hAFSC-EVs, silenced hAFSC-EVs did not rescue glomerular endothelial function in vitro and did not restore kidney function in vivo. We established that hAFSC-EVs regulate VEGFR1 and VEGFR2 signaling by miR-93-5p cargo transfer, highlighting that miR-93-5p can restore glomerular endothelial cell biology. Spatial transcriptomics analysis of hAFSC-EV–injected kidneys showed that these EVs can reverse pathways altered during disease progression by stimulating proregenerative processes, specifically in the glomerulus, by regulating miR-93-5p targets. Alteration of glomerular endothelial cell transcriptomics and miR-93-5p targets was also confirmed in biopsies of patients with Alport syndrome using spatial molecular imaging. We demonstrated the critical role of miR-93-5p in glomerular endothelial cells and the capability of hAFSC-EVs to regulate miR-93-5p and its targets in Alport syndrome.
Authors
Charmi Dedhia, Valentina Villani, Xiaogang Hou, Paolo Neviani, Geremy Clair, Mohammadreza Kasravi, Cristina Grange, Paolo Cravedi, Paola Aguiari, Velia Alcala, Giuseppe Orlando, Xue-Ying Song, Jonathan E. Zuckerman, Roger E. De Filippo, Stefano Da Sacco, Sargis Sedrakyan, Benedetta Bussolati, Laura Perin
Abstract
Thyroid hormone signaling is an essential regulator of skeletal muscle development, function, and metabolism, yet the specific signaling pathways required for muscle regeneration are not yet defined. We used scRNA-seq and the FUCCI (fluorescent ubiquitination-based cell cycle indicator) reporter mouse model to examine how hypothyroidism impacts repair processes after cardiotoxin-induced injury in mice. During regeneration, and up to 2 months after injury, hypothyroid muscles displayed smaller myofibers and a shift to slower oxidative fiber types. scRNA-seq of tibialis anterior muscle during regeneration revealed that hypothyroidism reduced myogenic-lineage diversity. Cell cycle analysis confirmed delayed cell cycle progression at 5 and 14 days after injury, with skeletal muscle stem cells stalled at the G1/S transition, hindering differentiation. Transcriptomic data revealed altered nonmyogenic dynamics, including elevated activated fibro-adipogenic progenitors (FAPs) early in repair and persistent proinflammatory macrophages. Integrative regulon and ligand-receptor analysis further demonstrated that triiodothyronine acted through dual modes: a direct transcriptional control of myogenic cell cycle and oxidative programs and an indirect paracrine remodeling mediated by FAP and immune signaling networks. This study identified what we believe to be novel effects of hypothyroidism on myogenic heterogeneity and impaired tissue repair, offering insights into muscle-wasting mechanisms relevant to hypothyroidism-associated myopathy and sarcopenia.
Authors
Paola Aguiari, Valentina Villani, Yan-Yun Liu, Gianni Carraro, Gregory A. Brent, Laura Perin, Anna Milanesi
No posts were found with this tag.