Dermatology
Abstract
BACKGROUND Icotrokinra is the first and only targeted oral peptide that selectively binds the IL-23 receptor with high affinity to precisely inhibit IL-23 signaling. Icotrokinra demonstrated high rates of complete skin clearance and durable disease control in the phase IIb trial, FRONTIER-1, and its long-term extension, FRONTIER-2, in participants with moderate-to-severe plaque psoriasis. This study evaluated systemic and skin pharmacodynamic response of icotrokinra and its relationship to clinical response in FRONTIER participants.METHODS FRONTIER-1 participants received icotrokinra or placebo for 16 weeks. FRONTIER-2 followed participants for up to 1 year of treatment; placebo participants transitioned to icotrokinra after week 16. Systemic pharmacodynamic changes were assessed in serum through week 52. Skin pharmacodynamic changes were assessed using transcriptomic analysis of skin biopsies and protein quantification in tape-strip samples through week 16.RESULTS Icotrokinra dose-dependently reduced serum levels of the IL-23/IL-17 axis and psoriasis disease biomarkers through week 52, with maximal reductions observed with the highest 100 mg twice-daily dose. Proteomic analyses showed icotrokinra selectively blocked IL-23–driven inflammation without broader impacts on circulating proteins, including serum IL-23 levels. Sixteen weeks of icotrokinra, but not placebo, reduced expression of psoriasis-associated genes in lesional skin. Icotrokinra treatment also reduced psoriasis-relevant proteins in week 16 lesional skin tape-strips to levels comparable to nonlesional samples.CONCLUSION Icotrokinra induced a dose-dependent pharmacodynamic response, with early (week 4) and sustained (week 52) reductions in biomarkers of IL-23 pathway activation and psoriasis disease severity, which correlated with clinical response.TRIAL REGISTRATION ClinicalTrials.gov: NCT05223868, NCT05364554.FUNDING Johnson & Johnson.
Authors
David Strawn, James G. Krueger, Robert Bissonnette, Kilian Eyerich, Laura K. Ferris, Amy S. Paller, Andreas Pinter, Dylan Richards, Elizabeth Y. Chen, Kate Paget, Daniel Horowitz, Roohid Parast, Joshua J. Rusbuldt, Jocelyn Sendecki, Sunita Bhagat, Lynn P. Tomsho, Ching-Heng Chou, Marta E. Polak, Brice E. Keyes, Emily Bozenhardt, Yuan Xiong, Wangda Zhou, Cynthia DeKlotz, Paul Newbold, Dawn M. Waterworth, Megan Miller, Takayuki Ota, Ya-Wen Yang, Monica W.L. Leung, Lloyd S. Miller, Carolyn A. Cuff, Bradford McRae, Darren Ruane, Arun K. Kannan
Abstract
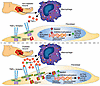
Uncovering the early interactions and spatial distribution of dermal fibroblasts and immune cells in treatment-naïve diffuse cutaneous systemic sclerosis (dcSSc) patients is critical to understanding the earliest events of skin fibrosis. We generated an integrated multiomic dataset of early, treatment-naïve dcSSc skin. Skin biopsies were analyzed by single-nuclei multiome sequencing (snRNA-seq and snATAC-seq) and two different spatial transcriptomic methods to comprehensively determine the molecular changes in these individuals. We identified an immunomodulatory niche within the papillary, hypodermis, and vascular regions that are enriched for activated myeloid cells and fibroblasts characterized by expression of genes such as CXCL12, APOE, and C7. Pathway analyses showed significant enrichment of PI3K-AKT-mTOR signaling pathway expression in these cellular niches, driven by profibrotic growth factor signaling networks. Macrophage subclustering showed SSc-specific macrophage activation of the IL6-JAK-STAT signaling and the enrichment of oxidative phosphorylation pathways. Ligand-receptor analysis revealed that SSc macrophages secrete PDGF and TGF-β to activate the SSc-dominant fibroblast subclusters. Spatial transcriptomic analyses showed monocyte-derived MRC1+ macrophages express PDGF near PDGFRhighTHY1high fibroblasts. Multi-omic data integration and spatial transcriptomic neighborhood analysis revealed the co-localization of fibroblasts, macrophages, and T cells around the vasculature. These data suggest that interactions between activated immune cells and immunomodulatory fibroblasts around vascular niches are an early event in scleroderma pathogenesis.
Authors
Helen C. Jarnagin, Rezvan Parvizi, Zhiyun Gong, Rosemary Gedert, Xianying Xing, Lam (Alex) C. Tsoi, Rachael Bogle, Madeline J. Morrisson, Laurent Perreard, Patricia A. Pioli, Fred Kolling IV, Johann E. Gudjonsson, Dinesh Khanna, Michael L. Whitfield
Abstract
Oral lichen planus (OLP) is a recalcitrant inflammatory disease with potential for malignant transformation, involving a cytotoxic CD8+ T cells-mediated basal keratinocyte apoptosis. However, it lacks an appropriate mouse model for study. Here we developed an OLP-like mouse model using topical oxazolone to induce a delayed-type hypersensitivity-mediated oral lichenoid reaction. Histological and ultrastructural analysis confirmed hallmark pathological features of OLP, including band-like CD8+ T cell infiltration and basal cell damage, and the presence of Civatte bodies. Comparative transcriptomic analysis revealed significant similarity between RNA-seq profiles of the mouse model and human OLP lesions, highlighting shared upregulated genes and enriched pathways, particularly those related to IFN-γ signaling and cytotoxic T cell activity. Functional studies demonstrated that the OLP phenotype depended on IFN-γ, with local priming by IFN-γ intensifying the disease through upregulation of major histocompatibility complex class I. Additionally, the absence of Langerhans cells exacerbated disease severity in vivo. Therapeutic evaluation showed that the JAK inhibitors baricitinib and ruxolitinib effectively reduced disease burden and provided mechanistic insights. In conclusion, this OLP-like mouse model recapitulates key immunopathological and transcriptomic features of human OLP, offering a robust platform for dissecting disease mechanisms and evaluating novel therapeutic strategies.
Authors
Zhenlai Zhu, Tinglan Yang, Peng Peng, Kang Li, Wen Qin, Chen Zhang, Shuyan Wang, Yuanyuan Wang, Minghui Wei, Erle Dang, Meng Fu, Hao Guo, Wen Yin, Shuai Shao, Qing Liu
Abstract
Epigenetic macromolecular enzyme complexes tightly regulate gene expression at the chromatin level and have recently been found to colocalize with RNA splicing machinery during active transcription; however, the precise functional consequences of these interactions are uncertain. Here, we identify unique interactions of the CoREST repressor complex (LSD1-HDAC1-CoREST) with components of the RNA splicing machinery and their functional consequences in tumorigenesis. Using mass spectrometry, in vivo binding assays, and cryo-EM we find that CoREST complex-splicing factor interactions are direct and perturbed by the CoREST complex selective inhibitor, corin, leading to extensive changes in RNA splicing in melanoma and other malignancies. Moreover, these corin-induced splicing changes are shown to promote global effects on oncogenic and survival-associated splice variants leading to a tumor-suppressive phenotype. Using machine learning models, MHC IP-MS, and ELISpot assays we identify thousands of neopeptides derived from unannotated splice sites which generate corin-induced splice-neoantigens that are demonstrated to be immunogenic in vitro. Corin is further shown to reactivate the response to immune checkpoint blockade, effectively sensitizing tumors to anti-PD1 immunotherapy. These data position CoREST complex inhibition as a unique therapeutic opportunity which perturbs oncogenic splicing programs while also creating tumor-associated neoantigens that enhance the immunogenicity of current therapeutics.
Authors
Robert J. Fisher, Kihyun Park, Kwangwoon Lee, Katarina Pinjusic, Allison Vanasse, Christina S. Ennis, Parisa Farokh, Scott B. Ficarro, Jarrod A. Marto, Hanjie Jiang, Eunju Nam, Stephanie Stransky, Joseph Duke-Cohan, Melis A. Akinci, Anupa Geethadevi, Eric Raabe, Ana Fiszbein, Shadmehr Demehri, Simone Sidoli, Chad W. Hicks, Derin B. Keskin, Catherine J. Wu, Philip A. Cole, Rhoda M. Alani
Abstract
Fibroblast to myofibroblast transition is a critical event required for effective tissue repair. In pathologic wound repair processes, such as type 2 diabetes (T2D), fibroblast to myofibroblast transition is impaired. The exact factors that control this transition in wounds are unclear. Here, using human tissue and murine transgenic models, we show that the histone methyltransferase SETDB2 is elevated in diabetic wound fibroblasts and TNF-α represses fibroblast to myofibroblast transition via Setdb2. We identified that TNF-α increases Setdb2 in fibroblasts via a JAK1,3/STAT3 signaling pathway, where pharmacologic or genetic manipulation of this pathway altered Setdb2 in fibroblasts. We also found that fibroblasts treated with pro-inflammatory macrophage supernatants displayed increased Setdb2 and downregulated myofibroblast genes; inhibition of the TNF-α receptor reduced the upregulation of Setdb2. In diabetes, we showed that TNF-α signaling was increased in wound fibroblasts, which functions to increase Setdb2 expression and represses fibroblast to myofibroblast transition. Fibroblast-specific knockdown of SETDB2 and therapeutic inhibition of JAK1,3/STAT3 improved diabetic wound repair, where wound fibroblasts expressed increased myofibroblast genes. This study is the first to our knowledge to identify an epigenetic mechanism for reduced fibroblast to myofibroblast transition in diabetic wounds. Therapeutic targeting of the TNF-α/STAT3/SETDB2 axis in wound fibroblasts may improve diabetic wound healing.
Authors
Tyler M. Bauer, Kevin D. Mangum, Samuel D. Buckley, James Shadiow, Amrita D. Joshi, Christopher O. Audu, Jadie Y. Moon, Lindsey D. Hughes, Rachel Bogel, Lam C. Tsoi, Qinmennge Li, He Zhang, Steven Kunkel, Johann E. Gudjonsson, Frank M. Davis, Katherine A. Gallagher
Abstract
Authors
Zhehao Tan, Gio Wu, Daniela Salgado Figueroa, Paramita Dutta, Zachary Jaeger, Marissa Mazurie, David Schairer, Dawn Eichenfield, Wynnis L. Tom, Lauren Galli, Lawrence Eichenfield, Bob Geng, Brian Hinds, Hal M. Hoffman, Lori Broderick, Ben Croker, Ferhat Ay, Reid Oldenburg
Abstract
Patients with cutaneous T cell lymphoma (CTCL) experience high morbidity and mortality due to S. aureus skin infections and sepsis, but the underlying mechanisms remain unclear. We have previously identified high levels of LAIR2, a decoy protein for the inhibitory receptor LAIR1, in advanced CTCL. Mice lack a LAIR2 homolog, so we used Lair1 knock-out (KO) mice to model LAIR2 overexpression. In a model of S. aureus skin infection, Lair1 KO mice had significantly larger abscesses and areas of dermonecrosis compared to WT despite similar bacterial burdens. Lair1 KO exhibited a pattern of increased inflammatory responses in infection and sterile immune stimulation, with increased production of proinflammatory cytokines and myeloid chemokines, neutrophil ROS, and collagen/ECM pathway proteins, including collagens and complement factors. These findings support the notion that loss of LAIR1 signaling causes an excessive inflammatory response that exacerbates tissue damage and does not improve infection control. Underscoring the clinical relevance of our findings, CTCL skin lesions exhibited similarly increased expression in cytokine and collagen/ECM remodeling pathways, suggesting that high levels of LAIR2 promote excessive inflammatory tissue damage and compromise host defense against S. aureus infection. LAIR signaling represents a promising target for therapeutic development in CTCL and other inflammatory diseases.
Authors
Hannah K. Dorando, Evan C. Mutic, Kelly L. Tomaszewski, Yulia Korshunova, Ling Tian, Mellisa K. Stefanov, Chaz C. Quinn, Deborah J. Veis, Juliane Bubeck Wardenburg, Amy C. Musiek, Neha Mehta-Shah, Jacqueline E. Payton
Abstract
Mammalian skin wounds typically heal with a scar, characterized by fibrotic tissue that disrupts original tissue architecture and function. Therapies that limit fibrosis and promote regenerative healing remain a major unmet clinical need. Rosemary extract, particularly in the form of topical oils and creams, has gained widespread public attention for its purported wound-healing properties. However, its efficacy and mechanism of action remain poorly understood. We show in adult wound healing mouse models that an ethanol-based rosemary extract accelerates the speed of wound healing and mitigates fibrosis. Mechanistically, we identify that carnosic acid, a major bioactive component of rosemary leaves, activates the TRPA1 nociceptor on cutaneous sensory neurons to enhance tissue regeneration. Mice lacking TRPA1 in sensory neurons do not exhibit these pro-regenerative responses, confirming its role as a critical mediator. Together, these findings suggest that topical rosemary extract may represent an effective and accessible therapeutic approach to improve skin repair outcomes.
Authors
Emmanuel Rapp, Jiayi Pang, Borna Saeednia, Stephen Marsh Prouty, Christopher A. Reilly, Thomas H. Leung
Abstract
Impaired wound healing poses a major and increasingly frequent health problem. Among the key players in the healing process are fibroblasts, but their metabolic profile in healing wounds is largely unknown. Using a combination of transcriptomics, targeted proteomics and metabolomics, we identified retinol metabolism as a top regulated pathway in wound fibroblasts. This is functionally relevant, since even a mild retinol deficiency caused a delay in wound closure and re-epithelialization, which mainly resulted from misdirected keratinocyte migration on the new granulation tissue. Quantitative proteomics identified integrin alpha 11 (Itga11) as a less abundant protein in wounds of mice subjected to a retinol-deficient diet. Reduced levels of this fibroblast-specific protein likely altered the granulation tissue matrix, which in turn affected re-epithelialization. These results provide a comprehensive overview on the transcriptome, proteome and metabolome of wound fibroblasts and identify retinol metabolism in fibroblasts as a key regulator of tissue repair.
Authors
Till Wüstemann, Elizabeta Madzharova, Mateusz S. Wietecha, Norbert B. Ghyselinck, Marcus Höring, Gerhard Liebisch, Nicola Zamboni, Ulrich auf dem Keller, Sabine Werner
Abstract
Impairment of desmosomal cell-cell adhesion leads to life-threatening diseases such as the autoimmune skin blistering disorder pemphigus vulgaris (PV). Disease management strategies that stabilize intercellular adhesion, in addition to the existing immunosuppression therapies, may result in improved clinical outcomes. Previous findings showed that the serine protease inhibitor SERPINB5 promotes intercellular adhesion by binding to and regulating the localization of the desmosomal adapter molecule desmoplakin (DSP) at the plasma membrane. We here show that SERPINB5 overexpression prevents PV-IgG-mediated loss of cell-cell adhesion and DSP dissociation from the cell membrane. We mechanistically demonstrate that SERPINB5 loss deregulates TGF-β signalling, a pathway known to destabilize DSP in keratinocytes. TGF-β signalling was also activated in skin biopsies of PV patients and keratinocytes treated with PV autoantibodies, suggesting a contribution to disease. Inhibition of TGF-β signaling ameliorated PV-IgG-mediated loss of cell-cell adhesion, increased DSP membrane expression, and prevented PV-IgG-induced blister formation in a human ex-vivo skin model. Together, SERPINB5 modulates DSP and intercellular adhesion through the regulation of TGF-β signalling. Further, TGF-β signalling was identified as a potential target for pemphigus treatment.
Authors
Maitreyi Rathod, Mariam Petrosyan, Aude Zimmermann, Maike Märker, Tobias Gosau, Henriette Franz, Tomás Cunha, Dario Didona, Michael Hertl, Enno Schmidt, Volker Spindler
No posts were found with this tag.